Reduced pulses in feet can signal heart disease risks
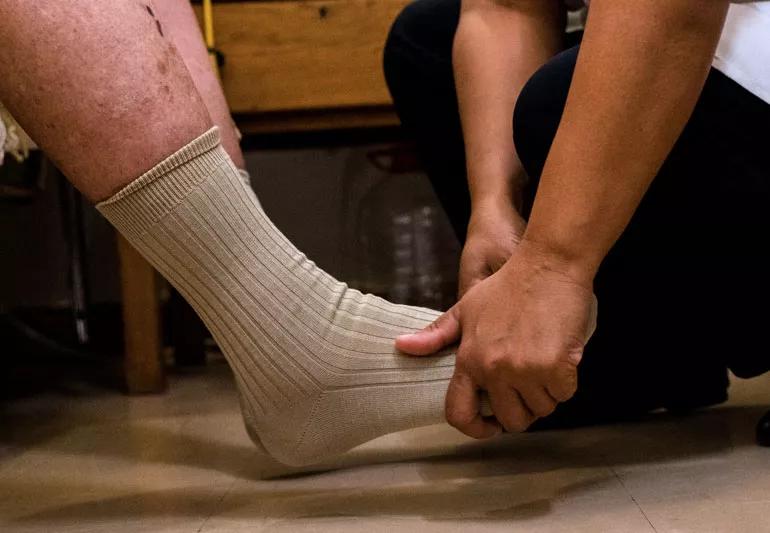
Peripheral artery disease (PAD) is a buildup of cholesterol and plaque in the arteries that lead to your extremities. PAD can cause discomfort in your legs and feet, and limit your walking and activities. Severe PAD can progress to loss of limb. Your doctor can check for signs of the disease with a simple test of pulses in your feet.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
When cholesterol buildup blocks the arteries to your heart, this is called condition coronary artery disease (CAD), explains vascular surgeon Lee Kirksey, MD.
“In reality, PAD and CAD are associated with a single disease, atherosclerosis, which is a buildup of cholesterol in the arteries throughout the body,” Dr. Kirksey says. Sometimes the presence of PAD indicates an increased risk for heart disease, so screening and awareness of the connection between PAD and CAD is important.
The simplest test to screen for PAD is to have your physician check for the pulses in your feet during a routine physical exam. In each foot, there should be two pulses that are easily detected by a trained physician. This test is performed to determine whether the blood flow to your feet is normal.
The next step in screening is the ankle brachial index, which uses blood pressure cuffs on your arm and leg in combination with a Doppler probe, which uses an ultrasound wave, to help hear the pulse in the foot. “Using this technology, we can better assess the blood flow to the area,” Dr. Kirksey says. “For most people, blood pressure in the foot should be similar to the blood pressure in the arm. A drop of as little as 10 percent in that pressure can be an indication of peripheral artery disease.”
You might have encountered offers for “comprehensive” screening/testing at community events, offered by for-profit companies, or surgical or interventional groups. These screenings often cover a wide range of conditions — everything from osteoporosis to coronary artery disease.
You are probably better off being seen by your primary care doctor, who knows you best, to find out whether you ought to have a specific test performed. There’s no proof of benefit to generic testing, and it can have unforeseen consequences, including false positive results that put you at risk for other invasive, unnecessary procedures.
People whose legs are painful or get tired easily or who have trouble walking distances because of leg cramps should have an assessment for PAD, Dr. Kirksey says. Current or past smokers, or anyone with a family history of PAD or symptoms of the disease, should also be assessed.
Screening for PAD probably doesn’t make sense for a healthy individual without symptoms, who is younger than 60 years old, has never smoked and has no family history of atherosclerosis or heart disease, he adds.
In this case, screening may actually expose a patient to more risk. This is because the tests can occasionally be incorrect and lead to much more invasive testing, which has its own inherent risks.
It’s important to remember that atherosclerosis is not a localized process; it is a systemic disease that affects the arteries everywhere in the body. To that end, if you have PAD, you have a greater risk of having a stroke or heart attack, Dr. Kirksey notes.
Medication and lifestyle changes, including stopping smoking, are very important for patients who have any evidence of a decrease in the blood flow in their legs and feet.
So listen to your body and report when your body is talking to you. ‘Charlie horses’ in your legs and muscle cramps may be a sign of vascular disease.
Learn more about our editorial process.

What to expect from a supervised walking program

First things first — slowly sit or lie down

Absolutely! In fact, in many ways, exercise is key to recovery

There’s no way to stop it once a heart attack is happening, but the most important thing you can do is to call for help

You can counter the risk of prediabetes-related heart attack or stroke by eating more fruits, vegetables and whole grains, as well as exercising regularly

An ideal blood pressure is less than 120 mm Hg systolic and less than 80 mm Hg diastolic

Age, sex and genetics are just a few factors that can affect your risk of developing coronary heart disease
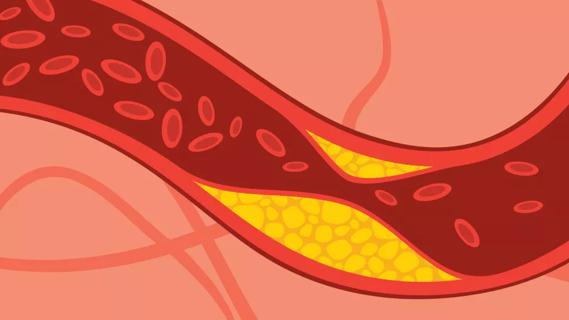
LDL cholesterol and lipoprotein (a) cholesterol are more likely to stick to your arteries and lead to dangerous heart events

Your metabolism may torch 1,300 to 2,000 calories daily with no activity

A gentle touch in all the right places may help drain your sinuses