The biggest concern is that they could rupture
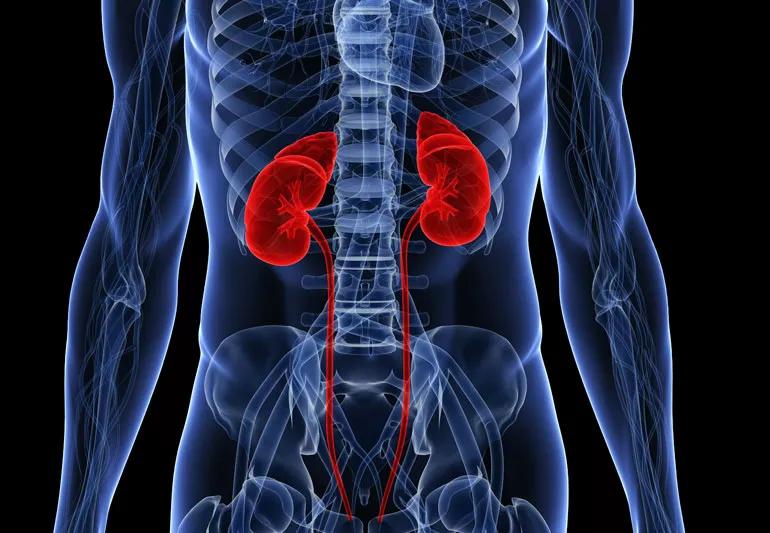
If you have a renal artery aneurysm — or a bulging, weakened area in the wall of an artery to your kidney — it could go unnoticed for some time.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Renal artery aneurysms (RAAs) are rare (they occur in approximately 0.1% of the general population), but they typically don’t cause symptoms and are often found during medical imaging for unrelated reasons, says vascular surgeon Francis Caputo, MD.
These aneurysms can sometimes lead to high blood pressure (hypertension) or compromised kidney function. But the biggest concern is the risk that they could rupture – particularly with increased size of the aneurysm. Ruptured RAAs are associated with significant morbidity and mortality, says vascular surgeon Jarrad Rowse, MD.
One explanation for RAA is atherosclerosis, or hardening of the arteries, which causes degeneration of the arterial wall. RAAs are also related to fibromuscular dysplasia, a disease that causes arteries to narrow, says vascular surgeon Sean Lyden, MD. Most people with this condition are 40 to 60 years old, and many are women.
According to one study, risk factors of RAA rupture include pregnancy, polyarteritis nodosa or large aneurysm size. Patients with these risk factors should be considered for a planned (elective) surgery before it becomes an emergency.
According to a study which looked at people with renal artery aneurysms that spontaneously ruptured, a few reasons you can develop one include:
Advertisement
If you have difficult-to-control hypertension, bloody urine, or pain in your upper abdomen, back or side (also known as flank pain), your doctor may perform a computed tomography angiography (CTA) scan to determine if you have a RAA. This scan gives the best view of the aneurysm and arteries branching off of it in order to determine how best to repair the aneurysm, Dr. Caputo says.
Repair of RAAs is recommended for patients who have medically refractory hypertension, renal artery stenosis (narrowing of the artery), or symptoms (bloody urine or upper abdomen, back or side pain), regardless of the size of the aneurysm.
Repair should be considered for patients with RAAs that aren’t causing symptoms if they are:
RAAs can be repaired either with endovascular repair or open surgery. Endovascular repair is a minimally invasive procedure that’s done inside your blood vessels. This has advantages over open surgery, as there’s a lower risk of major adverse effects and shorter recovery time. However, not every RAA can be treated this way, Dr. Rowse says.
While 98% of aneurysms occur outside of the kidney, if they involve more than one branch, open surgery is the gold standard for repair. The goal is to preserve as many branches off of the aneurysm as possible.
Whether your doctor recommends an open or endovascular repair, there is no difference in the lessening of your kidney function.
If your RAA can be treated with endovascular repair, you can expect to stay overnight in the hospital and return to normal activities in about a week. If an open operation is recommended, you can expect to be in the hospital for three to five days and back to regular activities within a month.
When looking to get a RAA repair, it’s important to go to a multispecialty hospital, Dr. Lyden stresses. Many of these repairs are performed with both urology and vascular surgeons to provide the best outcomes. Sometimes, repair is more complex and the kidney is removed so the aneurysm can be repaired. The kidney is then re-implanted, much like a kidney transplant, Dr. Lyden explains. This allows doctors to preserve the kidney during very complex procedures.
Advertisement
Learn more about our editorial process.
Advertisement

Tracking your weight, swelling, blood pressure and more may help you — and your provider — figure out what’s driving secondary FSGS

Regular visits with your nephrologist, at-home testing and symptom tracking ensure you’re doing all you can to preserve kidney function

Testing can both reveal the likelihood that you’ll pass on complement 3 glomerulopathy and identify possible treatments

It’s a way to further glomerular disease research and expand your treatment options

Expect some new prescriptions, as well as recommendations to avoid other medications
You may not notice any symptoms of kidney disease until later stages

When you have kidney disease, low-sodium and nutrient-rich foods are the dietary ‘golden rules’

The best predictors of kidney cancer’s return are cancer type, stage and grade after surgery

Wearing a scarf, adjusting your outdoor activities and following your asthma treatment plan can help limit breathing problems

Your diet in the weeks, days and hours ahead of your race can power you to the finish line

When someone guilt trips you, they’re using emotionally manipulative behavior to try to get you to act a certain way