Vasculitis is an autoimmune disease that causes inflammation in your blood vessels. The swelling makes it hard for blood to flow through your affected vessels, which can cause organ and tissue damage. Most people can manage their symptoms with medication.
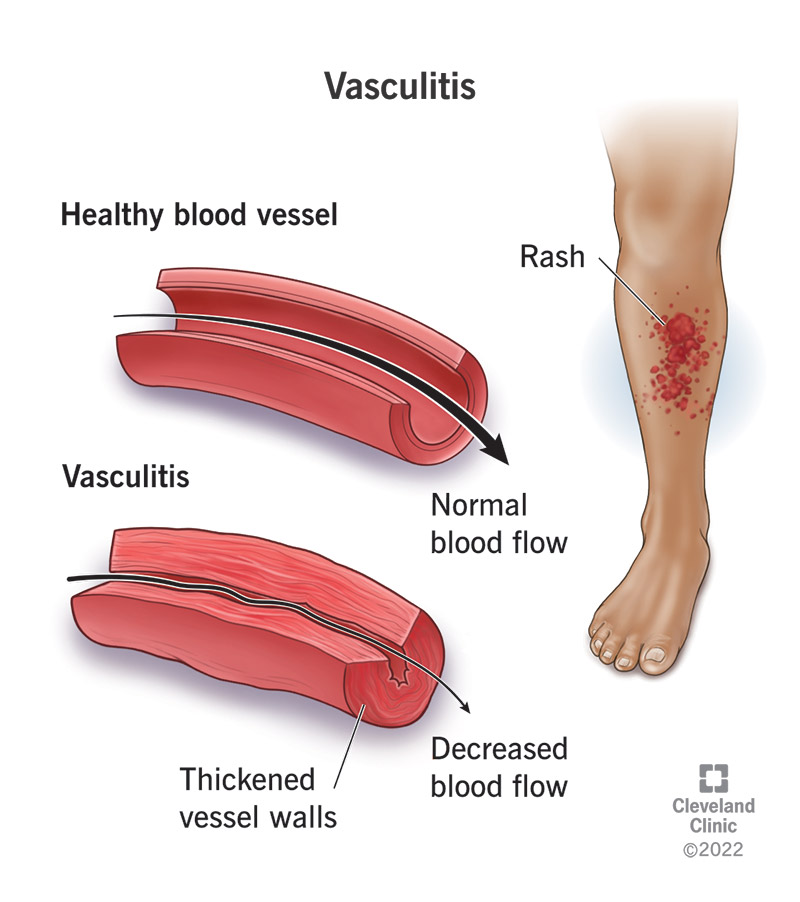
Vasculitis is a condition that causes inflammation (swelling) in your blood vessels.
Blood vessels are channels that carry blood throughout your body. They form a circuit that begins and ends at your heart. You have three types of blood vessels:
If you have vasculitis, your blood vessels swell and thicken. This makes it harder for blood to flow through them. Over time, the inflammation can damage your organs and cause serious complications like aneurysms.
Most people with vasculitis can manage their symptoms with medication. But vasculitis can be fatal if you experience severe symptoms that affect blood flow to your organs.
Visit a healthcare provider if you experience symptoms like fever or feel numbness or tingling in your hands or feet. Call 911 (or your local emergency number) or go to the emergency room if you’re having trouble breathing or experiencing heart attack symptoms.
Vasculitis can affect any blood vessel in your body, including the ones that are connected to your:
Vasculitis is rare. Experts estimate fewer than 50 out of every million people in the U.S. develop it each year.
People older than 50 are more likely to develop vasculitis, but it’s still rare. Experts estimate that fewer than 300 people in one million people older than 50 in the U.S. are diagnosed with vasculitis each year.
There are more than 30 types of vasculitis. A healthcare provider might diagnose you with a specific kind of vasculitis based on which of your blood vessels are affected.
Some types of vasculitis include:
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Some of the most common vasculitis symptoms include:
Which symptoms you experience depends on which blood vessels are affected and how severe the inflammation is.
Listen to your body and trust your instincts. Visit a healthcare provider if you notice any changes or symptoms that make you feel worried or uncomfortable.
Vasculitis is an autoimmune disease. Autoimmune diseases are the result of your immune system accidentally attacking your body instead of protecting it. Experts aren’t sure what makes your immune system attack your blood vessels and cause vasculitis.
Some heath conditions that cause inflammation in your body can trigger vasculitis. Some people develop vasculitis with no cause or trigger (developing it idiopathically).
Some triggers of vasculitis include:
A healthcare provider will diagnose vasculitis with a physical exam and tests. They’ll ask you about your symptoms and when you first noticed them.
Diagnosing vasculitis is usually part of a differential diagnosis for other conditions. This means your provider will probably use a few tests to determine what’s causing your symptoms before diagnosing you with vasculitis. Some tests you might need include:
You’ll probably need to see a rheumatologist — a healthcare provider who specializes in treating inflammatory diseases.
Your provider will suggest treatments that manage the symptoms you’re experiencing. They’ll help you find treatments that prevent damage to your blood vessels and organs. Some medications your provider might prescribe include:
You might need surgery if vasculitis damages your blood vessels. Your provider or surgeon will tell you which type of surgery you’ll need and what to expect.
There’s no cure for vasculitis. Once you find treatments that manage your symptoms well, you might enter remission — long periods of time between episodes of symptoms. Some people are in remission for months or years before experiencing symptoms again.
You can’t prevent vasculitis because experts don’t know what causes it. There’s no way to know if someone will develop it.
You should expect to manage vasculitis for a long time, maybe for the rest of your life. Even if you don’t have severe symptoms, you’ll need to see a provider regularly to monitor any changes in your blood vessels. Ask your provider how often you need follow-up appointments and tests.
Even if you enter remission, there’s always a chance vasculitis will cause symptoms again in the future.
Monitor your symptoms and keep track of any changes you notice. Follow the treatment plan you worked on with your provider. Don’t hesitate to visit them if you think a treatment isn’t working (or isn’t as effective as it used to be).
See your provider if you notice new symptoms, or if your symptoms are getting more severe.
Your provider will tell you how often you’ll need regular follow-up appointments, blood tests or additional screenings.
Go to the emergency room or call 911 (or your local emergency number) if you’re experiencing any of the following symptoms:
A note from Cleveland Clinic
Vasculitis is inflammation in your blood vessels. Even if you only ever experience mild symptoms, you’ll need follow-up visits and appointments with a healthcare provider. They’ll monitor any changes in your blood vessels and make sure vasculitis hasn’t damaged your organs.
Vasculitis can be confusing because it affects everyone differently. Trust your instincts — don’t ignore or downplay new or changing symptoms. Talk to your provider if you have any questions. They’ll help you understand what’s going on inside your body and which treatments you’ll need.
Last reviewed by a Cleveland Clinic medical professional on 08/17/2023.
Learn more about our editorial process.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy