You know heartburn all too well. Maybe it happens after too much salsa. Or after any big meal. Or when you lie down.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
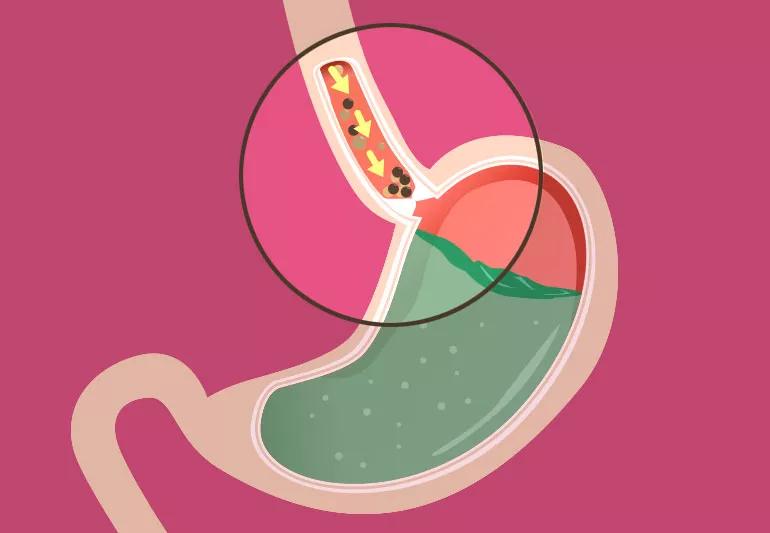
Acid, partly digested food and other stomach contents creep up into your esophagus, causing the inside of your chest to burn like a jalapeño.
Most of the time it’s just acid reflux, or gastroesophageal reflux disease (GERD), which affects about 1 in 5 Americans. But for about 1 in 100,000 Americans per year, it’s actually a different condition, called achalasia.
Knowing which condition you have is important because acid reflux and achalasia are treated differently. If untreated (or treated incorrectly), you may continue to suffer with symptoms — and continued damage to your esophagus can become irreversible.
Both acid reflux and achalasia happen when the “door” from your esophagus to your stomach is broken. With acid reflux, the door doesn’t close when it should. With achalasia, the door doesn’t open when it should.
The door is called the lower esophageal sphincter. It’s a ring of muscle that should be squeezed shut most of the time. When you swallow, it should relax and open to let food into your stomach and then squeeze shut again.
“You may experience a small amount of acid reflux during this process,” says gastroenterologist Scott Gabbard, MD. “Up to one hour of acid reflux per day is actually considered normal.”
If you have achalasia, your lower esophageal sphincter doesn’t open. Whatever you swallow gets stuck at the bottom of your esophagus, which can cause heartburn, just like acid reflux.
It’s not clear what causes achalasia, but it has to do with the nerves that tell the sphincter when to open. Something causes those nerves to disappear, possibly an immune system response to a virus.
Because the conditions have similar symptoms, it’s not uncommon for people with achalasia to be treated for acid reflux — sometimes for years.
“If stomach contents come back up after you’ve swallowed them, most of the time it’s acid reflux,” says Siva Raja, MD, PhD, Surgical Director of the Center for Esophageal Diseases. “But if you have difficulty swallowing and feel like your food gets stuck in your esophagus, you should be tested to rule out conditions like achalasia and even esophageal cancer.”
A gastroenterologist may do an endoscopy to look in your esophagus or conduct a barium swallow or esophageal manometry to see how your esophagus is working.
Feeling like your food doesn’t go down to your stomach can be a sign of achalasia, but not always, says Dr. Gabbard. Acid reflux can cause ulcers at the bottom of your esophagus, which can cause food to get stuck, too.
If you have acid reflux, treatments usually involve:
If you have achalasia, acid reflux treatments typically won’t relieve your symptoms. Instead, your doctor may recommend:
Because achalasia is so rare, you may need to be referred to an experienced medical center for accurate diagnosis and treatment.
“I recommend different treatments for different patients,” says Dr. Gabbard. “The same treatment isn’t best for everyone.”
If you have heartburn and regurgitation once a week or less, try lifestyle changes and over-the-counter acid reflux medications first. If your symptoms don’t improve, see a doctor to be evaluated for achalasia or other conditions.
See a doctor sooner if you:
“Achalasia is a rare chronic disease,” says Dr. Raja. “Having regular follow-ups with an experienced specialist is important for long-term relief from symptoms and to ensure your esophagus is working as well as it can.”
Learn more about our editorial process.

Often, a throat tickle is due to a cold, allergies or GERD — but see a doctor if it won’t go away

For some lucky people, these pillows can eliminate the need for medications or surgery

There’s not enough research to know, but it’s OK to try it for most

Lifestyle changes such as diet and weight loss or medication such as antacids can bring relief

Here’s five ways to cut your hiccups short

Mix up your regular cup, with these low-acid options

The short answer from a gastroenterologist

Your metabolism may torch 1,300 to 2,000 calories daily with no activity

A gentle touch in all the right places may help drain your sinuses