Who should consider surgery for long-term weight loss

A 2018 survey found that almost half of U.S. adults weigh much more than they should. This “new normal” may be widely accepted, but it’s not healthy. The extra pounds put you at risk by triggering the development of risk factors for cardiovascular disease.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
If you have struggled and failed to lose weight, it may be time to consider bariatric surgery.
“Diet alone — although sometimes effective — generally results only in temporary weight loss. The two most common forms of bariatric surgery — laparoscopic sleeve gastrectomy and laparoscopic Roux-en-Y gastric bypass — have been shown to be more effective in losing weight and keeping it off, resolving weight-associated comorbidities and lowering cardiovascular risk,” says Raul J. Rosenthal, MD, Director of Cleveland Clinic Florida’s Bariatric and Metabolic Institute.
We may notice weight gain in our belly, waist, hips or neck, but it’s what we can’t see that increases our cardiovascular risk. That’s because in addition to accumulating under our skin, fat deposits grow inside our abdomen, between our heart and the sac surrounding it and inside our artery walls. These internal fat deposits accelerate the development of atherosclerosis, type 2 diabetes, hypertension and sleep apnea — all of which increase the risk of heart attack and stroke.
The risks of being overweight extend beyond the heart and vascular system, as well. “More than 50 percent of cancers in women are related to obesity,” says Dr. Rosenthal.
The majority of patients who undergo weight-loss surgery are women. The procedures restrict the amount of food that can be eaten or shorten the digestive tract to limit the calories that are absorbed. Either way, extra pounds disappear.
In six to 12 months, you lose 60
to 80 percent of your excess body
weight.
The impact can be substantial:
These improvements actually reverse detrimental aging of the blood vessels. In one study, the mean age of the participants was 52, but their blood vessels were those of a 69-year-old. One year after bariatric surgery, their vascular age was the same as their chronological age: 53. The surgery made their blood vessels seven years younger. This beneficial effect significantly lowers the risk of heart attack and stroke.
“The laparoscopic sleeve gastrectomy and laparoscopic Roux-en-Y gastric bypass procedures are equally effective in improving the age of the heart and blood vessels and reducing cardiovascular risk 12 months after the surgery,” says Dr. Rosenthal. “We usually recommend the gastric sleeve because it is less likely to cause problems later on.”
Anyone with a body-mass index (BMI) of 35-40 and other serious cardiovascular risk factor who has been unable to lose a substantial amount of weight on their own should consider weight-loss surgery.
“You must be ready to make lifestyle changes, which will be absolutely necessary to long-term success,” says Dr. Rosenthal.
This article originally appeared in Cleveland Clinic Heart Advisor.
Learn more about our editorial process.

Having underweight, having overweight and having obesity can be dangerous for your heart
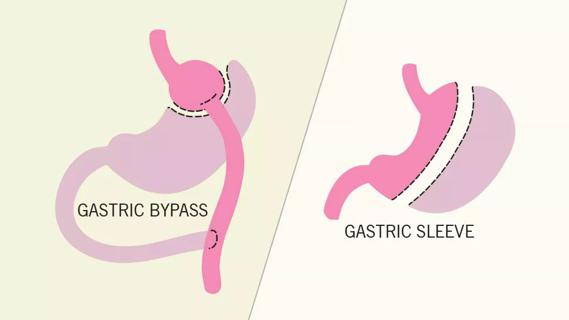
Gastric bypass and sleeve gastrectomy are different procedures that offer similar benefits, including significant weight loss

Your weight-loss plateau isn’t a question of willpower, it’s your body fighting back

The yellow-colored spice does more than add flavor to your meals

Your food choices can have a profound impact on how long you’ll live

What you should know about bariatric surgery
Adults at low risk for heart disease may not need them

Realistic expectations are key to weight-loss success

Your metabolism may torch 1,300 to 2,000 calories daily with no activity

A gentle touch in all the right places may help drain your sinuses