3 kinds of blisters and how to treat them (Spoiler: Popping them isn’t best the answer)
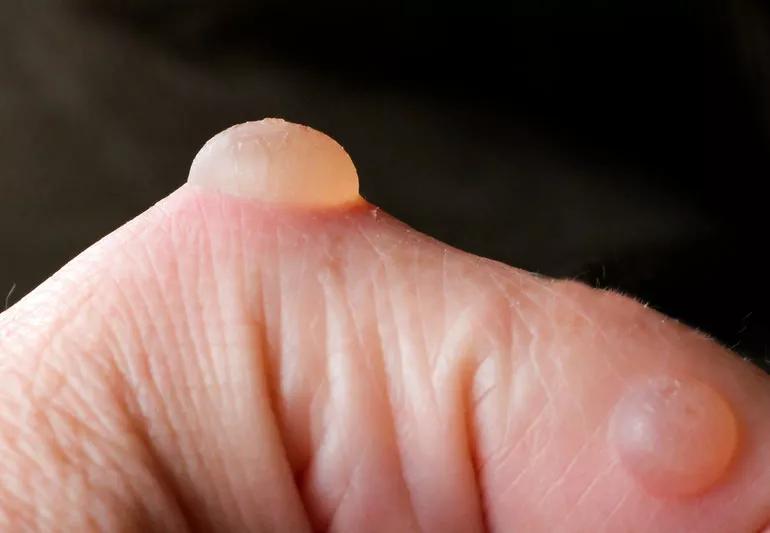
Blisters, am I right? We all get them. Maybe you wore shoes that weren’t quite right for your feet. Maybe that baking sheet wasn’t quite cool enough to handle. Or maybe you have a medical condition or a viral infection that causes flare ups of blisters.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Wherever they came from, the temptation to pop a blister may just get the best of you. But experts say that’s usually not your best bet.
We talked with dermatologist Shilpi Khetarpal, MD, about why you shouldn’t pop most blisters and how, instead, to treat three common kinds of blisters.
The short answer? In most cases, a big ol’ nope.
“Blisters are your body’s way of forming a bandage after an injury,” Dr. Khetarpal says. “The fluid in the blister helps to prevent further damage to the skin below and allows the skin to heal.”
In most cases, you’re best off letting a blister heal on its own. But the American Academy of Dermatology (AAD) says you can drain a blister if it is “very large and painful.”
Popping or draining a blister can lead to infection, so if you absolutely must do it, take care to keep it clean.
Certain people at risk for infection should consult their healthcare practitioner to drain a blister. They will use a sterile needle to allow fluid to drain. This is especially important for people with compromised immune systems, including:
Advertisement
If your blister bursts, naturally or otherwise, you’ll want to take care to ensure it heals properly and doesn’t become infected.
Don’t peel off the dead skin. Leave it in place to shield the skin underneath from dirt, debris and bacteria.
Allow the fluid to drain naturally and then cover the area with a dry, sterile bandage to promote healing and keep it clean.
Blisters can often be a result of repetitive friction, like from shoes or gloves. They’re also common after being burned. And some medical conditions can cause blistering, too.
Dr. Khetarpal helps explain the causes of these different kinds of blisters, how to prevent them and how to treat them.
It’s a common scenario. You’ve laced up your brand-new running shoes. But 10 minutes into your run, you feel a painful rub. The next morning, you see it: The angry, red skin has puffed up and is a fluid-filled sac.
Friction blisters commonly form on your toes, feet and ankles after wearing shoes that are too tight or too loose. (It’s a Goldilocks kind of thing … you want them to fit juuuust right.) Even with a proper fit, though, some new shoes are more likely to cause blisters than your worn-in favorites. Materials like leather, for example, need some time to wear in and soften to mold to your feet.
Friction blisters may also form on your palms or fingers after working with your hands, like when shoveling, gardening or performing other hands-on tasks.
The AAD suggests these steps to prevent nagging and painful friction blisters:
Again, popping your blister shouldn’t be the go-to. Try these methods instead:
First things first, if you suffer a minor burn — say in an ill-conceived attempt to remove a hot pan from the stove — start by cooling down the area. Fast.
“When you get burned, your first course of action should be to run the burn under cool water,” Dr. Khetarpal says. “That will help with the pain and can also reduce swelling.”
Keep the burned area in cool water for about 5 minutes or until the pain stops. Don’t use ice or icy water, which can further damage the tissue.
The AAD suggests not popping a burn blister. Instead, try these fixes:
Advertisement
If the burn doesn’t improve in two weeks or causes severe pain, contact a healthcare provider for further help.
Certain conditions and viruses can cause patches of blisters or full-body blistering. They include:
Treatments vary for these conditions but in almost no circumstance should you pop, drain or itch these blisters. Talk with your healthcare provider about options to manage a blistering condition. They may recommend medications, ointments and other management strategies.
The depth of the blister determines whether or not it will scar.
“The deeper the injury (particularly when it comes to a chemical or heat burn), the more likely it is for a scar to form,” Dr. Khetarpal says. “Typically, friction blisters do not scar as they tend to be more superficial.”
Most blisters can be treated at home. If your blister is particularly large and painful, consider talking with a healthcare provider before choosing to drain it yourself, especially if you are living with a condition that puts you at a higher risk for infection.
Advertisement
Also talk with a healthcare practitioner if:
Advertisement
Learn more about our editorial process.
Advertisement

Both inflammatory conditions have varying triggers and symptoms

Keeping your skin dry, wearing the right clothes and investing in anti-chafe products can help minimize skin irritation

Working with a therapist, staying active and practicing mindfulness are just a few ways to help manage stress

Laser hair removal, laser surgery, excision and steroid injections are all potential treatment options

Use products that reduce inflammation without causing irritation and avoid fragrances, dyes and exfoliators

Nutrition plays an important role in managing this chronic inflammatory skin disease

Aloe vera, warm compresses and diet adjustments can help alleviate symptoms

Popping or prodding at these cysts could lead to infection

The tropical fruit is a good source of antioxidants and vitamin C

Most people fall asleep within 10 to 20 minutes, but if your experience is different, adjusting your sleep schedule may help

Exploring your hidden side can lead to better understanding of what makes you tick