It can take time for doctors to find a diagnosis

You’ve done your research and are convinced that an autoimmune disease is to blame for your dry eyes, fatigue and thinning hair. But your doctor isn’t so sure. Why is it so hard to correctly diagnose autoimmune diseases like rheumatoid arthritis (RA), lupus or Sjögren’s?
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
There are plenty of autoimmune diseases — not to mention other conditions — that share similar symptoms. And the vagueness of these symptoms (i.e., “My muscles ache. I feel tired all the time.”) makes it challenging for doctors to offer a definitive diagnosis. But as rheumatologist Linda Mileti, MD explains, you may not even need a specific diagnosis to get the healing underway.
“Patients, understandably, want answers for why they are feeling unwell,” says Dr. Mileti. “But it’s important to rule out conditions rather than jump to conclusions. I’ve had people come in who are convinced they have lupus, when in fact they had sleep apnea. We have completely different ways of addressing these two conditions.”
Dr. Mileti says it can feel like a slow process to correctly identify what’s causing your discomfort or malaise. Even if your doctor suspects an autoimmune disease, it can take time to determine what specific disorder you’re dealing with. If you have mild symptoms, you may need to wait for the disease to blossom and the signs to become more obvious.
“We may use laboratory tests to check for antibodies specific to lupus, RA or Sjogren’s,” says Dr. Mileti. “When they are positive, we breathe a sigh of relief because we have something concrete. But often, the labs aren’t definitive or the antibody the person has doesn’t match their symptoms.”
“It’s frustrating for patients to play the waiting game,” says Dr. Mileti. “I tell people that even with a clear-cut diagnosis of lupus, RA or Sjögren’s, we don’t have a one-size-fits-all treatment plan.”
Doctors get personal when treating autoimmune diseases. Often, they treat the symptoms the person is experiencing, not the disease itself. This individual attention is significant because one person with lupus may have kidney disease requiring potent immunosuppressant drugs. Another person may have a rash and joint pain, which doctors may treat with mild medication.
Dr. Mileti says patients with autoimmune disorders often experience fatigue. Since there isn’t an effective fatigue treatment, she recommends that patients:
Patients also need monitoring. “A patient taking medicine will need frequent lab tests, so I can make sure the medicines aren’t affecting other organs,” says Dr. Mileti. “Patients who aren’t receiving active treatment typically come back once a year. I check for evidence of inflammation and that the disorder isn’t damaging organs.”
Dr. Mileti sees many people for second, or third, opinions. Often, she finds people have been made to feel that they’re not really suffering because they haven’t been diagnosed with a condition. But, says Dr. Mileti, a person can be unwell even if they don’t have a diagnosis.
“I always reassure and validate that the symptoms are real,” says Dr. Mileti. “But I let people know we could do more harm if we jump to a diagnostic conclusion and use unnecessary medicine.”
Dr. Mileti says it’s appropriate to monitor and treat symptoms that pop up. As time goes on, the condition may blossom and become apparent, making treatment easier. “And sometimes the opposite happens — with a little time, the symptoms resolve on their own.”
Learn more about our editorial process.

The answer varies from person to person and vaccine to vaccine

The autoimmune protocol diet is designed to help identify inflammatory triggers

A compromised immune system requires precaution

Managing the chronic pain of this autoimmune condition is important

The link between joint pain and skin rashes
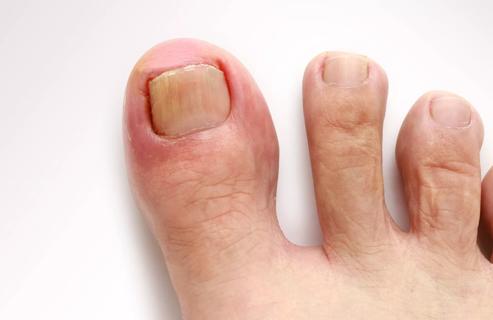
Pain meds, toenail protectors and petrolatum jelly may spare you a trip to a podiatrist

An ice bath can ease sore muscles and decrease inflammation after a workout

Wrist flexor and extensor stretches are the best stretches for wrist pain

Your metabolism may torch 1,300 to 2,000 calories daily with no activity

A gentle touch in all the right places may help drain your sinuses