Skin conditions in babies and kids may include rashes, hives, warts, acne, birthmarks and more. These conditions may be caused by dermatitis, viral infections, bacterial infections, fungal infections or other diseases. Treatment varies from anti-itch creams to pain relievers to antibiotics, depending on the condition.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Various skin conditions can affect babies, toddlers, children and adolescents throughout their lives. Healthcare providers receive more than 12 million office visits from children each year related to skin concerns. Skin conditions in kids may include hives, warts, acne, birthmarks and all sorts of rashes.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Many different types of rashes can affect your child. Dermatitis, viral infections, bacterial infections, fungal infections and many other conditions may cause rashes.
Dermatitis is an umbrella term for any condition that causes skin inflammation. These conditions may cause red rashes, itchiness and dry skin on your child and happen at any age. Types of dermatitis include diaper rash, cradle cap, eczema and contact dermatitis.
Diaper rash: Diaper rash is also called diaper dermatitis. It’s the most common skin condition seen in babies. Diaper rash occurs when moisture in your baby’s diaper area causes irritation or growth of fungi or bacteria that normally live in small amounts on the skin. To prevent or treat diaper rash, keep your baby’s diaper area clean and dry by changing diapers frequently. When changing your child's diaper, leave it off for a short while before putting it back on. You can also apply an ointment or cream that contains zinc oxide or petroleum jelly to protect your baby’s skin in the diaper.
Cradle cap: Cradle cap is also called infant seborrheic dermatitis. It’s a skin condition that looks like yellow scaly patches often surrounded by a red rash on your baby’s scalp. Overproduction of the oil-producing sebaceous glands on your baby’s scalp may cause cradle cap. You can treat cradle cap at home with mild baby shampoo and can also lightly rub the scale off if it doesn’t bother your baby.
Advertisement
Eczema: Eczema is also called atopic dermatitis. Eczema makes your child’s skin itchy and then it gets red, irritated and dry. Differences in your child’s skin barrier (compared to normal, healthy skin) and an immune system that tends toward allergies cause eczema. Issues with the barrier make your child’s skin more sensitive and prone to infections and dryness. Controlling your child’s symptoms is the goal of treatment. Often there are seasonal or allergic triggers that you should help your child avoid. Good skin care includes bathing in warm but not overly hot water and moisturizing regularly, especially immediately after baths or water exposure.
Contact dermatitis: Contact dermatitis can occur when kids have a reaction to an allergen or an irritant. Allergens may include poison ivy or medications. Irritants may include perfumes, soaps, cleaners and paints. Contact dermatitis causes an itchy skin rash that is sometimes also painful. Treatment includes moisturizers, anti-itch creams and topical (or sometimes oral) steroids.
Viral rashes in babies, toddlers and kids are caused by a variety of different viruses. These infections include fifth disease, roseola, chickenpox, measles, rubella, molluscum contagiosum and hand, foot and mouth disease.
Fifth disease: Fifth disease is also called slapped cheek (slap face) disease. It causes a bright red rash on your child’s cheeks. A specific virus, Parvovirus B19, causes fifth disease. Along with the rash, your child may have a fever and other nonspecific symptoms. After a few days, the facial rash will fade. But then pink patches may develop in a lacy pattern on your child’s arms and legs. Treatment includes comfort measures like non-steroidal anti-inflammatory drugs (NSAIDs) anti-itch creams or antihistamines.
Roseola: Roseola is also called sixth disease. Human herpesvirus 6 causes roseola. With roseola, your baby will suddenly develop a high fever that can last up to a week. Once the fever breaks, a slightly raised, spotty pink rash may appear on your baby’s chest or stomach. The rash may spread to your baby’s upper arms and neck, and then it will fade after about 24 hours. Treatment may include acetaminophen for your baby’s fever, but the rash doesn’t itch or cause pain.
Chickenpox: Varicella zoster virus causes chickenpox. It can be prevented by a vaccine. Chickenpox generally causes a rash on your child’s face, chest and back first, but it may travel to their entire body. The rash turns into itchy, fluid-filled blisters, then blisters turn into scabs. Chickenpox usually goes away on its own in one to two weeks. You can treat your child’s symptoms with antihistamines and acetaminophen. They are contagious until all of the blisters are crusted over.
Advertisement
Measles: Morbillivirus causes measles. Measles is very contagious and prevented by the measles vaccine or MMR vaccine. It causes a rash that starts on your child’s face. It’s typically seen behind the ears or around your child’s mouth. Then it moves down over their body. The rash starts as flat red spots, but then smaller raised white spots may appear on top of the red spots. The spots may join together as it moves down your child’s body. Measles has to run its course. It will go away within about two weeks unless complications develop. You can treat your child’s symptoms of fever and achiness with acetaminophen or NSAIDs.
Rubella: Rubella is also called German measles and can be prevented by a vaccine. It can look similar but is caused by a different virus than measles. Rubella causes a red or pink rash that starts on your baby’s face and neck. The rash then spreads to other parts of your baby’s body and lasts about three days unless complications develop. Your baby may have a fever, cough or runny nose before the rash appears. Rubella has to run its course. You can treat your child’s symptoms of fever and achiness with acetaminophen or NSAIDs.
Molluscum contagiosum: Molluscum contagiosum virus causes this benign but sometimes unpleasant rash. Molluscum contagiosum has raised bumps on your child’s skin. The bumps are usually flesh-colored, pink or pearly white with indentations in the center. The bumps will show up on your child’s face, chest, stomach, arms and legs. They’re painless but they may not go away for several months or years. Molluscum contagiosum will eventually go away on its own without treatment.
Advertisement
Hand, foot and mouth disease: A virus in the enterovirus family causes hand, foot and mouth disease. The disease causes a red rash to develop around your toddler’s mouth, and on the palms of their hands and soles of their feet. It may also affect other areas. The rash may turn into bumps or blisters on your baby’s skin and in their mouth, and they can be very painful. Hand, foot and mouth disease usually goes away on its own within one to two weeks. You can treat your toddler’s symptoms with acetaminophen or NSAIDs.
Types of baby rashes may also include bacterial infections such as scarlet fever and impetigo.
Scarlet fever: A bacteria called group A Streptococcus causes strep throat and scarlet fever. Scarlet fever usually starts with a fever, sore throat and headache, but the key symptom is a raised, red rash on your child’s neck and upper chest. The rash may then spread to other areas of your child’s body. Your child’s face may be red with a pale area left around their mouth. The rash feels rough like sandpaper and may look like your child has a sunburn. Treatment for scarlet fever includes antibiotics.
Impetigo: Group A Streptococcus or Staphylococcus aureus bacteria cause impetigo. It’s most common in kids aged 2 to 5 years old but can happen at any age. Impetigo causes red bumps, blisters or crusty spots to develop. These are most common around your toddler’s mouth and nose and can be anywhere that skin gets repeatedly irritated. Treatment for impetigo usually includes antibiotics that may be oral or put directly onto the skin.
Advertisement
Common skin rashes seen in babies, toddlers and children can also include fungal infections such as ringworm.
Ringworm: Despite its name, a fungus causes ringworm, not a worm. It causes round or oval patches to develop on your child’s skin. The patches have smooth centers and red, scaly borders and may not look like rings right away. But you’ll notice the rings when they get bigger. The patches may be itchy and painful and may become puffy and inflamed. You can treat your child’s ringworm with antifungal medicines either orally or put directly on the skin.
When your baby’s teeth are starting to come in, they may drool a lot more than usual. Drool can irritate your baby’s skin. This can cause a harmless rash known as a teething rash. The rash causes tiny, red raised bumps on your baby’s face, neck or chest. Teething rashes may come and go as new teeth pop up or when your baby stops drooling as much.
Teething rashes don’t cause fevers, so if your baby has a fever with a rash, talk with their healthcare provider. You can treat your baby’s teething rash by keeping the area clean and dry. You can also apply emollient cream to the affected area. This may prevent your baby’s drool from irritating their skin.
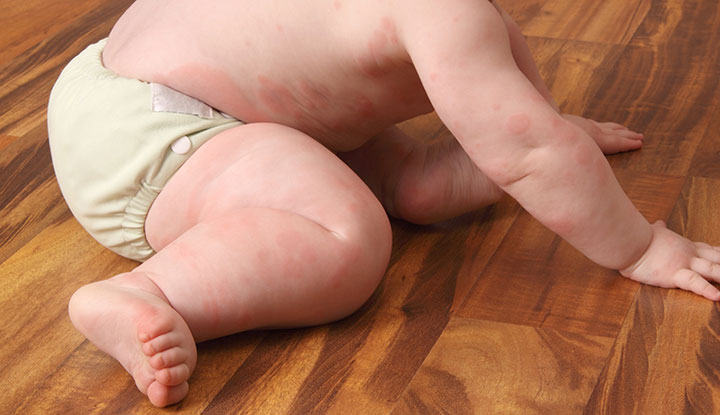
Hives are also called urticaria. Hives are itchy pink, pale or red bumps on your baby’s skin. They may be small slightly raised spots or large welts of different shapes. Sometimes hives are ring-shaped or look like targets. The rings may have normal-looking skin in the center, or they may look pale, purple or blue. Hives can appear anywhere on your child’s body and may flatten out over several hours. But new bumps can keep showing up for days or weeks.
Viral infections are a common cause of hives. But allergic reactions to foods, medicines and additives, or even cold temperature and stress may also cause hives. But many cases of hives have no known reason. The best treatment for hives is antihistamines.
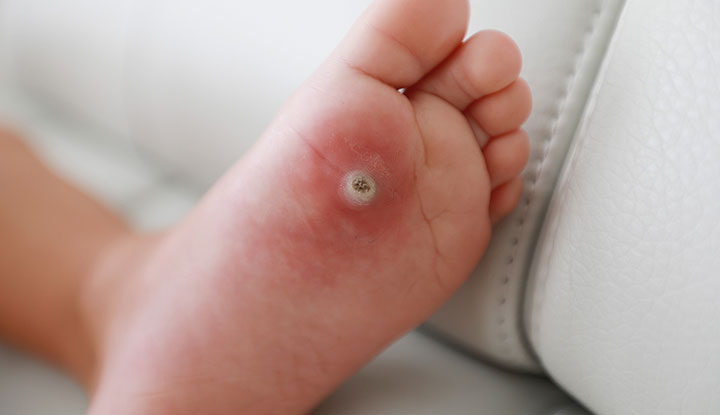
Warts on kids are a type of skin infection caused by the human papillomavirus (HPV). There are multiple types of HPV that cause infections in different areas of skin. The infection causes hard bumps to form on your child’s skin. Warts most commonly appear on your child’s hands and fingers, but they can also appear on their feet, face, genitals and knees. Warts are common in children of all ages. Warts often go away on their own after your child’s immune system fights off the virus, but they can be painful and unpleasant in appearance.
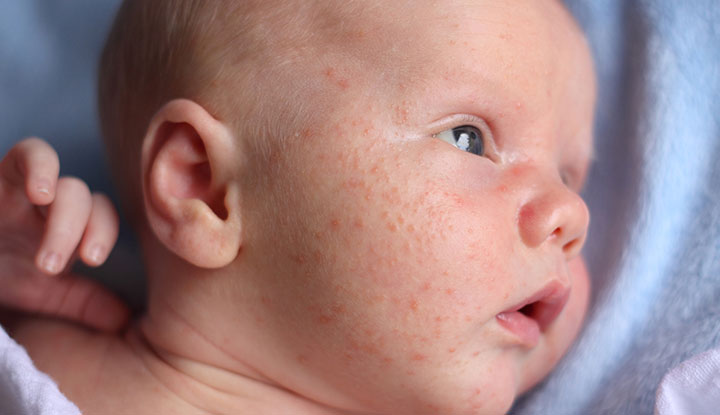
Baby acne causes little white bumps and pink pimples to appear on your baby’s face including their forehead, cheeks, eyelids and chin. An inflammatory reaction to yeast on your baby’s skin may cause baby acne. Sometimes baby acne is seen on your baby’s chest or neck. Baby acne usually goes away on its own within your baby’s first three months of life.

There are two main types of birthmarks — red birthmarks and pigmented birthmarks. Red birthmarks are skin markings caused by a collection of blood vessels. Pigmented birthmarks are areas in which the color of your child’s birthmark is different from their skin color.
Strawberry hemangiomas: Strawberry hemangiomas can be found anywhere, but are most commonly found on your baby’s face, scalp, back or chest. They’re made up of small, closely packed blood vessels. Strawberry hemangiomas usually fade or go away as your child ages. Some minor discoloration or wrinkling of your child’s skin may remain at the site of the hemangioma.
Cavernous hemangiomas: Cavernous hemangiomas look sort of like strawberry hemangiomas. But they’re deeper in your child’s skin and often darker in color. They look like reddish-blue spongy masses of tissue filled with blood. Cavernous hemangiomas usually go away on their own as your child ages.
Port-wine stains: Port-wine stains are flat, reddish-purple birthmarks. They’re made up of dilated blood capillaries. They’re commonly seen on your child’s face and they vary in size. Port-wine stains are permanent, without treatment. They might thicken or darken over time.
Salmon patches: Salmon patches are also called stork bites or angel’s kisses. Salmon patches are small blood vessels that are visible through your baby’s skin. They are frequently seen on your baby’s forehead, eyelids, upper lips, between their eyebrows and on the back of their neck. Salmon patches fade as your baby grows.
Slate gray nevus or congenital dermal melanocytosis (previously called Mongolian spots): These birthmarks are typically bluish and may look like bruises. They’re often found on your baby’s buttocks and/or lower back. Sometimes they appear on your baby’s chest, back or arms. Mongolian spots are seen most often in babies with darker skin.
Pigmented nevi: Pigmented nevi are also called moles. Moles are growths on your baby’s skin that typically are flesh-colored, brown or black. Moles can appear anywhere on your baby’s skin. Your baby may have one mole or several in a group.
Congenital nevi: Congenital nevi are moles that your baby was born with. These moles have a slightly increased risk of becoming skin cancer. Larger congenital nevi have a greater risk than smaller congenital nevi do. Your baby’s healthcare provider should examine all congenital nevi and may refer you to dermatology.
Cafe-au-lait spots: Cafe-au-lait spots are light tan or brownish-colored spots. They’re usually oval-shaped. They commonly appear at birth but might develop in the first few years of your child’s life. Cafe-au-lait spots are usually harmless. But if your child has many cafe-au-lait spots, or if they are large, consult their healthcare provider. It may indicate a serious genetic condition.
Finding a rash, bump, mark or other skin condition on your child’s body may be scary. But kids get tons of rashes, and most of the time, these rashes and other conditions shouldn’t cause too much worry. If you have any concerns, check in with your child’s healthcare provider. They can usually easily diagnose the skin condition and get your child started on any treatment, if necessary.
As your child grows, you need healthcare providers by your side to guide you through each step. Cleveland Clinic Children’s is there with care you can trust.

Last reviewed on 04/21/2022.
Learn more about the Health Library and our editorial process.