MRI improves detection, but it's not yet a substitute for standard biopsy
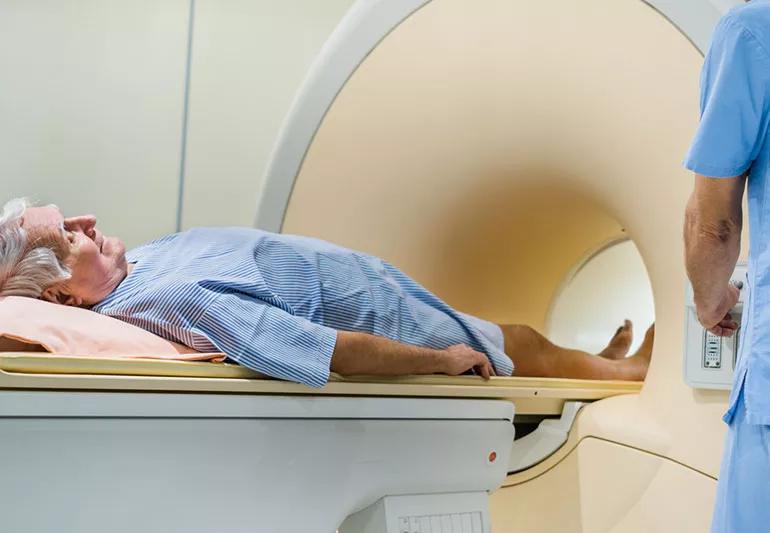
Magnetic resonance imaging (MRI) is used to diagnose an array of medical conditions. Today, medical experts are combining a type of imaging known as multiparametric MRI with traditional transrectal ultrasound (TRUS) prostate biopsy in an effort to diagnose prostate cancer more accurately and effectively. Some advocate using MRI to triage men undergoing an initial prostate biopsy.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
However, despite research suggesting that MRI can improve the accuracy of conventional prostate biopsy, it has limitations, and its usefulness in some clinical situations remains in question, says Eric A. Klein, MD, Chairman of the Glickman Urological & Kidney Institute.
“The value of MRI is that it shows areas that are highly suspicious for cancer and that you should biopsy those areas,” Dr. Klein explains.”There’s no question that MRI makes biopsy more accurate, but it’s not perfect.”
Results of prostate-specific antigen (PSA) and other screening tests can raise suspicions of prostate cancer, but a biopsy is necessary to diagnose the disease.
In a conventional TRUS prostate biopsy, an ultrasound probe containing a spring-loaded needle is inserted into the rectum. The ultrasound guides the physician to various areas of the prostate, and then the needle is inserted into the prostate through the rectal wall to collect tissue samples.
In image-guided targeted fusion biopsy, patients first undergo multiparametric MRI, and a radiologist reviews the results and marks any worrisome areas. These images are fused with real-time ultrasound images taken during the biopsy, enabling the physician to target any concerning areas from the MRI to make sure they’re biopsied.
Dr. Klein supports the use of MRI fusion biopsy primarily for men with prior negative biopsy findings but who still have worrisome PSA levels.
“MRI is a go without question because we know that many of those patients have tumors in the anterior part of the prostate that are missed on transrectal ultrasound, and an MRI can detect them,” he says. “Also, you might have a patient treated with radiation or who has a PSA that’s rising and you wonder if they have recurrent cancer in the prostate. We use MRI in that circumstance to help figure out where to biopsy.”
Advertisement
Some urologists are using MRI to clarify the extent (stage) of a man’s prostate cancer before surgery, while others endorse its use to monitor patients on active surveillance and potentially reduce the number of serial biopsies they require. However, Dr. Klein says evidence supporting MRI’s use in these situations is inconclusive and still evolving.
One potential use for MRI that’s drawing significant interest is as a triage test to determine whether men at risk of prostate cancer require a first biopsy. In a recent study involving 626 men with no biopsy history, researchers concluded that MRI-guided biopsy, compared with TRUS biopsy, resulted in a similar detection rate of clinically significant prostate cancer (defined as Gleason score 3+4 or higher) but with fewer cases of clinically insignificant cancer. Nearly half the men had negative MRI findings and could forgo biopsy, at the risk of missing clinically significant cancer in 4% of cases, the study authors concluded.
Earlier studies found that, compared with TRUS biopsy, MRI fusion biopsy detected a higher percentage of clinically significant prostate cancers and fewer clinically insignificant tumors, and that using multiparametric MRI as a triage test could reduce unnecessary biopsies by a quarter.
However, Dr. Klein notes that not all Gleason 3+4 cancers are clinically significant, which might diminish the advantages of MRI fusion biopsy reported in these studies. Furthermore, the studies involved highly trained radiologists, so it’s unclear how applicable the results might be in a community setting.
He also points to research suggesting that MRI misses many smaller, but potentially life-threatening, prostate cancers that could be detected by TRUS biopsy: “The available data so far suggest that you can’t forgo biopsy in the face of a negative MRI, because MRI misses most high-grade cancers if they are small (less than 0.5cc in diameter),” he says.
“MRI has an established role in ruling out missed high-grade cancer in patients who have had a previous negative biopsy and worrisome PSA. There’s no controversy about that. There is controversy about whether it should be used in all men before an initial biopsy. Whether it’s a substitute for biopsy in men, so far the data don’t support that.”
Available mostly at larger academic medical centers, multiparametric MRI takes about a half-hour to complete. Patients are given an intravenous contrast solution, which allows for visualization of the prostate. The MRI is not recommended for people with chronic kidney disease or who have allergies to the contrast solution. It also may not be suitable if you have problems with confined spaces.
Advertisement
MRI fusion biopsy carries the same risk of complications as standard TRUS biopsy. The biopsy procedure may cause discomfort, and most men have blood in their semen for a few months afterward. You also may have blood in your rectum, stool and urine for several days.
Another potential complication of biopsy is infection. But, with today’s prophylactic antibiotic regimens, the risk of serious infections is very low — 0.5% at Cleveland Clinic, Dr. Klein says.
Dr. Klein recommends asking your physician these questions ahead of time:
This article originally appeared in Cleveland Clinic Men’s Health Advisor.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about our editorial process.
Advertisement
Possible signs include slow urine flow and loss of bladder control — but if this common cancer is caught before it spreads, the prognosis is good

You don’t have to cope in silence with issues like urinary incontinence and sexual dysfunction

Family history and genetics may heighten your risk for prostate cancer

Check-in with your care team, and focus on low-impact exercises and walking for good gains

Sex may be different after prostate cancer treatment, but it can still be enjoyable

Yep! Research shows a possible connection

Not following recommended follow-ups could put you at risk
High-intensity focused ultrasound (HIFU) provides new treatment options

Even small moments of time outdoors can help reduce stress, boost mood and restore a sense of calm

A correct prescription helps your eyes see clearly — but as natural changes occur, you may need stronger or different eyeglasses

Both are medical emergencies, but they are very distinct events with different causes