Eczema triggers are different for everyone, but there are some common ways to manage flare-ups, like using a humidifier and fragrance-free creams
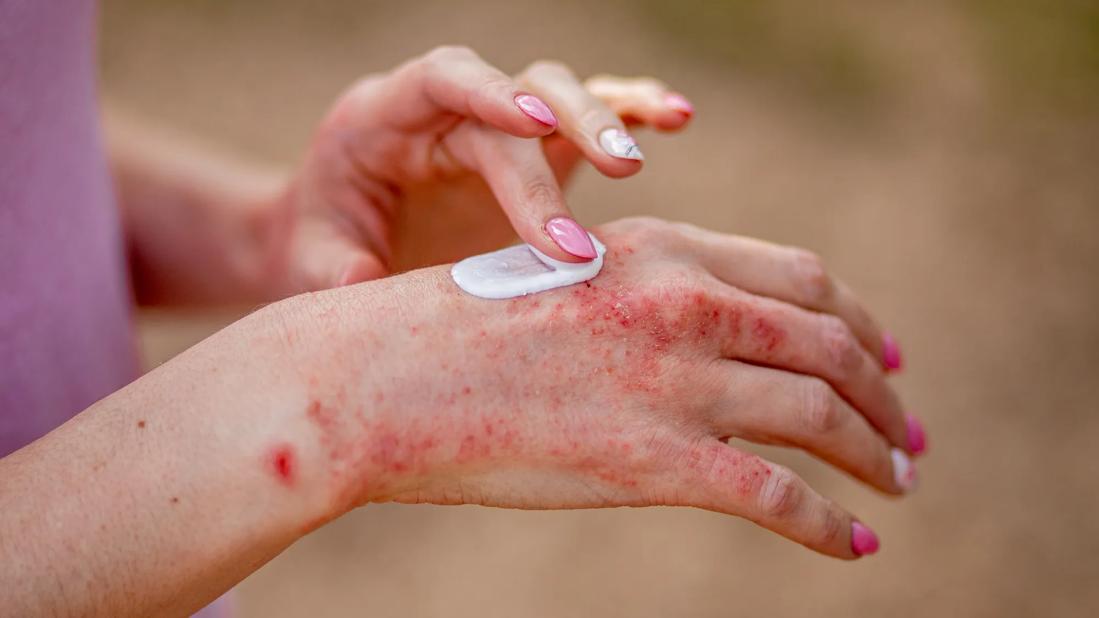
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/d2f16e30-5a3e-43ce-8125-17102733872f/apply-creme-eczema-hands-1387126118)
Person applying lotion to eczema rash on hands
Just when you think the redness, dryness and itchiness have finally gone away — think again. You look down at your knees or elbows, and another eczema flare-up has begun.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Atopic dermatitis is the most common type of eczema, but that doesn’t make it any less tricky to manage. The key is knowing your specific triggers and making changes to avoid future flare-ups.
Family medicine specialist Saadia Hussain, MD, explains why eczema flare-ups happen, how to prevent them and how to find relief.
An eczema flare-up is when one or more areas of your body — commonly your hands, feet, chest or neck — break out in an intense, itchy or dry rash. During an eczema flare, your symptoms suddenly get worse, resulting in:
“Research shows patients with moderate to severe atopic dermatitis experience an average of nine flares per year, with duration ranging from days to weeks depending on severity,” says Dr. Hussain. “For many, flare-ups tend to come back whenever you’re faced with specific irritants, allergies or triggers.”
Eczema can flare up for a variety of reasons, including:
Advertisement
Eczema flare-ups often involve some combination of these. And because an overreactive immune system causes eczema, anything that triggers your immune system to kick in can inevitably cause an eczema flare.
“Using harsh cleaners or solvents, for example, can also cause eczema to flare up because it can take all the fat and oil out of the skin and damage the skin barrier,” explains Dr. Hussain. “As a result, you get inflammation in the affected area, and your symptoms get worse.”
Other common irritants that can cause eczema flare-ups include:
If something irritates your skin, it can also weaken your skin barrier to the point that it makes you more vulnerable to an allergy.
“The irritant not only causes a rash, but it also makes it more likely for you to become allergic to that irritant as well,” he adds. “Since your immune system responds to allergens as a threat, you then experience worse symptoms whenever you come into contact with that specific irritant.”
Video content: This video is available to watch online.
View video online (https://cdnapisec.kaltura.com/p/2207941/sp/220794100/playManifest/entryId/1_5u6y2al6/flavorId/1_5f3sgelj/format/url/protocol/https/a.mp4)
Worried about a future flare? Here are 7 tips for preventing eczema and reducing the severity of your symptoms.
Another key to relieving an eczema flare-up is to take good care of your skin, even after it has gone away or calmed down. It’s important to see a dermatologist to figure out the triggers that are causing your reactions. They can also recommend a variety of over-the-counter and prescription creams or lotions to keep on hand for future flare-ups.
Combined with lifestyle changes, like exercise and healthy eating habits, eczema flare-ups are commonly treated with:
“Our goal is to help restore the skin barrier,” emphasizes Dr. Hussain. “When the skin is inflamed, it’s partly a result of the skin barrier being compromised. When your skin is damaged, it allows things to penetrate a little more and for things to be more irritating. So, it ends up being a vicious cycle.”
“While oral antihistamines are commonly used for itch relief, they have limited effectiveness for atopic dermatitis-related itch and are not recommended as a primary treatment for eczema,” clarifies Dr. Hussain.
Unlike allergic reactions, where histamine drives itching, the itch in atopic dermatitis involves different inflammatory pathways that antihistamines don’t effectively target.
“However, sedating antihistamines may occasionally help with sleep if nighttime itching is disrupting rest because it has a drowsiness side effect,” he adds.
Advertisement
As for preventing an eczema flare-up, Dr. Hussain recommends the following:
Advertisement
Even mild eczema flare-ups over a long period of time can affect your well-being. You’ll want to see a healthcare provider if you experience:
“You might see a dermatologist or an allergist,” says Dr. Hussain. “We all work together to try and figure out if there are any factors you can modify in your lifestyle. And when there isn’t, we can recommend a number of new medications to help treat eczema.”
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about our editorial process.
Advertisement
Address your nighttime itching with moisturizers, topical anti-inflammatories, and changes to your bedtime routine and environment
If you’re dealing with intense itching and red or swollen skin, it might be eczema
There’s not one specific cure-all diet for eczema, but it helps to keep track of what you eat and when you experience symptoms
Both inflammatory conditions have varying triggers and symptoms
Colloidal oatmeal, petroleum jelly and other around-the-home products can help provide needed relief
Your body’s natural response to stress can lead to painful skin irritation
From hyperactive immune response to disordered nerve connections, the itch is real
Hot or cold, your eczema can have flare-ups during multiple times of the year
The virus that causes the so-called ‘stomach flu’ can cling to surfaces for days or even weeks
There isn’t clear evidence that melatonin harms your heart — but finding the cause of sleep issues is key to long-term heart health
Your dollar bills, coins and cards are covered in germs — but they’re very unlikely to make you sick