What’s the difference between these types of arthritis?

You have psoriasis, and now you’re experiencing joint pain. Does this mean you have psoriatic arthritis? Or could it be unrelated?
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Osteoarthritis is the most common type of arthritis, and, sometimes, it can occur alongside psoriasis. Then again, psoriatic arthritis is also a possibility if you are experiencing skin symptoms,” says rheumatologist Rochelle Rosian, MD.
How can you make sense of it all? We talked to Dr. Rosian to find out what these types of arthritis have in common, how they differ and how to treat them.
“The word ‘arthritis’ is kind of a catch-all term,” Dr. Rosian explains. It’s used to describe more than 100 different conditions that cause pain, swelling and joint damage. Osteoarthritis and psoriatic arthritis are two of those many conditions.
Osteoarthritis, or degenerative joint disease, is the most common type of arthritis. It occurs when the cartilage that cushions your bones wears down, leaving bone to rub against bone.
Since it’s caused by wear and tear on the joints over time, it usually develops in older adults. Unlike psoriatic arthritis, osteoarthritis doesn’t involve inflammation or an overactive immune system.
Common features of osteoarthritis include:
Advertisement
The location of the pain depends on the type of osteoarthritis:
Psoriatic arthritis is a type of inflammatory arthritis. It occurs when your body’s immune system works overtime, creating inflammation throughout your body. In psoriatic arthritis, that inflammation targets the joints and the places where tendons and ligaments attach to bones.
Most people with psoriatic arthritis also have psoriasis, a disease that causes red, scaly patches of skin. Psoriatic arthritis can strike at any age, though symptoms usually develop between ages 30 and 50.
Psoriatic arthritis causes symptoms in your joints and beyond, including:
Joint symptoms:
Skin symptoms:
Other symptoms:
In osteoarthritis, X-rays may show signs like worn cartilage. In psoriatic arthritis, X-rays can show joint damage in later stages of the disease.
But they aren’t especially helpful in making a diagnosis in the early stages. “X-rays can help make an arthritis diagnosis. But they aren’t always a slam dunk,” Dr. Rosian says.
X-rays can also reveal bone spurs, which can develop in people with osteoarthritis and psoriatic arthritis. Those images may reveal differences between the two diseases:
To diagnose joint disease, your healthcare provider will probably consider several factors in addition to X-rays, including:
Getting an accurate diagnosis is important since psoriatic arthritis and osteoarthritis require different treatments.
Advertisement
Medications are often an essential part of treating arthritis. But the medications can differ depending on the type.
Treatments for osteoarthritis include:
Treatments for psoriatic arthritis include:
In addition to medication, you can take other steps to manage arthritis symptoms. These approaches can help whether you have psoriatic arthritis or osteoarthritis:
“By making certain lifestyle changes and working with your doctor to develop a treatment plan, you can keep arthritis symptoms in check,” says Dr. Rosian.
Advertisement
Learn more about our editorial process.
Advertisement

Choose foods high in omega-3s and antioxidants; avoid red meat and dairy

Cold or hot therapy, massage and exercise may help reduce pain and inflammation in your joints

Focus on sleep, limit alcohol and reduce your stress and anxiety to help lessen symptoms
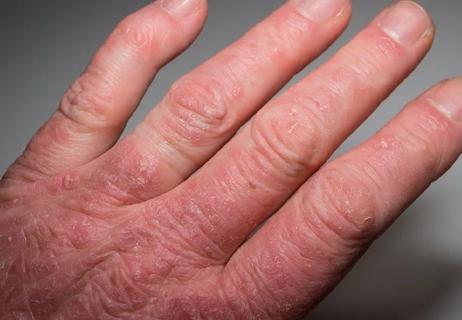
What’s the difference between these types of inflammatory arthritis?

The link between joint pain and skin rashes
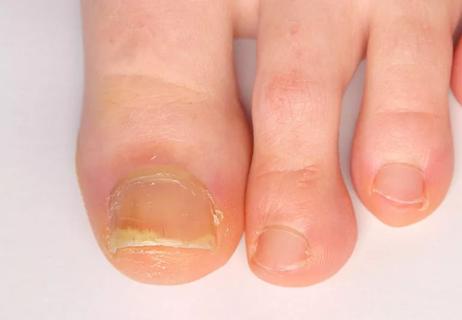
Symptoms of nail psoriasis and how to treat it

Managing psoriatic arthritis foot pain

Does arthritis make you tired?

Wearing a scarf, adjusting your outdoor activities and following your asthma treatment plan can help limit breathing problems

Your diet in the weeks, days and hours ahead of your race can power you to the finish line

When someone guilt trips you, they’re using emotionally manipulative behavior to try to get you to act a certain way