What to watch out for + what treatment is needed

You see the headlines about the latest football player to suffer a concussion. Or there’s your work colleague whose daughter just got a concussion at her high school soccer game. But nonathletes need to pay attention too, including middle- and older-age adults who can hit their head from a fall. Among people age 65 and older, about 80% of emergency department visits for head injuries happen from a fall.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“A concussion is a temporary decrease in neurologic function in response to a traumatic blow or jolt to the brain or a violent jerk of the head,” explains primary care sports medicine physician Richard Figler, MD. There’s typically no structural damage to the brain, but a cascade of injuries disrupts normal brain function.
A blow to the head can temporarily stun pathways in the brain and the functions they control.
The symptoms of concussion will depend on the part of the brain affected. They include headache, dizziness, blurry vision, nausea and vomiting, light and noise sensitivity, confusion, difficulty focusing or just not feeling right.
People who’ve had a blow to the head need to be monitored for the first 24 to 48 hours to watch for signs of a more serious brain injury, such as bleeding in the brain. “A rule of thumb is to not leave a person with a concussion alone,” Dr. Figler says.
Worrisome signs and symptoms can show up hours or even days after the injury. If there are any concerns, see a doctor right away. “When in doubt, check it out,” he says.

To diagnose a concussion, the doctor will ask questions about the event and subsequent symptoms and perform a neurological exam. An imaging study, such as a computed tomography (CT) scan or magnetic resonance imaging (MRI), isn’t always needed. These are done to rule out other possible causes of symptoms.
“You also need a good cervical spine examination because there can be two different injuries, one to the brain and one to the area of the spine where the skull meets the neck,” Dr. Figler says. People who have degenerative changes in the spine are particularly vulnerable to cervical spine injury. This may cause headaches and neck pain as well as more dizziness and lightheadedness.
“To treat a concussion, first and foremost, support relative brain rest,” Dr. Figler says. This means taking time to rest and recover. Recognize triggers that make symptoms worse, and then slow down or avoid those activities.
For example, “Someone who looks at their smartphone for a few minutes and notices their headache is getting worse or they have eye discomfort should close their eyes,” he says. Those are symptoms from the concussion. “It should go away when you rest.” Don’t aggravate symptoms, and most will gradually improve over one to two weeks.
Sleep is also imperative for recovery. “People typically need more sleep than normal as the brain heals,” Dr. Figler notes.
If a pain medication is needed, avoid anti-inflammatory drugs (which can thin blood) in case a subtle bleed occurred during the fall. Acetaminophen (Tylenol ®) is typically safer.
There’s an increased risk for another concussion shortly after a concussion. So guard against another blow to the head. Dr. Figler also warns against trying to rush recovery. Don’t start driving until your reaction time is back to normal.
This article originally appeared in Cleveland Clinic Arthritis Advisor.
Learn more about our editorial process.
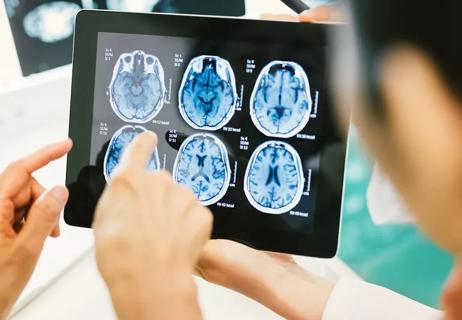
Know the warning signs, what to do and what not to do

The short answer from a concussion specialist

For starters, they’re not just football injuries
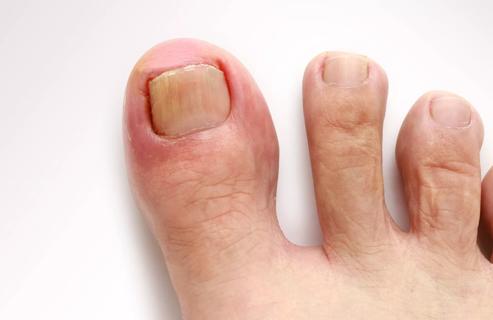
Pain meds, toenail protectors and petrolatum jelly may spare you a trip to a podiatrist

An ice bath can ease sore muscles and decrease inflammation after a workout

Wrist flexor and extensor stretches are the best stretches for wrist pain

Simple exercises like tendon glides and finger lifts can have a big impact

They can last 10 to 15 years, but factors like age and activity level can impact their longevity

Your metabolism may torch 1,300 to 2,000 calories daily with no activity

A gentle touch in all the right places may help drain your sinuses