Changing your wardrobe or environment won’t eliminate eczema, but it can help reduce flares
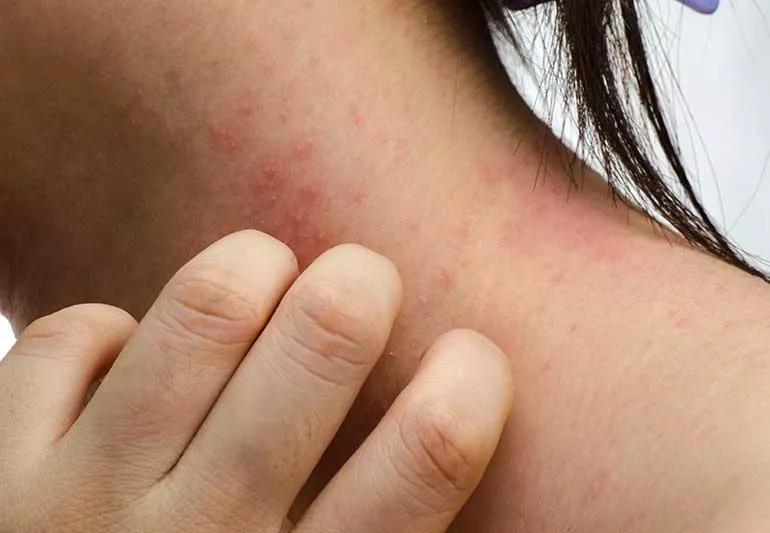
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/1c2637e6-e997-42f4-86e8-bafb27fa0806/Lifestyle-Changes-Atopic-Dermatitis-180934156-770x533-1_jpg)
person scratching neck that has eczema
If you or somebody you love struggles with eczema, you know all too well how much it can impact your daily life. The itching keeps you awake at night and distracted at work, and the angry red rash is a particularly annoying third wheel on date night. It may prevent you from doing activities you love, or even mess with your mood.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
For people whose eczema (the most common form of which is called atopic dermatitis) isn’t well-managed, the impact can truly be all-consuming. But there’s good news: Your skin condition might not be curable, but it can be improved.
We talked with dermatologist Anthony Fernandez, MD, PhD, to learn how lifestyle changes and self-care practices can impact eczema. He shares some strategies for calming your skin and improving your daily lives.
Self-care means different things to different people, but when we’re talking about self-care for eczema management, the definition’s a bit easier to wrap your arms around.
“It’s all about prioritizing your physical and emotional well-being,” Dr. Fernandez says. In this context, that means intentionally taking time out of your day to care of yourself in ways that support your skin’s health.
For people living with eczema, the standard self-care bubble bath is a bad idea. But there are plenty of activities you can do that aren’t just OK for your skin, but good for it. It could be anything from taking a short nap or a walk to devoting five minutes to mindfulness every morning.
Right about now, you might be wondering, “How are naps, walks and mindfulness good for your skin?” The answer might surprise you.
Advertisement
When you’re living with eczema, stress shows up on your skin. That, itself, can be pretty stressful. But that vicious cycle isn’t the only reason you need to attend to your insides as much as your outsides.
Dr. Fernandez explains that people with atopic dermatitis actually perceive itchiness differently than typical people do because their neural pathways are overreactive. Put another way, people living with eczema don’t just have sensitive skin; they also have sensitive nervous systems. When you take care of your mental and emotional well-being, you are treating your skin condition.
But let’s, for a moment, pretend there wasn’t a neuro or psychological component to eczema. It’s still a chronic illness. While some people are lucky enough to outgrow it, many individuals have work to manage the symptoms for the rest of their lives. As is true for most chronic illnesses — the mental and emotional health impact of dealing with eczema can be just as difficult to handle as the physical symptoms. That’s one reason Dr. Fernandez is a strong believer in the importance of mindfulness practices for atopic dermatitis treatment.
“Your eczema probably won’t cause you to develop a mental or emotional health issue, but it can definitely make one worse — and vice versa,” he explains. “Mindfulness can help everybody, but especially people who are experiencing severe symptoms.”
The research backs Dr. Fernandez up. A 2023 study found that adults with eczema who did online mindfulness and self-compassion training for 13 weeks saw a decline in the severity of their symptoms and an overall improvement in their quality of life. When we say, “quality of life,” we mean that they were in less discomfort, reported being in a better state of mind and were able to do their day-to-day tasks more effectively.
Here are a few ways you can work (preferably with the help of a trained mental health professional) to harness the power of the brain-body connection:
Advertisement
Making time for mindfulness is just one lifestyle change that can positively impact your day-to-day symptoms. If you feel less like you’re managing your eczema and more like it’s managing you, Dr. Fernandez suggests considering changes in these five areas:
Atopic dermatitis treatment has come a long way in a short time, so if you haven’t seen a dermatologist recently, Dr. Fernandez suggests making an appointment.
“There are new prescription medications — some pills, some injections and some creams — that are making a big difference for people with eczema,” he says.
Also keep in mind that if you have other allergic conditions like a histamine intolerance, certain kinds of asthma, or mast cell activation syndrome (MCAS), treating those conditions might also improve your skin. Finally, a positive side effect!
Dr. Fernandez has seen it happen far too often: People with severe eczema stop being physically active. Why? Because raising the surface temperature of your skin and sweating can make eczema itch worse.
“The benefits of exercise far outweigh the impact on your skin,” he says. “Instead of giving up on your fitness routine, choose activities that are less likely irritate your eczema and take precautions before, during and after your workout.”
Advertisement
Here are a few recommendations:
Advertisement
There’s no one way people who have eczema should eat because everybody has different triggers. That’s why it’s important to take the time — and it does take time — to figure out if anything you’re eating is making your eczema worse.
One way to do that is to go on an elimination diet. An elimination diet is exactly what it sounds like: An experiment to see what happens if you completely stop eating a certain type of food like gluten, dairy, or red meat for an extended period of time, usually about a month.
It’s important to do elimination diets under medical supervision. Your provider can help you ensure your nutritional needs are being met. They can also they monitor your symptoms and give you advice on what to cut out of your diet and when.
If you find your symptoms improve while you’re on an elimination diet, that’s valuable information that can help you decide what an eczema-friendly diet looks like for you.
People living with eczema have to be very intentional about their personal hygiene. It’s important to keep showers short and temperatures lukewarm to cool. You also need to use bath products that are mild and, where possible, fragrance-free. Gently pat yourself dry with your towel to avoid irritating your skin and slather on the lotion afterward to lock in the moisture. And If you tend to scratch in your sleep, it’s time to embrace the short-nail lifestyle (or sleep with gloves on).
Like any other allergic condition, the severity of your eczema has a lot to do with your surroundings. If your symptoms are giving you trouble, Dr. Fernandez says you may want to evaluate your space. You might need to put an air purifier in your bedroom or switch your cleaning products and laundry detergents. It could be time to swap out your yoga pants for something that’s less restrictive. If your furry friends shed a lot, you may need to vacuum several times a week to keep the dander levels in check. It may even be necessary to limit your time outside— or, if that’s a no-go, take steps to reduce your sun exposure. Small changes like these can make a big difference to your quality of life.
There’s no cure for eczema, but that doesn’t mean you need to resign yourself to a lifetime of itching and discomfort. Instead, look at your lifestyle and see what changes you can make. From managing stress to making different fashion choices, there are lots of ways to reduce the frequency and severity of your flare-ups. Take what works, leave the rest — and when in doubt, talk to your dermatologist.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about our editorial process.
Advertisement
Eczema triggers are different for everyone, but there are some common ways to manage flare-ups, like using a humidifier and fragrance-free creams
There’s not one specific cure-all diet for eczema, but it helps to keep track of what you eat and when you experience symptoms
Both inflammatory conditions have varying triggers and symptoms
Colloidal oatmeal, petroleum jelly and other around-the-home products can help provide needed relief
Your body’s natural response to stress can lead to painful skin irritation
From hyperactive immune response to disordered nerve connections, the itch is real
Hot or cold, your eczema can have flare-ups during multiple times of the year
Keep your showers short and lukewarm, and moisturize promptly after with a cream containing ceramides
These tiny saltwater larvae can get trapped under your swimsuit and trigger an itchy reaction called seabather’s eruption
Searching nature for edible items requires training and knowledge to avoid poisonous plants
Yes, but you can protect yourself with hats, scarves or even hair sunblock