The link between joint pain and skin rashes

You have swollen, painful joints. It might be a sign of psoriatic arthritis. But you don’t have the telltale skin rash that signals psoriasis. Could you have one condition without the other?
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Psoriasis and psoriatic arthritis are related conditions, but they don’t always strike at the same time,” says rheumatologist Ivana Parody, MD.
Here’s what to know about psoriasis and psoriatic arthritis and how they fit together.
Video playlist content: This video playlist is available to watch online.
View video playlist online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_qg0j86ei/flavorId/1_5f3sgelj/format/applehttp/protocol/https/a.mp4)
Learn more about psoriatic arthritis, it's symptoms and possible treatment options.
Psoriatic arthritis is an autoimmune disease. It occurs when your body’s immune system attacks its own tissues. The disease causes pain and swelling in your joints and the places where tendons and ligaments attach to bones. It can develop at any age, but most people experience their first symptoms between ages 35 and 55.
So, where does the skin come into play? Psoriasis is an autoimmune disease that affects your skin. It causes red, itchy, inflamed patches of skin that can be covered with silvery scales.
Psoriasis is common on the elbows, knees and scalp but can show up just about anywhere on your body. Most people with psoriasis never get psoriatic arthritis. But about 30% of people with psoriasis do develop the disease.
“It’s possible, but not very common,” says Dr. Parody. Most people develop psoriasis first. Psoriatic arthritis typically emerges about seven to 10 years later.
That’s not always the case, however. A small number of people have joint pain first, and the skin disease appears later. It’s even possible that a person with psoriatic arthritis will never have any skin symptoms. “But that doesn’t happen often. When it does, there is usually a family history of psoriasis,” Dr. Parody says.
Advertisement
Psoriatic arthritis can cause different symptoms from person to person. But there are several common symptoms:
Experts aren’t sure what causes psoriatic arthritis. They suspect a combination of genes and environmental factors is to blame.
Unfortunately, no single test can identify psoriatic arthritis. It’s usually easier for a doctor to diagnose you if you have psoriasis, as the two diseases often tag team.
Whether or not your skin is involved, your doctor will consider several factors to make a diagnosis. These include:
“If you have painful, swollen joints and other symptoms, start with your primary care doctor,” says Dr. Parody. “They may refer you to a rheumatologist, who specializes in diagnosing and treating arthritis and other diseases that affect the joints, muscles and bones.”
Some psoriatic arthritis treatments will also help calm skin symptoms. But if you have bothersome psoriasis symptoms, it can be helpful to see a dermatologist, too (an expert in skin conditions).
Some people with psoriatic arthritis have mild symptoms. They may be able to control pain and swelling with over-the-counter anti-inflammatory drugs.
People with advanced disease usually need prescription medications. These drugs can relieve symptoms and prevent permanent joint damage. They include:
Besides medications, there are things you can do to help relieve pain and protect your joints:
Advertisement
“There’s no cure for psoriasis or psoriatic arthritis, but you can manage both with treatment. And new medications come out every year,” says Dr. Parody. “By working with your doctor, you can develop a plan to protect your joints and keep doing the things you love.”
Advertisement
Learn more about our editorial process.
Advertisement

Choose foods high in omega-3s and antioxidants; avoid red meat and dairy

Cold or hot therapy, massage and exercise may help reduce pain and inflammation in your joints

Focus on sleep, limit alcohol and reduce your stress and anxiety to help lessen symptoms
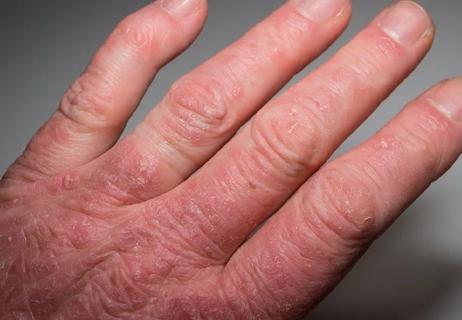
What’s the difference between these types of inflammatory arthritis?
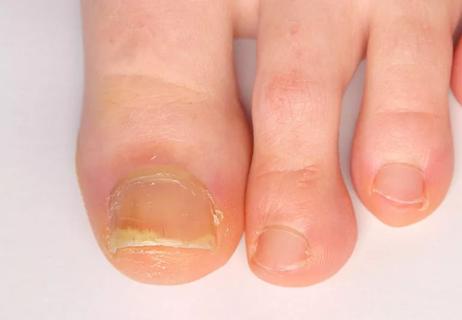
Symptoms of nail psoriasis and how to treat it

What’s the difference between these types of arthritis?

Managing psoriatic arthritis foot pain

Does arthritis make you tired?

The tropical fruit is a good source of antioxidants and vitamin C

Most people fall asleep within 10 to 20 minutes, but if your experience is different, adjusting your sleep schedule may help

Exploring your hidden side can lead to better understanding of what makes you tick