The field of uterus transplant is advancing

The consequences of infertility can be devastating for women and couples.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Medical experts are working hard to find better solutions to help these women. For a certain type of infertility known as uterine factor infertility, they’re testing an amazing procedure that could give some women with UFI hope for having a baby.
Women with UFI either don’t have a uterus or have one that is not functional. In the past, there has been no way for these women to get pregnant. But in recent years, uterus transplant has emerged as a potential solution for certain women. This involves removing a functioning uterus from one woman who is done having children and implanting it into a woman with UFI so that she can get pregnant and carry a baby.
It might sound futuristic, but it’s really happening.
As part of a clinical trial at Cleveland Clinic, two mothers who received uterus transplants from deceased donors have now given birth to healthy babies.
Maternal-fetal medicine specialist Uma Perni, MD; transplant surgeon Cristiano Quintini, MD, who is the principal investigator on the clinical trial; and transplant surgeon Andreas Tzakis, MD, PhD, who spearheaded bringing uterus transplantation to Cleveland Clinic in 2015, explain how this process works and what the future holds.
A: UFI can be what we call “acquired,” which means that a woman has undergone surgery to remove her uterus. Or it can be congenital, meaning there is an underlying abnormality that caused her to be born without a functioning uterus.
Advertisement
A: The main options would be adoption or surrogacy. Some women are happy with those solutions, but they may not work for everyone because of cultural or religious reasons. Some women also have a deep desire to carry a child on their own.
These are the women who could benefit from a uterus transplant. It’s a recent kind of transplant, and it was a significant innovation in the medical field when we first showed that it can be successful. We place a new uterus into a woman that will allow her to become pregnant and carry a child of her own. It’s the only available treatment for uterine factor infertility.
A: It’s a new procedure, so it’s not widely available. It’s still considered experimental and is only performed as part of a clinical trial.
A: The first step is for us to identify a uterus donor who is of childbearing age and has previously given birth. Meanwhile, the woman who is going to receive the uterus transplant goes through in-vitro fertilization. Her eggs are retrieved and fertilized with sperm in the IVF lab.
The surgery to remove the uterus from the donor is extremely technically challenging. Having a perfectly harvested uterus is critical for the success of the transplant. The uterus is then transplanted into the recipient. That’s also a long and delicate procedure.
During recovery, the recipient takes immunosuppressant medication to prevent her immune system from rejecting the new uterus. If there’s no sign of rejection after several months, infertility specialists complete the embryo transfer and work with the patient to make sure her pregnancy is carried out successfully until the delivery.
A: From what we know so far, these pregnancies are pretty similar to pregnancies in women with their own uterus. We are still very early in this field, though, and we’re still learning what the risks are and how these pregnancies are different. We know there’s an increased risk for preeclampsia in women who have had a uterus transplant. They also must stay on immunosuppressant medications during pregnancy to avoid their body rejecting the uterus. Delivery must happen via C-section, so that’s different as well.
A: The uterus is removed after the woman delivers one or two babies, depending on her preference. This minimizes the amount of time she needs to be on immunosuppressant medications.
A: We want to establish uterus transplantation as a viable treatment option for women with absolute uterine factor infertility. The main challenge remains how to have this procedure become available and affordable for use in a broader population.
Advertisement
Here at Cleveland Clinic, we are pioneering a new aspect of uterus transplantation which involves the use of a uterus from a donor who has died, as opposed to one from a living donor. Recently, a second patient in our clinical trial gave birth after receiving a transplanted uterus from a deceased donor. Both of these births were incredibly joyous occasions for the families and for our entire transplant team. It’s a very exciting time because we’re finally seeing the amazing and life-changing outcomes this transplant can have.
Advertisement
Learn more about our editorial process.
Advertisement

The list includes eating a healthier diet, managing your weight and reducing stress

These consumer-friendly devices can’t assess male fertility nearly as well as a fertility specialist can
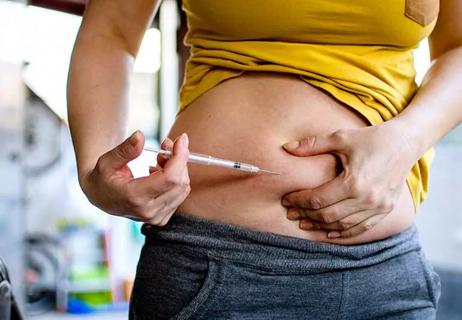
These step-by-step instructions will help you perform self-injections like a pro

Various prescription medications and recreational drugs can have an impact

Here’s a helpful starting point as your infertility journey begins

7 tips to ease the process

Common causes and when to seek help

Some couples should see a doctor sooner than others

The best parenting style balances enforcing rules and showing plenty of love

Tips include cutting back on sugar, focusing on exercise and managing stress

It can be harder to let go when you’ve invested time, energy and emotions — but it might be the healthier choice long term