Nail psoriasis and nail fungus have a lot of similarities, but one is a result of an infection and the other is inflammatory
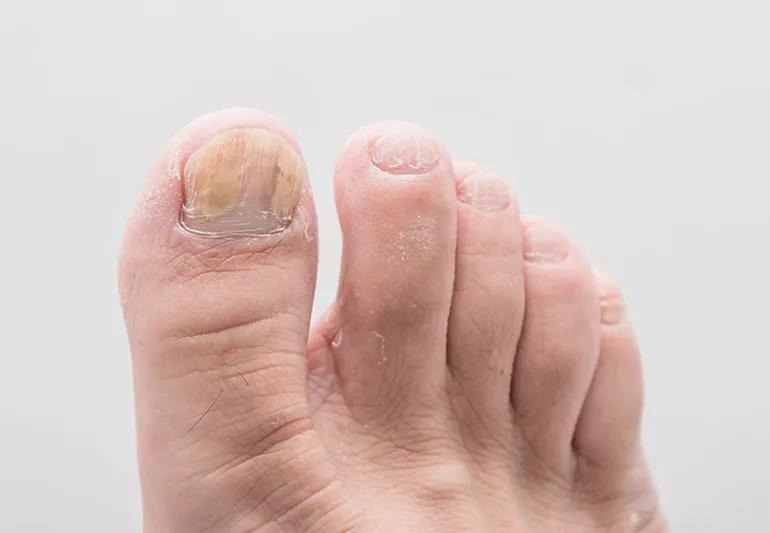
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/466a1450-3879-42eb-9171-57892f2acf44/ToenailPsoriasisVFungus-1069043376-770x533-1_jpg)
Closeup of a foot with yellowed fungus on big toe
Trying to figure out whether you have nail psoriasis or nail fungus may keep you on your toes. There are a lot of similarities between the two — and you can actually have both conditions at the same time — but they’re different from each other and require different types of treatment.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Psoriasis is a skin disorder in which your immune system overreacts, causing inflammation in your skin cells and forming scaly or red patches called plaques. Sometimes, these plaques can be itchy or painful. You can also develop psoriatic arthritis, which causes joint pain and swelling. There’s no cure for psoriasis, but there are ways to alleviate many of its symptoms and provide relief.
Fungal infections are different: They’re curable infections that occur when a bunch of fungi come into contact with your skin and get in between your nail and nail bed. These infections spread quickly and can be contagious. Often, you tend to pick them up in warmer, moist climates. Walking barefoot in wet, high-traffic areas like locker rooms, beside pools or even in garden soil may lead to infection, especially if you have an open wound like a cut or small scrape.
Both nail psoriasis and nail fungus can occur on your hands and feet; however, it’s much more common for nail psoriasis to occur on your fingers rather than your toes.
In virtually every case of nail psoriasis, someone will show other signs of psoriasis somewhere else on their body because it’s a full-body inflammatory disease. “About 5% of people have nail psoriasis alone, meaning they don’t have psoriatic arthritis or skin psoriasis,” says dermatologist Jonathan Braue, MD. “If you see somebody with pretty typical plaque psoriasis, or they have a history of plaque psoriasis, and most of the nail changes they’re having are on the fingernails, then it’s a slam dunk.”
Advertisement
When you have psoriasis, sometimes the top of your nail tends to break down, causing pits, or small divots, to appear along the surface of your nail. “It literally looks like you took a little tack and nailed it down into your nail,” says Dr. Braue. “It’s not a deep pit. It doesn’t go through the entire nail. It just looks like these small little depressions.”
With psoriasis and fungus, sometimes your nail will become detached from your skin and lift on its own, creating a gap underneath your nail. This process is typically painless. “But in psoriasis, you tend to get almost like a lipstick line around that area of white where the plate has lifted,” says Dr. Braue.
Other times, you’ll find red or dark brown splotches on the nail itself. This is often caused by the infiltration of white blood cells in an area that’s been inflamed. “If you see what’s often called an oil spot, that does not happen in toenail fungus,” says Dr. Braue.
While psoriasis is more commonly found on fingers, fungal infections typically occur on your toenails, and most often on a single toe unless it’s left untreated and spreads. “If you see a single toenail involved, it’s much more likely it’s a fungal infection or trauma-related, not psoriasis,” says Dr. Braue. “Fungus will affect your nails differently based on the part of the nail that’s infected.”
This highly contagious fungal infection is a form of ringworm that causes an itchy, stinging or burning rash on your skin. Sometimes, the skin under your nails can become cracked, causing open wounds that may then become further infected, causing toenail fungus. “If you see someone who just has rip-roaring athlete’s foot and they have toenail changes, it’s probably a fungus,” says Dr. Braue.
As with psoriasis, nails affected by fungus can become detached, causing severe discoloration in the nail. Often, you may find yellow or white streaks along the entirety of the nail that’s become detached, or in small lines. “Because the plate is lifted, it’s not uncommon to get some secondary bacterial infections in there as well,” says Dr. Braue.
Sometimes, your nail and the skin underneath it will thicken as a result of a fungal infection. This nail growth is not normal and will often be brittle and crack. “You can get pain associated with it especially if it thickens so much,” says Dr. Braue. “It can be painful in certain shoes. It can be painful to trim.”
Since the root causes of nail psoriasis and nail fungus are different, the ways they’re both treated are also different.
“For nail fungus, you’re trying to treat an infection, so you’re using antifungals, topically or orally,” says Dr. Braue. “Psoriasis is inflammatory, so you’re trying to quell the immune response and calm that inflammation. In those cases, you’re using things like steroids.”
Advertisement
If you’re noticing signs of nail psoriasis or nail fungus, you should see your healthcare provider, who can accurately diagnose exactly what it is you’re dealing with. They’ll then prescribe ointments or medication — and in some cases, a combination of both. Treatments may last anywhere from a couple of months to a full year, as you need to give your body time to rid itself of the infection (in the case of fungus) or to regrow healthy nails. As a healthy nail grows over time, it’s important to trim the unhealthy or infected part of the nail off. If you’re experiencing pain, consider wearing more comfortable, loose-fitting shoes until you’re fully healed.
Occasionally, you can get steroid injections — though, these tend to hurt when given in such a sensitive spot like your feet — to speed up the process, or you may be able to seek out cosmetic options such as laser or surgical removal.
“Most people are going to improve within six weeks or so with skin psoriasis, but it may take several months to notice improvements with purely nail psoriasis,” says Dr. Braue. “It takes 12 to 18 months to regrow a toenail. If you remove the toenail completely, you’re going to be waiting a year, year-and-a-half.”
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about our editorial process.
Advertisement
Plaque psoriasis builds over time, while GPP can appear suddenly with symptoms that may require urgent care
Signs like fever, breathing problems and muscle weakness, along with red patches and pus-filled bumps, mean it’s time for emergency treatment
Understanding what sets off this serious skin condition can help you recognize when you need urgent care
Moisturize often, take oatmeal baths, use Epsom salts and follow a healthy diet to help reduce your symptoms
The common skin condition isn’t contagious, but it can pop up anywhere on your body during a flare
A well-balanced diet with anti-inflammatory foods can help reduce flare-ups and severity of psoriasis symptoms
Caused by inflammation, psoriasis itch can be managed with a variety of treatments, like moisturizing and taking cooler and shorter showers
Stress, infections, skin injuries and environmental factors can trigger an onset of psoriasis symptoms
The virus that causes the so-called ‘stomach flu’ can cling to surfaces for days or even weeks
There isn’t clear evidence that melatonin harms your heart — but finding the cause of sleep issues is key to long-term heart health
Your dollar bills, coins and cards are covered in germs — but they’re very unlikely to make you sick