Tough times can become even tougher if they leave an itchy rash on your skin
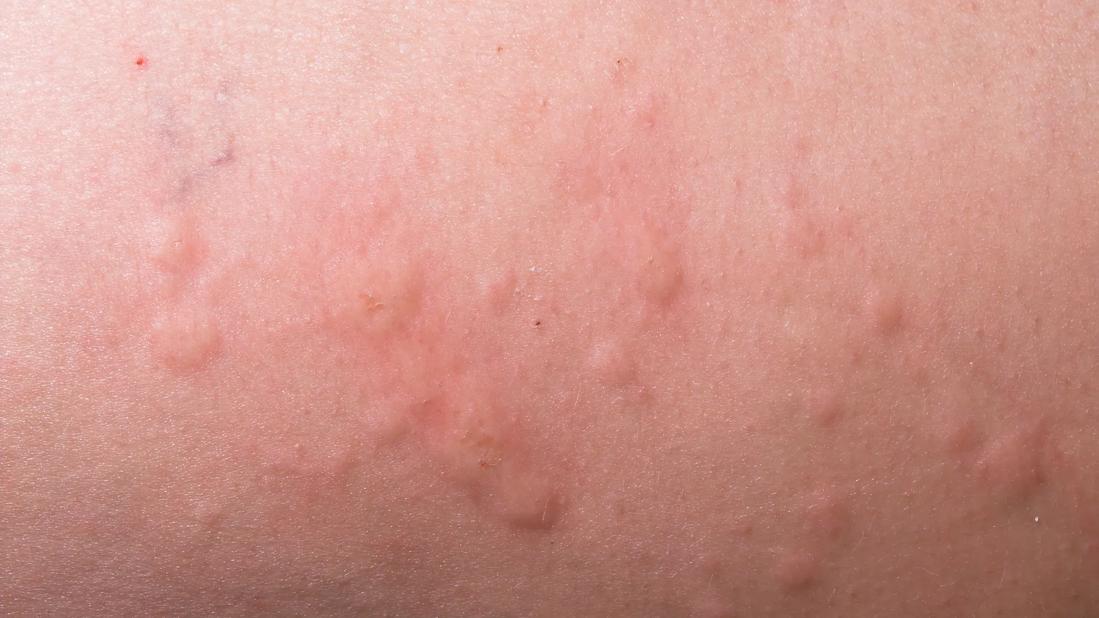
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/1c7be5ff-365b-4ae4-b2bf-4520d31eb4bd/stress-hives-92419172)
Close-up of rash on skin
It’s been a rough-and-tumble week, with stress levels rocketing sky-high. And now, out of nowhere, you’re covered in hives — because dealing with splotchy, itchy skin was just what you needed.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
So, what’s the deal? Well, as it turns out, stress hives are a real thing. Consider the outbreak a physical manifestation of the turmoil you’re experiencing as your body searches for ways to cope.
Family medicine physician Brian Myers, MD, has some tips to help you calm things down.
People tend to think of stress in a mental or emotional context, but it can also bring physical symptoms. Your heart may start racing, for instance, or your stomach may feel a little topsy-turvy.
Those responses reflect your body’s built-in “fight-or-flight” response driven by your autonomic nervous system.
Which brings us to stress rashes and hives.
Your body’s response to stress can include the release of a natural chemical known as histamine. Although this is done as a protective action, the results can have unintended consequences, like hives.
The same process occurs during an allergic reaction, which — not coincidentally — can also bring out hives.
Hives are raised red welts or splotches that appear on your skin. Typically, they’re small — like the size of a fingertip. But individual hives also can cover an area the size of a dinner plate. (Smaller hives may sometimes merge into huge patches called plaques, too.)
Advertisement
Odds are, you won’t just see hives either: You’ll feel them. Hives can itch, burn and even hurt, says Dr. Myers.
Anyone can get stress hives, but they tend to be more common in women. They also seem to most often affect people during their 20s, 30s and 40s.
And if you’ve had allergen-driven hives, you’re more likely to experience stress hives, notes Dr. Myers.
But again, no one is immune. “It can happen to anyone out of the blue,” he says.
The good news? Stress rash often disappears in a day or two. But don’t be surprised if another batch of hives rears up as a replacement — especially if you’re still dealing with your stressors.
Stress hive breakouts may also come and go in waves and can flare up again a few weeks after disappearing.
Dr. Myers offers these suggestions for stress rash treatment:
Remember, too, that stress isn’t the only possible cause of hives. Something unusual you ate could be behind the rash. Or maybe your skin isn’t agreeing with a new shampoo or laundry detergent. It could be something as simple as the heat outside, too.
“Do some sleuthing,” recommends Dr. Myers. “If you think back over the last few days, you might come up with an explanation and solution.”
If hives last longer than a few days despite treatment efforts, talk to a healthcare provider to see what’s going on. And seek immediate medical attention if hives come with symptoms like swelling of your mouth, tongue or lips, as those are signs of a more serious allergic reaction.
The best way to deal with stress hives is to identify and avoid their triggers, says Dr. Myers. Schedule time in your calendar for some self-care to keep stress levels in check. Ask for help when you need it.
“There’s no downside to stress management,” emphasizes Dr. Myers. “Your whole body will thank you for it.”
But to be on the safe side, it might not be a bad idea to keep antihistamines on hand.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about our editorial process.
Advertisement
These tiny saltwater larvae can get trapped under your swimsuit and trigger an itchy reaction called seabather’s eruption
Stress, tight clothing and even sunlight can cause this itchy condition
Treatment is tailored to you and may involve medications like antihistamines, corticosteroids or antidepressants
OTC medications, loose clothing, sun protection and other health habits can help manage flares
The itching and swelling of chronic spontaneous urticaria can disrupt sleep, confidence and daily life — and stress can make symptoms worse
For most people with chronic spontaneous urticaria, diet changes don’t make a meaningful difference
Hormonal changes during your period, pregnancy and more can contribute to hives
A distressed skin barrier can lead to red, itchy and scaly skin
These tiny saltwater larvae can get trapped under your swimsuit and trigger an itchy reaction called seabather’s eruption
Searching nature for edible items requires training and knowledge to avoid poisonous plants
Yes, but you can protect yourself with hats, scarves or even hair sunblock