Early detection of the disease can extend your life, but there are specific testing guidelines
Early detection of lung cancer increases your odds of successful treatment and celebrating more birthdays. But a lung cancer screening comes with a few risks, too. So, should you get checked?
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The American Cancer Society, American Lung Association and the U.S. Preventive Services Task Force (USPSTF) say “yes” if you meet certain criteria tied to long-time cigarette use.
Let’s take a closer look at your options with pulmonologist Peter Mazzone, MD, MPH.
A lung cancer screening isn’t for everyone, states Dr. Mazzone. It’s recommended only for adults who are at high risk for the disease — which explains why screening guidelines are pretty specific.
The USPSTF suggests an annual lung cancer screening if all of the following apply:
It’s also important that you’re healthy enough to benefit from finding and treating early-stage lung cancer. People who get tested don’t typically have symptoms of lung cancer.
“If someone comes to us in a wheelchair already wearing oxygen and couldn’t tolerate treatment, they typically aren’t eligible for screening,” clarifies Dr. Mazzone. “However, there are nearly 15 million Americans who are at high risk and should receive screening.”
It should be noted, too, that a lung cancer screening is a quick and painless imaging exam. It uses low-dose computed tomography, or low-dose CT, to capture very detailed pictures of your lungs.
As noted, lung cancer often doesn’t announce itself with early symptoms. So, without an annual screening, lung cancer is often detected once the disease has progressed and spread — which makes successful treatment less likely.
People with lung cancer have about an 80% chance of being alive five years later if the cancer is diagnosed and treatment begins during Stage 1. The five-year survival rate is about 4% if tumors have spread.
That leads us to this alarming reality: Only about 1 in 4 people with lung cancer are diagnosed before the cancer spreads. “Early detection is key to changing that,” says Dr. Mazzone.
Are lung cancer screenings perfect? Of course not. Scans sometimes detect small spots called nodules that look concerning but are basically harmless little scars. Radiation exposure is a concern, too. Ditto for overdiagnosis of conditions and additional testing and stress.
“But the benefits of lung cancer screening still outweigh any potential harm for many people,” notes Dr. Mazzone.
Lung cancer is found in about 1 in every 140 people who get screened. This may sound like a small number, but it’s about the same or better than the results for breast cancer and colon cancer screening.
A counseling session is often required before a lung cancer screening so you can discuss lung cancer risks, the screening process, benefits and potential harm. It can be a complex and difficult decision for people to make.
“Many people value the potential benefit of screening so much they’re happy to accept them,” explains Dr. Mazzone. “Others may have a different perspective. Talk to your doctor to help decide what’s best for you.”
And because the test is annual, the decision on whether to do it can be revisited every year.
Learn more about our editorial process.

Vaping exposes you to thousands of chemicals, including many that cause cancer and lung disease

Your risk goes down once you quit, but you may still need a lung cancer screening
Knowing the signs (like a cough that won’t quit) may help some people detect lung cancer early

Lung cancer is not just a smoker’s disease
Early detection and screening are important
Early detection through screening can improve survival numbers
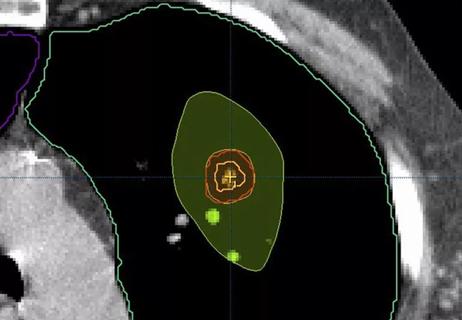
SBRT is an effective option when you’re too frail for surgery

Both conditions have similar symptoms, but different causes and treatments

Your metabolism may torch 1,300 to 2,000 calories daily with no activity

A gentle touch in all the right places may help drain your sinuses