A combination of treatments can help you conquer the compulsion
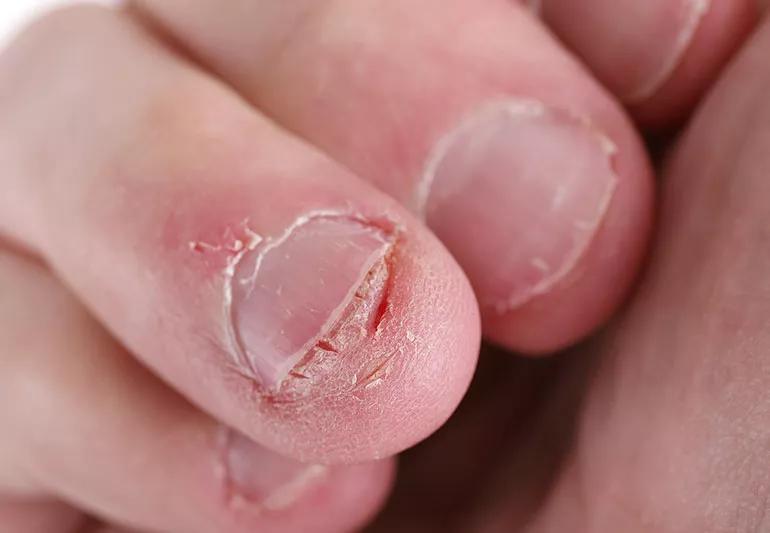
Do you find yourself absentmindedly chewing on or biting your fingernails — and when you try to quit the habit, it just doesn’t take?
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Rest assured that you’re not alone. Although to many people, nail biting is an occasional thing, for 20% to 30% (or more) of Americans, nail biting is a behavior they can’t stop on their own.
In fact, healthcare providers classify chronic nail biting as a type of obsessive-compulsive disorder or a body-focused repetitive behavior (BFRB). There’s even a name for chronic nail biting: Onychophagia.
Although providers don’t fully understand the cause of chronic nail biting, there are ways to halt the habit.
Preventive medicine physician and wellness expert Sandra Darling, DO, shares tips on how to stop nail biting.
When you’re a chronic nail biter, you often want to stop — and may have even made multiple attempts to quit, without success.
But people with onychophagia can’t stop the behavior on their own. In other words, it doesn’t help to tell someone to stop — and reprimanding them only makes them feel worse because it reinforces their feelings of being flawed.
But you can get closer to recovery with repeated effort and self-care. Dr. Darling usually recommends a combination treatment approach that includes:
Therapy can help release the shame and negative emotions that often accompany nail biting. It can also help increase awareness of your triggers and urges. In some cases, habit-reversal training or hypnotherapy are effective.
Advertisement
Self-care — like regular meals, more movement and ample sleep — helps you feel calmer, more confident and resilient, giving you the strength to recover. Nail biting satisfies a strong urge, so to quiet your mind and ease the tension created by the urge, we recommend meditation, journaling and yoga.
Talking to a support buddy when you feel the urge to bite your nails can help you get through the stressful moment. The TLC Foundation for Body-Focused Repetitive Behaviors offers a directory of support groups and educational events.
People with chronic nail biting may need medications or behavioral therapy to address a related condition. We do know that people with the following conditions often have onychophagia as well:
Let’s face it, nail polish doesn’t taste good. But there is actually a variety of nail polishes made specifically to deter you from biting your nails. This polish tastes particularly bitter or foul on purpose — and people have found it to be an effective way to stop biting.
Chronic nail biting often has a self-soothing quality — in fact, it provides a sense of calm — so people may use it as a coping mechanism.
Sometimes, a hangnail or nail imperfection spurs you to groom a nail excessively, in order to improve the look of your nail. Unfortunately, this often makes the nail look worse.
People also bite their nails when feeling stressed or bored, while watching TV or when focusing on a task like reading.
You should seek medical treatment if nail biting is causing physical damage to your nail, cuticle or surrounding skin, or if there are signs of an infection (including redness, pain or swelling).
If nail biting is causing you psychological distress, such as shame, anxiety, depression or low self-esteem, a mental health provider can help. It’s important to discuss your concerns with a professional if the behavior is affecting your social life, too, or affects your professional life or job performance.
Advertisement
Learn more about our editorial process.
Advertisement

Color, texture or shape changes may signal a larger medical issue
Safety, hygiene and technician training are among the biggest benefits of a ‘medi pedi’
These manicure techniques vary in terms of longevity, hygiene and overall nail health

The temporary nail damage is bad, but the cumulative UV exposure could be worse

Animal safety and bacterial infections are concerns

Resist the urge to bite, tear or rip off those little pieces of skin

Frequent manicures, high-watt bulbs increase potential

Make sure your salon is clean and sterilizes its instruments

Wearing a scarf, adjusting your outdoor activities and following your asthma treatment plan can help limit breathing problems

Your diet in the weeks, days and hours ahead of your race can power you to the finish line

When someone guilt trips you, they’re using emotionally manipulative behavior to try to get you to act a certain way