Cortisone shots (steroid injections) deliver a dose of medication directly to a problem spot in your body. Corticosteroids can help reduce inflammation. Injections can be helpful in treating conditions like arthritis, tendinitis or bursitis.
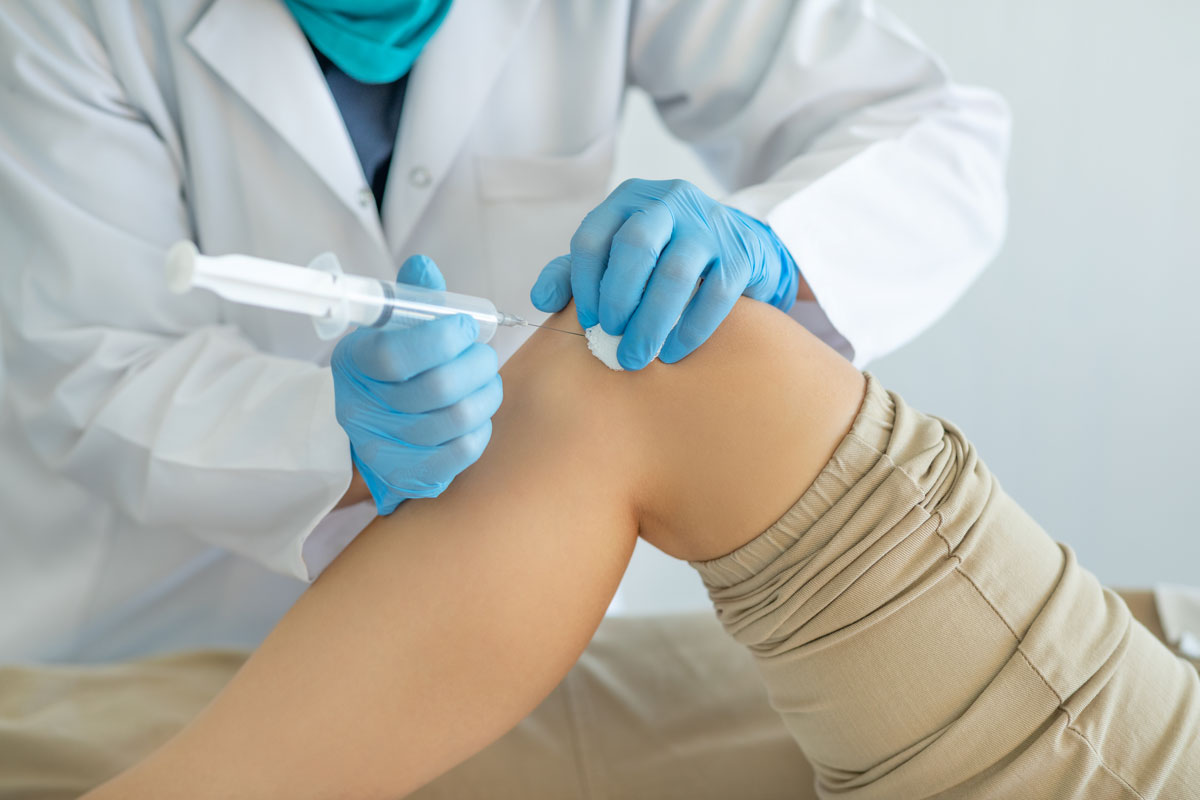
A cortisone shot is an injection of medicine that relieves pain and reduces inflammation (swelling). Healthcare providers also call them steroid injections or steroid shots. These are the same treatment — a dose of a corticosteroid injected into your body.
Corticosteroids (steroids) are manufactured drugs that closely resemble cortisol, a hormone your adrenal glands produce. They temporarily reduce your immune system’s activity to decrease inflammation.
Providers usually use cortisone shots to treat inflammation in your joints, including your:
Your provider might also use cortisone shots to treat inflammation in your tendons or bursae — the fluid-filled sacs that cushion spaces around and between your joints, tendons and bones.
A healthcare provider might treat any condition that causes pain and inflammation with a cortisone shot, including:
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A healthcare provider may give you a cortisone shot during a normal office visit. Or they might schedule a separate visit for the injection.
Your provider will insert a needle into the area that needs treated and inject cortisone (a steroid). They might use an ultrasound to guide the injection needle.
A cortisone shot might sting when your provider puts the needle into your skin, but it shouldn’t cause intense pain. Your provider might give you a local anesthetic to numb the area around the injection site.
Tell your provider if you experience fear or anxiety about getting shots. They’ll help you relax and feel more comfortable about receiving a steroid injection.
A cortisone shot reduces pain and inflammation in the area around where your provider injects it.
Inflammation usually happens when your immune system sends cells to fight infections or heal an injury in your body. Your provider will inject cortisone into the part of your body that’s experiencing inflammation. The cortisone calms your immune system’s response in that location. This reduces pain and inflammation.
Your provider will inject cortisone directly into the area of your body that’s experiencing inflammation. This will deliver the dose of corticosteroid right where it’s needed.
The steroid medication will circulate through your bloodstream and can affect other areas of your body. But these systemic effects are usually so small that you won’t notice them.
Cortisone shots are a safe, effective way to relieve pain and inflammation. They can help you manage symptoms or conditions that make it hard (or impossible) to participate in all of your day-to-day activities.
The most common side effects of cortisone (steroid) shots include:
It’s rare for steroid injections to cause severe side effects, but it’s possible to experience:
People who receive many rounds of steroid injections may have an increased osteoporosis risk.
You shouldn’t receive steroid injections if you have an infection. Corticosteroids have a short-term immunosuppressant effect and can make it harder for your body to fight an infection and heal itself.
People who take blood-thinning medications (anticoagulants) or have a bleeding disorder (like hemophilia) may not be able to receive steroid injections. Tell your provider which conditions you have and how you’re managing them, including which medications or supplements you take.
How long it takes for a cortisone shot to work varies from person to person. Your symptoms, like pain and inflammation, might not get better immediately. It can take up to a week for a cortisone shot to take effect. Talk to your provider if it’s been more than 10 days and you don’t feel better.
You might only need one cortisone shot to relieve pain and inflammation, especially if you’re recovering from a temporary injury. If you have a chronic (long-term) condition, you might need more steroid injections in the future.
Your provider will tell you when it’s safe to receive another dose. You’ll probably need to wait at least three months between rounds of steroids. Most people shouldn’t have more than three shots in a year.
Everyone’s body responds differently to a cortisone shot. Steroid injections usually last somewhere between a few weeks and a few months. If you’re experiencing inflammation after an injury, the cortisone shot should be effective long enough for your body to heal fully.
If you experience chronic inflammation, you might notice your symptoms returning gradually over time. Talk to your healthcare provider if you notice new or worsening inflammation.
Talk to your provider if you’re still experiencing pain and inflammation more than 10 days after a cortisone shot. Let them know if your symptoms start to return a few months after your first cortisone shot.
Visit your healthcare provider if you experience any of the following symptoms after a cortisone shot:
Cortisone is a type of corticosteroid. Providers might refer to cortisone shots or steroid injections with the shortened term “steroids.” This means any manufactured medication that reduces swelling in your body.
These anti-inflammatory steroids are different from the anabolic steroids some athletes use to gain an unfair competitive advantage. Anabolic steroids are manufactured forms of testosterone.
Cortisone shots or other types of corticosteroids a healthcare provider prescribes are safe. They’ll tell you which type of medication you’ll need and will give you the injection themselves.
Anabolic steroids aren’t safe to use recreationally or without a prescription from your provider. Nonprescription doses are often 10 to 100 times higher than what providers prescribe to treat medical conditions. Side effects from nonprescription steroid injections are usually more severe and can be life-threatening.
Healthcare providers use cortisone shots to treat inflammation throughout your body. They’ll inject cortisone directly into an area that’s experiencing inflammation. You should feel relief from symptoms around a week after your injection.
Some people only need one cortisone shot to give their body time to heal after an injury. Others need regular injections to help them manage a chronic condition. Your healthcare provider can tell you if or how often you’ll need follow-up injections.
Last reviewed by a Cleveland Clinic medical professional on 02/05/2025.
Learn more about our editorial process.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy