Advertisement
A neurostimulator implant can help head off seizures
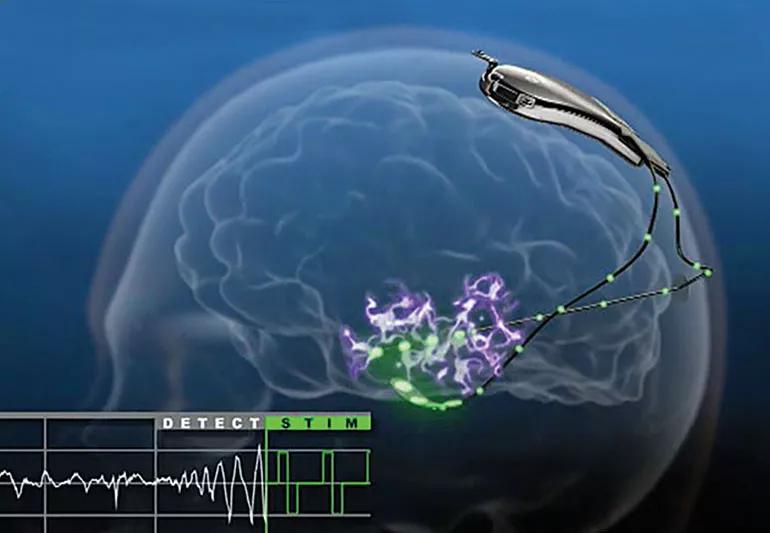
If you have treatment-resistant epilepsy, you may benefit from recent advances in surgical procedures, specifically, FDA approved responsive neurostimulation (RNS).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The treatment can alleviate epilepsy for some patients with partial onset seizures that have not been controlled by two or more medications and are not candidates for surgical resection. The treatment is an alternative for patients who have no other surgical options.
During this procedure, surgeons implant a device that provides responsive neurostimulation (RNS).
The RNS device has “the potential to improve seizure control in patients with difficult to control epilepsy,” says neurological surgeon William Bingaman, MD, Head of the Section of Epilepsy Surgery at Cleveland Clinic. “Approximately 50% to 60% of patients have had good results.”
The device has the potential to improve the quality of life for the hundreds of thousands of people in the United States who suffer from some forms of epilepsy that cannot be helped by medications.
Surgeons first remove a portion of the skull so they can insert a thin metal tray that holds the neurostimulation device, which measures about 6 centimeters by 4 centimeters — about the size of two small postage stamps.
Surgeons then implant the device into the tray. They also implant electrodes connected to the device into the brain in the region where a pre-surgery assessment has indicated the seizures originate.
The device provides a continuous electroencephalogram (EEG) recording, which measures the electrical activities between brain cells that are communicating with each other. The device also contains a seizure detection program that identifies abnormal epileptic electrical activities in your brain.
If the device detects epileptic/seizure activity, it delivers low levels of electrical stimulation that you cannot feel, but returns your brain activity to normal before a seizure occurs.
“While I’d like to see the success rate be 80% to 90% of patients, it’s helping a lot of patients who had 0% success with medicine,” Dr. Bingaman says. “It’s a new and very exciting option.”
RNS also can help patients with bi-temporal epilepsy, a condition that is very difficult to treat, Dr. Bingaman says. For these patients, epilepsy originates in two lobes of the brain. Removing one lobe doesn’t help, and surgeons can’t remove two.
“Now, with these patients, we can remove one lobe and implant the device to stimulate the other, or we can implant it to stimulate both,” he says.
In recent years, surgeons also have treated two types of epilepsy with laser ablation. Using magnetic resonance imaging (MRI) to guide them, surgeons can reach a deep part of the brain through minimally invasive surgery.
Advertisement
In this procedure, surgeons insert a guidance catheter through a tiny hole in the skull into the temporal lobe where scar tissue is causing seizures. Then the surgeons insert a laser with a tip that can deliver different amounts of heat to remove the tissue.
Surgeons perform these procedures in an intraoperative MRI suite. They use the MRI to see inside the brain so that they can ensure the correct placement of the laser device. They also can see when the laser has destroyed the scar tissue.
The procedure also can treat children with hypothalamic hamartoma, a benign tumor or wart in the hypothalamus portion of the brain. This type of growth causes seizures that sometimes cause delays in the child’s development.
“We can use the laser to ablate or remove it, rather than doing an open craniotomy,” Dr. Bingaman says. “It’s right in the middle of the brain, so it’s a hard place to reach surgically.”
Advertisement
Learn more about our editorial process.
Advertisement

There are times and cases when physician-supervised breaks may be beneficial

Eating mindfully, sipping water and chewing slowly can help your brain catch up with your stomach

Seizure symptoms can go far beyond convulsions and may include feelings of déjà vu, temporary confusion and unusual movements

They can feel like a typical headache or a migraine headache, but the pain can last for weeks to months
It’s always a good idea to let a healthcare provider know about any back pain you’re experiencing, especially if it results from trauma or persists longer than three months

It’s all about the amount — try to stick to 100 to 150 milligrams a day to reduce and prevent a pounding, throbbing head

Even one drink can have an impact on your cognitive function leading to slurred speech, blurred vision and impaired memory

Among the options is a fast-acting medication that offers relief in as little as 15 minutes

Your metabolism may torch 1,300 to 2,000 calories daily with no activity

A gentle touch in all the right places may help drain your sinuses