The best treatment depends on the cause
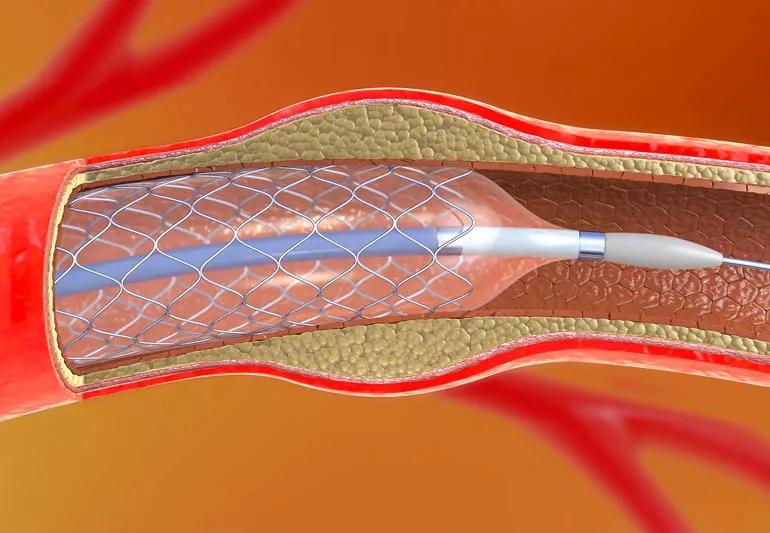
Good blood flow throughout your body is obviously important. That’s why stenosis, or narrow blood vessels, is a problem. And unfortunately, this problem can happen again after you’ve had a blocked artery reopened. That’s when it becomes restenosis.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Stent placement helps restore blood flow through previously blocked arteries, but some patients develop restenosis (re-narrowing) over time.
Stephen Ellis, MD, Director of Interventional Cardiology, explains, “There are effective ways to restore blood flow if restenosis occurs, but it’s important to assess the cause and to tailor treatment accordingly.”
Despite advances, Dr. Ellis says, “in-stent restenosis still occurs in approximately 3 to 10% of patients within six to nine months, and sometimes afterwards. We have learned that restenosis is a very complex process.”
Some known causes include:
• Stents that are too small or misaligned in the blood vessel.
• Older-generation stents.
• Abundant healing within the stent with scarring.
Before any treatment for restenosis, your doctor will perform tests to understand what’s causing any problems. Catheterization allows doctors to look inside the artery and to perform tests including:
Different options are available to treat restenosis the first time it happens:
For some patients, restenosis is a recurring problem. If the blockage has recurred several times or if there are multiple blockages, your doctor may recommend bypass surgery to restore adequate blood flow.
Other options include:
Medicines. Two oral medications may somewhat lessen the risk of restenosis: sirolimus, the drug used on the first generation of drug-eluting stents, and cilostazol, another type of medicine that helps widen blood vessels and reduce clumping of red blood cells. These are typically used in conjunction with balloon or cutting balloon angioplasty.
Though sometimes useful, these drugs aren’t for every patient and they require more study, Dr. Ellis says.
Brachytherapy. This treatment uses radiation to keep scar tissue from building up again in the stent. Doctors perform brachytherapy at the same time as angioplasty.
After completing angioplasty, the doctor threads another catheter with a “ribbon” of radioactive particles (isotopes) to the blockage, leaves it in place for a few minutes, and then removes the catheter.
When you face problems resulting from restenosis, it is important to find a center that has experienced doctors who are able to provide you with a broad range of treatment options.
Learn more about our editorial process.

First things first — slowly sit or lie down

Absolutely! In fact, in many ways, exercise is key to recovery

There’s no way to stop it once a heart attack is happening, but the most important thing you can do is to call for help

You can counter the risk of prediabetes-related heart attack or stroke by eating more fruits, vegetables and whole grains, as well as exercising regularly

An ideal blood pressure is less than 120 mm Hg systolic and less than 80 mm Hg diastolic

Age, sex and genetics are just a few factors that can affect your risk of developing coronary heart disease
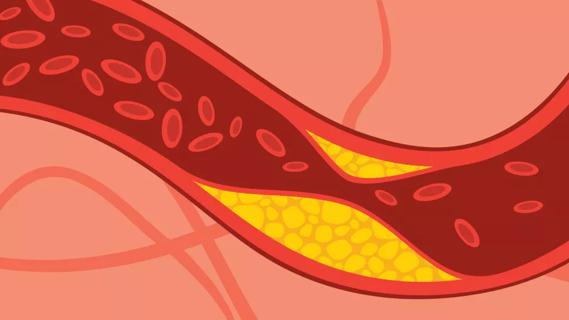
LDL cholesterol and lipoprotein (a) cholesterol are more likely to stick to your arteries and lead to dangerous heart events

Having underweight, having overweight and having obesity can be dangerous for your heart

Your metabolism may torch 1,300 to 2,000 calories daily with no activity

A gentle touch in all the right places may help drain your sinuses