Researchers identify a new subtype of multiple sclerosis
Every case of multiple sclerosis is a little different. Every patient has his or her own set of symptoms and course of treatment. This is something doctors know well.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
But they’re learning more about how that individualization looks inside the body, and about what’s needed to be able to offer patients better treatments that are more personalized for them.
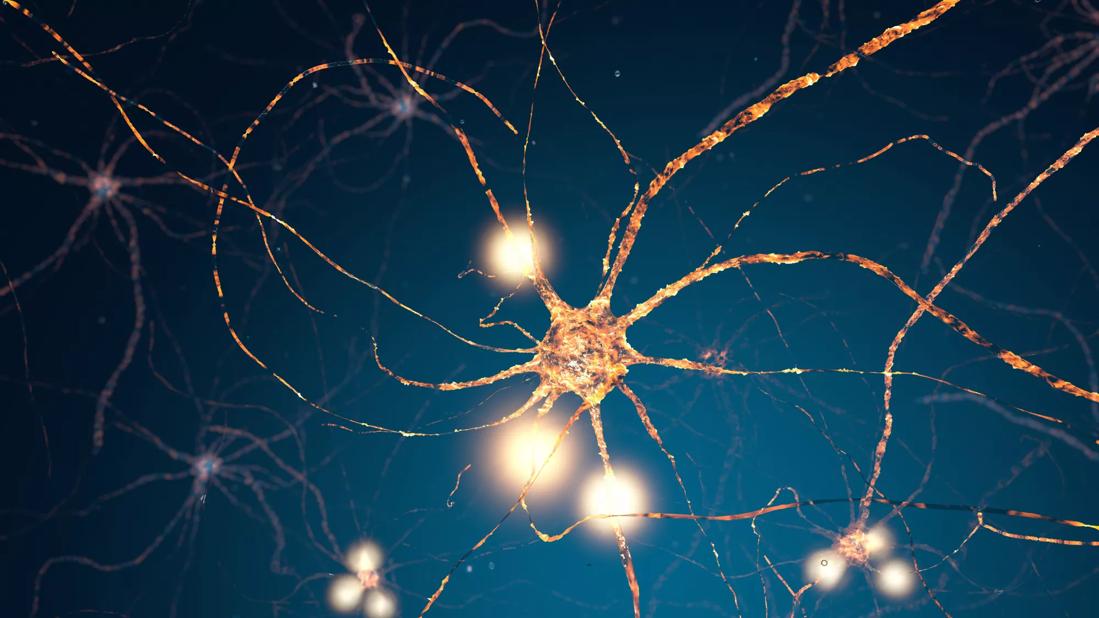
Multiple sclerosis is an autoimmune condition that can cause an assortment of muscle, vision and cognitive problems. In the medical community, it’s characterized by an attack of the immune system on the myelin that coats nerve cells in the brain and spinal cord.
Think of myelin as the protective coating on a piece of wire. “It insulates the nerve cell’s axon, which is the wire of the brain,” explains Bruce Trapp, PhD, Chairman of the Department of Neurosciences in Cleveland Clinic Lerner Research Institute, who’s been researching multiple sclerosis for more than two decades.
Myelin also plays a critical role in relaying messages between the brain, spinal cord and the rest of the body. When myelin is damaged, nerve cells are left exposed, and they aren’t able to do their jobs as effectively. Eventually, they die off. That’s what’s known as neural degeneration.
A research team led by Dr. Trapp recently discovered that not all people with multiple sclerosis experience the destruction of myelin in the brain and spinal cord in the same way.
Surprisingly, they found that some patients don’t even show any visible signs of damaged myelin in the white matter of the cerebrum, the part of the brain that is responsible for directing motor function, sensory processing, communication and memory. This has classically been thought of as a hallmark of the disease.
The fact that nerve cell degeneration can happen without this loss of myelin in the brain’s white matter opens up a whole new area in MS research, say Dr. Trapp and Daniel Ontaneda, MD, a neurologist in Cleveland Clinic’s Mellen Center for MS. They say it’s so significant that they’ve given this type of multiple sclerosis a name – myelocortical MS.
“This may have implications in the types of treatments that we use,” Dr. Ontaneda says. “One might hypothesize that the treatments we have available currently might not work the same in both groups.”
Or, some patients might benefit from a combination of neuroprotective therapies and anti-inflammatory therapies to stop progression of the disease.
The big challenge, for now, is that doctors can’t see these differences in myelin loss just by looking at an MRI. So, Drs. Trapp and Ontaneda also see a need for more specific MRI technology that would allow doctors to detect and monitor the loss of myelin in these patients. “MRI is a very young technology, so we have yet to see the best,” Dr. Trapp explains.
Both doctors are hopeful that their research will lay a path for new, tailored treatment strategies for patients living with different forms of MS.
Learn more about our editorial process.
The benefits go beyond cosmetic enhancements

Watch out for vision loss, facial paralysis, limb weakness and dizziness

Advice for keeping multiple sclerosis in check
The short answer from a neurologist

FDA approves drug to help treat symptoms of SPMS

Eating mindfully, sipping water and chewing slowly can help your brain catch up with your stomach

Seizure symptoms can go far beyond convulsions and may include feelings of déjà vu, temporary confusion and unusual movements

They can feel like a typical headache or a migraine headache, but the pain can last for weeks to months

Your metabolism may torch 1,300 to 2,000 calories daily with no activity

A gentle touch in all the right places may help drain your sinuses