Early detection and screening are important
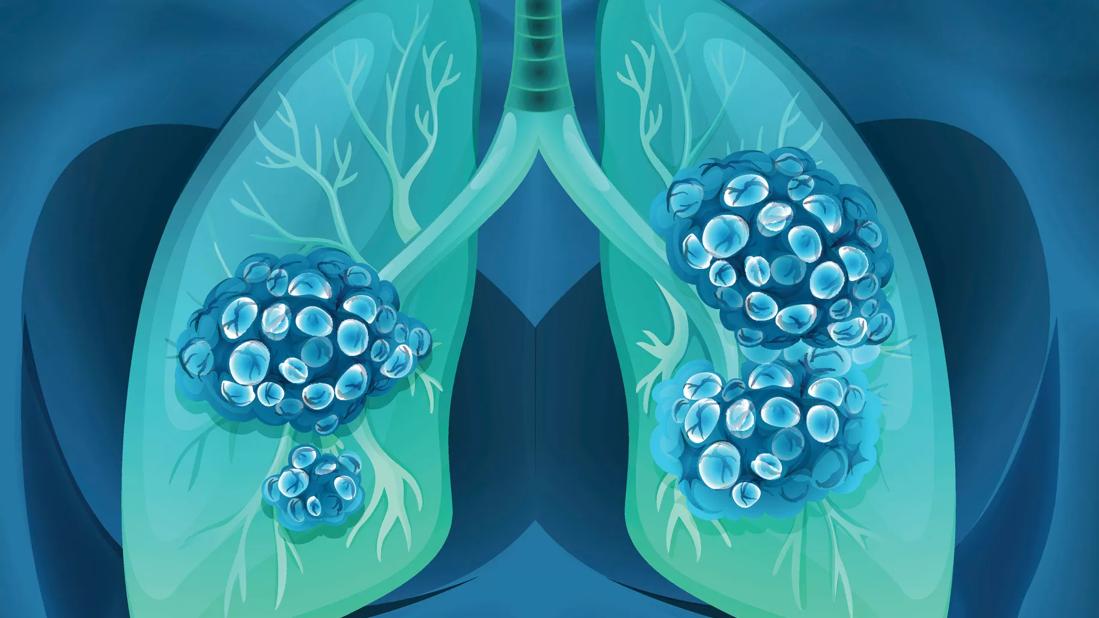
If you’re worried because tests show that you have a lung nodule, keep in mind that the vast majority of pulmonary nodules aren’t cancerous. In fact, only 3 or 4 in 100 of these small growths are cancerous.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
But it’s important to follow up on it because lung cancer remains the leading cause of cancer deaths for both men and women in the United States. The disease takes more lives than colon, breast and prostate cancers combined.
And, while smoking cigarettes is the most common risk factor for developing lung cancer, 25% of all cases worldwide are found in people who have never smoked.
Here’s what you need to know about early detection and screening — the key to allowing doctors to identify and treat a nodule that is cancerous in its early stages.
Lung nodules are soft-tissue lesions that can be either rounded or irregular in shape. A nodule is defined as a lesion measuring 3 centimeters or smaller in diameter, says lung specialist Louis Lam, MD. (Anything larger than 3 centimeters is considered as a mass.)
Nodules are typically detected with routine chest imaging during an annual check-up or when you have a respiratory illness or unrelated doctor visit.
They can show up either on a chest X-ray or computed tomography (CT) scan. “We generally don’t expect to see symptoms,” Dr. Lam says.
Many doctors recommend an annual CT scan for those at high-risk for lung cancer. This scan is more effective in detecting the disease early in its course when it is treatable.
Medicare guidelines state that you’re eligible for a low-dose screening CT once a year if you are:
Advertisement
Dr. Lam says patients should know that there is a slight risk of radiation exposure from a CT scan and a small chance of “false-positives” that sometimes cause additional testing or surgery on a nodule that is non-cancerous.
But he says the risks are worth it when weighed against the benefits of such a screening. The National Lung Screening Trial found a 20% reduction in lung cancer related death rates in high-risk patients who had CT screening over those who had chest X-rays, he says.
When testing detects a nodule or spot, your doctor likely will continue checking the nodule for two years. The recommended course of action, however, will depend on the size of the nodule and your risk level.
For instance, a person with a small nodule who is at low risk might have a follow up CT scan annually for two years. But a high-risk individual might have three CT scans during that period.
If the nodule does not grow over the two-year period, your doctor likely will diagnose it as benign and will not treat it further, Dr. Lam says. If growth is detected, a biopsy or surgery would be recommended. In general, malignant nodules double in size every one to six months.
“The bulk of nodules are benign,” he adds. (Lung cancer rates vary by state due to several variables, including socioeconomic status, lifestyle choices and exposure to radon, the second leading cause of lung cancer.)
But even if the nodule is not cancerous, Dr. Lam uses the experience as an opportunity to educate patients about the dangers of smoking.
One study found that people who smoke lose at least one decade of life expectancy compared with people who have never smoked. It also found that people who quit smoking by age 40 reduce their risk of smoking-related death by 90%.
Advertisement
Learn more about our editorial process.
Advertisement

Some tips to make your next fire safer
The right treatment starts with the right diagnosis

There’s no safe way to identify, handle, repair or remove asbestos yourself — it’s always a job for a professional

Mold exposure can cause allergic reactions, asthma and skin rashes

Many claims lack science-backed research, but halotherapy is popular and considered safe

Both are respiratory infections, but bronchitis affects your bronchial tubes, while pneumonia affects the air sacs in your lungs

Breathing in toxic smoke can lead to serious health problems

From dental diseases to cardiovascular problems, the harmful effects of smoking hookah have plenty of downsides for your health

If you’re feeling short of breath, sleep can be tough — propping yourself up or sleeping on your side may help

If you fear the unknown or find yourself needing reassurance often, you may identify with this attachment style

If you’re looking to boost your gut health, it’s better to get fiber from whole foods