What’s the difference between these types of inflammatory arthritis?
Psoriatic arthritis and rheumatoid arthritis are easy to mix up. Both cause pain, swelling and stiffness in the joints. But they’re more like siblings than identical twins.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Rheumatoid arthritis and psoriatic arthritis share some common symptoms. But they are distinct diseases,” says rheumatologist Rochelle Rosian, MD. “Getting a correct diagnosis will help your provider develop a more personalized treatment plan.”
People talk about arthritis as though it’s one disease. But the term can describe a wide variety of conditions like:
Osteoarthritis is the most common form of arthritis. (If psoriatic arthritis and rheumatoid arthritis are siblings, think of osteoarthritis as their distant cousin.) Osteoarthritis is caused by wear and tear on the joints over time and is most common in older adults.
This category is where you’ll find psoriatic arthritis and rheumatoid arthritis, both diseases that involve your immune system. They occur when your body’s immune system mistakenly attacks healthy tissues, including your joints.
Psoriatic arthritis and rheumatoid arthritis share several features. “Both diseases cause joint pain and swelling,” Dr. Rosian says. “And in both cases, symptoms usually show up suddenly in episodes called flares, before eventually calming down again.”
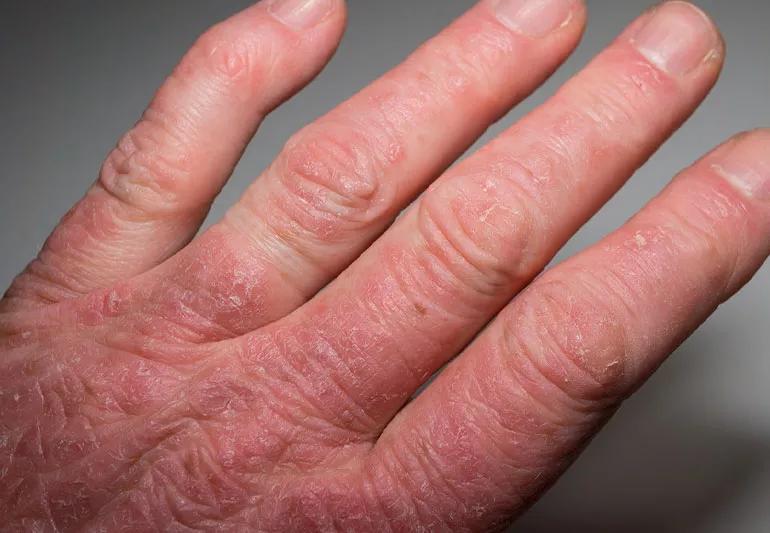
Psoriatic arthritis affects your joints and the places where tendons and ligaments attach to bones. Many people with psoriatic arthritis also have psoriasis, a disease that causes scaly, flaky patches of skin.
Advertisement
About 30% of people with psoriasis will develop psoriatic arthritis. Symptoms can develop at any age but usually show up between ages 35 and 55. It affects men and women equally. The arthritis can occur before the skin disease or with mild skin involvement, such as only nail or scalp psoriasis.
Common symptoms of psoriatic arthritis include:
Rheumatoid arthritis causes pain, swelling and stiffness in your joints. It usually affects the same joints on both sides of your body, such as both thumbs or both wrists. Sometimes, it also affects internal organs.
Rheumatoid arthritis is more than twice as common in women as in men. It can develop at any age but most often develops between ages 20 and 50.
Common symptoms of rheumatoid arthritis include:
While symptoms of psoriatic arthritis and rheumatoid arthritis can overlap, there are some notable differences:
Doctors look at several factors to determine whether your symptoms are psoriatic arthritis or rheumatoid arthritis.
Researchers believe both psoriatic arthritis and rheumatoid arthritis are caused by a mix of genetics and environmental factors. Your doctor may ask if you have a history of psoriasis or if anyone in your family has psoriasis, psoriatic arthritis or rheumatoid arthritis.
Blood tests can help your doctor determine which type of arthritis you have. People with rheumatoid arthritis often have a protein called rheumatoid factor in their blood. People with psoriatic arthritis usually don’t.
Another test looks for CCP antibodies, sometimes called anti-CCP antibodies. These can be a sign of rheumatoid arthritis.
X-ray images of psoriatic arthritis and rheumatoid arthritis can look similar. But since the diseases tend to affect different joints, X-rays can help pinpoint a diagnosis. The images can also reveal other differences between the diseases:
Several medications work for both psoriatic arthritis and rheumatoid arthritis:
As researchers learn more about the causes of inflammatory arthritis, they’re developing new medications to manage these diseases. Some of these new drugs are designed to specifically target one disease or the other.
Advertisement
“Both psoriatic arthritis and rheumatoid arthritis are chronic diseases. They can’t be cured, but they can be managed,” Dr. Rosian says. “By working with your doctor to get the correct diagnosis, you can manage symptoms to feel your best.”
Advertisement
Learn more about our editorial process.
Advertisement

Choose foods high in omega-3s and antioxidants; avoid red meat and dairy

Cold or hot therapy, massage and exercise may help reduce pain and inflammation in your joints

Focus on sleep, limit alcohol and reduce your stress and anxiety to help lessen symptoms

The link between joint pain and skin rashes
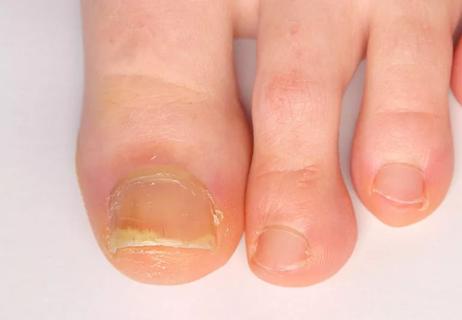
Symptoms of nail psoriasis and how to treat it

What’s the difference between these types of arthritis?

Managing psoriatic arthritis foot pain

Does arthritis make you tired?

Wearing a scarf, adjusting your outdoor activities and following your asthma treatment plan can help limit breathing problems

Your diet in the weeks, days and hours ahead of your race can power you to the finish line

When someone guilt trips you, they’re using emotionally manipulative behavior to try to get you to act a certain way