Symptoms can feel like long COVID or the flu, with body aches or even nerve damage
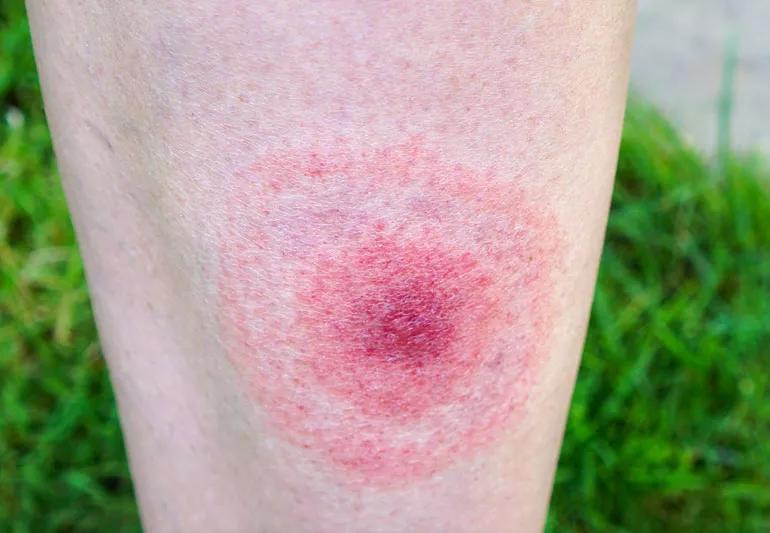
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/b2ce45e8-8818-41db-93e6-25fcf6e5c672/lymeDiseaseRash-597213730-770x553-jpg)
Bullseye-like rash on leg from lyme disease infection
If you don’t notice a tiny deer tick bite on your body, it’s easy to dismiss the symptoms of Lyme disease. Headaches, body aches, fatigue, fever — you assume you just have the flu. So, you lay low and give it a week or so, thinking it will resolve on its own. But by then, the bacterial infection from a tick bite has had time to spread.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Primary care physician Daniel Sullivan, MD, walks us through the experience of Lyme disease, and the sometimes complicated healing process.
Video content: This video is available to watch online.
View video online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_v4l3nw2h/flavorId/1_5f3sgelj/format/url/protocol/https/a.mp4)
Lyme disease, spread by blacklegged ticks, can start with rash, fever, chills and aches. Early antibiotics can cure it and prevent complications.
The bacterium Borrelia burgdorferi causes Lyme disease when it gets into your bloodstream. You may experience a variety of symptoms, depending on the stage of the infection.
“The human body reacts the same way to many different things,” Dr. Sullivan says. “If you get the flu, you get a low-grade fever, develop muscle aches and feel a little off. And if you are infected with the Lyme bacteria, you can feel the same way.”
Early on, typical symptoms of Lyme disease include fever, chills, headache, joint aches and — most distinctively — a spreading rash that resembles a bullseye.
But if it isn’t identified and treated within 36 to 48 hours, the infection can spread to other parts of your body, including your heart and nervous system.
The later, more serious stages of Lyme disease can lead to neurological damage and arthritis.
With treatment, Lyme disease does go away. But the process can look different from person to person and situation to situation.
Most people get lucky, according to Dr. Sullivan. They notice the bullseye rash, seek treatment immediately and that’s the end of the story.
Advertisement
“During the early stages of Lyme disease, oral antibiotics can treat the infection. So, most patients will recover quickly and completely,” he says. “But if that rash goes unnoticed, the infection will progress, affecting the muscles, joints, heart and nerves.”
Whether a doctor identifies the disease in its early stages or later on, the first step is treating the infection with antibiotics.
“In most cases where the disease has spread, once the infection is treated, the inflammation and the irritation to the nerves, heart and joints will slowly resolve over time,” Dr. Sullivan explains. “Most patients are on antibiotics for between 10 days and two weeks. If it affected the heart or spinal fluid, it’s a four-week course.”
Once antibiotics resolve the infection, you can support your recovery from Lyme disease as you would with any kind of arthritis flare or nerve injury. Dr. Sullivan recommends that you:
“The damage Lyme disease causes to your nerves or muscles will heal over the course of several months,” he continues. “Identifying the infection and treating it is the first step. Once it’s clear, the body can start the healing process.”
You’re probably familiar with post-COVID syndrome — also known as long COVID. Post-treatment Lyme disease syndrome (PTLDS) is a similar condition. People living with PTLDS don’t still have Lyme disease. The infection is gone. What they do have are lingering symptoms that can take months to go away. According to the American Medical Association, for reasons we don’t yet understand, some people’s symptoms even continue past the six-month mark.
Somewhere between 5% and 15% of people diagnosed with Lyme disease go on to develop PTLDS. But, as the U.S. Centers for Disease Control and Prevention (CDC) notes, it’s important that you don’t assume that’s the reason you’re still feeling unwell. There are lots of medical conditions that cause similar symptoms. Let your healthcare provider know what’s happening so they can run tests and rule out other possibilities.
If your healthcare provider determines that you have PTLDS, it can be hard to know what to expect in the weeks and months ahead. As you recover, your symptoms may come and go or vary in intensity. Consider tracking them, along with your daily activities, in a journal. You might stumble upon a few kernels of wisdom that help you better manage stubborn symptoms.
Advertisement
It’s important to note that some patient advocacy sites argue that long courses of antibiotic therapy (up to six months) can resolve PTLDS. But Dr. Sullivan and the CDC say there’s no evidence to support extending the treatment beyond four weeks.
“Within four weeks, the antibiotics will kill the bacteria,” Dr. Sullivan says. “A longer course of antibiotics could potentially cause more harm than good.”
It’s natural to be frustrated when there’s not much to do but wait and troubleshoot symptoms. And it’s important that people living with PTLDS receive support and understanding from their friends, loved ones and providers. Their symptoms are real — and they can have an equally real impact on their mental health.
If you have PTLDS and notice that you’re isolating yourself from others, feeling sad, angry or hopeless, or that you’re showing other signs of depression, don’t wait to reach out for help. The provider treating you needs to know, not only because neurological symptoms are common in PTLDS, but also because your mental health is just as important as your physical health. Your provider may encourage you to join a Lyme disease support group or refer you to a mental health professional for additional support.
Advertisement
Lyme disease is a bacterial infection that some (but not all) deer ticks carry. If a deer tick bites you, seek immediate medical attention. The sooner you receive antibiotics, the less likely the disease will progress. If you don’t realize you’ve been bitten, an infection can spread — and you can develop increasingly serious symptoms.
But no matter how severe your condition may become, treatment remains the same: antibiotics. Once the infection is gone, the healing process can begin. Recovery may be slower for some than others, with symptoms continuing for weeks or months after the infection is cured.
In these circumstances, symptom management and mental health support are key, so it’s important to be open with your doctor and your loved ones. They can help ensure that your recovery process is as safe and healthy as possible.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about our editorial process.
Advertisement
If you find a tick attached to your skin, pulling it out the right way can lower your risk of infection
Taking proper precautions — like wearing long pants and using bug spray — can protect you against Lyme disease and other tick-borne illnesses
Keep ‘mozzies’ at bay by avoiding scented body products, beer and certain colored clothes
Vanilla extract won’t keep mosquitoes away for long, if at all — and could even attract other bugs, like wasps or flies
Alpha-gal syndrome has become more common and is a leading cause of anaphylaxis
These red, raised bites often show up in a zigzag pattern on areas of your skin that come into contact with bedding
Bug bites create tiny openings in your skin that can let in dangerous bacteria
Using insect repellent, covering up and keeping your property dry can help keep the buggers at bay
The virus that causes the so-called ‘stomach flu’ can cling to surfaces for days or even weeks
There isn’t clear evidence that melatonin harms your heart — but finding the cause of sleep issues is key to long-term heart health
Your dollar bills, coins and cards are covered in germs — but they’re very unlikely to make you sick