Advertisement
This time-tested treatment isn’t always on people’s radar
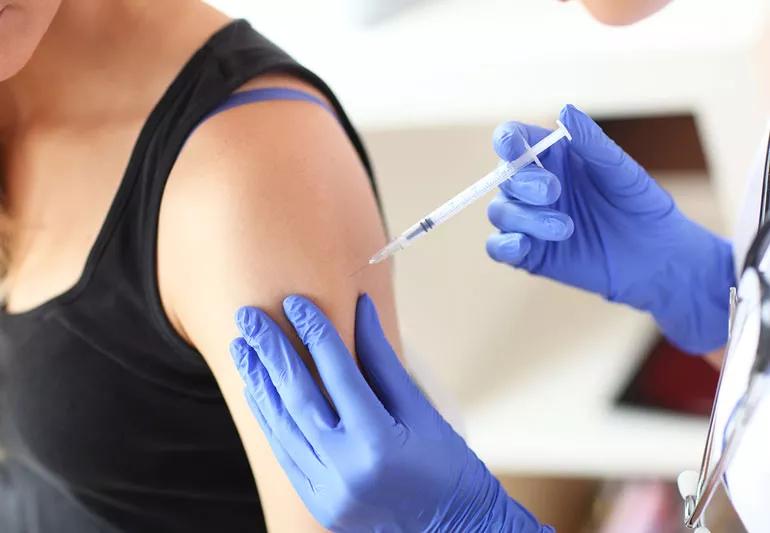
Antihistamines and other allergy medications offer a quick fix for the sneezing, runny nose, itchiness and teary eyes brought on by allergies. But a potentially longer-lasting treatment often goes ignored: allergy shots.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
More formally called allergen immunotherapy, allergy shots work to slowly decrease a person’s sensitivity to certain allergens and reduce their symptoms.
“When it’s impossible to avoid allergy triggers or allergy medicine isn’t working, it may be time to consider allergy shots,” says allergist Ronald Purcell, MD.
Allergy shots can’t protect against food, drug or latex allergies. But they may be able to relieve nose (allergic rhinitis), eye (allergic conjunctivitis) and airway (allergic asthma) symptoms triggered by:
“Evidence suggests that shots may effectively treat itchy skin rashes caused by airborne allergens,” Dr. Purcell says. “They may also prevent people with allergic rhinitis from developing asthma.”
While allergy shots are generally suitable for adults and children over age 5, they aren’t for everyone. People with severe asthma or heart disease, or who need to take medications such as beta blockers, aren’t good candidates for them.
“Your other health conditions and your ability to complete the shot regimen are important considerations,” Dr. Purcell says. “Talk to your physician to see if they’re appropriate for you.”
Like vaccines, allergy shots build up immunity. However, “this is not a quick-fix therapy,” Dr. Purcell cautions. “Shot programs range from three to five years and consist of a build-up phase and a maintenance phase.”
That’s why they’re typically recommended only after you’ve tried medications and taken steps to avoid the things you’re allergic to.
Advertisement
During the build-up phase, you’ll receive injections once or twice a week for three to six months. Each one contains a small dose of the allergen that gradually increases each week. Bit by bit, your body becomes used to the allergen. And, if they’re successful, your symptoms will decrease.
Once you reach the highest dose, you continue getting what are called maintenance shots every two to four weeks.
How long will the benefits of allergy shots last? Three years of treatment can result in tolerance that persists for at least seven years and, for many patients, indefinitely, Dr. Purcell says.
It’s important to consult a board-certified allergist about shots. Very rarely, allergy shots can lead to anaphylactic shock. An allergist’s staff is trained to treat potential systemic reactions such as hives, wheezing or hypotension.
The slight risk of reaction from shots should not be a deterrent, Dr. Purcell says. The allergen extracts used in shots are highly standardized today — they’re produced consistently from batch to batch for reliable quality and dosing.
“Shots have been given for more than 100 years. This is a therapy that has withstood the test of time,” he says.
If your allergies are making you miserable and you are willing to invest the time, consider asking an allergist if shots may be right for you.
Advertisement
Learn more about our editorial process.
Advertisement

Enteroviruses are often to blame for summer colds, leading to a runny nose, sore throat and digestive symptoms

From bug bites and blisters to sunstroke and swimming safety, here’s how to stay well this season

Often, a throat tickle is due to a cold, allergies or GERD — but see a doctor if it won’t go away

A reaction to the medication may trigger preexisting asthma and result in sinus or skin reactions

Autumn allergens typically begin to bloom — and release their pesky pollen — around August

Collect your supplies, wash your hands, prep the site ... and take a deep breath
Sneezing, coughing and clear mucus shouldn’t be ignored

Focus on your body’s metabolic set point by eating healthy foods, making exercise a part of your routine and reducing stress

PFAS chemicals may make life easier — but they aren’t always so easy on the human body

While there’s little risk in trying this hair care treatment, there isn’t much science to back up the claims