Ignoring the warning signs could put you at risk for serious health issues

How often do you think about the quality of your breathing while you sleep? Probably never. But it might be time to give it some thought — particularly if you wake up feeling less than rejuvenated.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Sleep apnea is a “grossly under-recognized” breathing condition that increases the risk of heart attack, stroke and other serious health consequences. It’s estimated that 85% to 90% of people with sleep apnea don’t know that they have it.
Meanwhile, research shows that the number of people with diagnosed sleep apnea continues to grow, affecting:
That’s a worrisome trend that can keep you up at night. To help you sleep easier, let’s learn more about the condition and talk about solutions with sleep medicine specialist Nancy Foldvary-Schaefer, DO, MS.
In the simplest of explanations, you stop breathing.
Obstructive sleep apnea (the most common type of sleep apnea) occurs when your upper airway narrows or becomes blocked at the back of your throat, which reduces or even stops airflow to your lungs.
Thankfully, your body’s on-duty survival reflex is trained to kick in when your oxygen dwindles. That save-the-day response results in you waking up just enough to resume breathing, explains Dr. Foldvary-Schaefer.
People with moderate to severe sleep apnea may have 15 or more of these episodes per hour. Briefly waking up is better than not breathing, of course … but it’s also not great for restful and restorative sleep.
Advertisement
If your sleep apnea is severe, you might wake up at night gasping for air and feeling like you’re choking. (If you share a bed with someone, they may tell you that it’s pretty scary watching you sleep.)
Snoring is often a telltale sign of sleep apnea. “Not all snorers have sleep apnea, but snoring is usually the first noticeable symptom,” shares Dr. Foldvary-Schaefer.
But signs of sleep apnea aren’t just evident during sleep. Fatigue, declining performance at work or school and mood changes are all associated with sleep apnea. Morning headaches are common, too. You also may experience problems with sex.
Women often have more subtle symptoms, typically involving fatigue and often attributed to depression. “It can take women up to a decade longer than men to receive a diagnosis of sleep apnea,” says Dr. Foldvary-Schaefer.
Anyone at any age can experience sleep apnea, but some groups or circumstances make the condition more likely. The list includes:
Drinking alcohol and sleeping on your back also can aggravate the condition, notes Dr. Foldvary-Schaefer.
Ignoring sleep apnea can come with consequences.
“Untreated apnea increases your risk of stroke, heart attack and high blood pressure,” states Dr. Foldvary-Schaefer. “If you have atrial fibrillation, sleep apnea doubles your odds of having a recurrence. If you have heart failure, it increases your risk of hospital admission.”
Sleep apnea can leave you fatigued and irritable, too, raising your risk of motor vehicle crashes, work-related injuries and accidents. Children with sleep apnea may have difficulty focusing on school.
Worldwide, people with obstructive apnea rate their quality of life worse in every measurable way.
Sleep apnea is very treatable once it’s identified. That’s where you come in.
“It’s easy to forget to bring up sleep apnea symptoms at your annual checkup, but it’s best to tell your doctor about them,” advises Dr. Foldvary-Schaefer. “Otherwise, sleep apnea can be missed for many, many years.”
To see if you have sleep apnea, your healthcare provider will likely take a sleep history and order a sleep study. In some cases, you may be referred to a sleep medicine specialist or sleep center.
Advertisement
The gold standard for sleep apnea treatment is positive airway pressure (PAP). This method uses specialized devices to increase air pressure in your airway, which keeps it open so you can breathe.
Odds are you’ve heard of a continuous positive airway pressure (CPAP) machine, one of many devices used for treatment.
“But there are multiple forms of PAP therapy and a wide range of masks,” clarifies Dr. Foldvary-Schaefer. “Patients with difficulty tolerating the constant flow of air pressure often prefer auto- or bi-level PAP therapy and need help with mask options.”
Other treatment routes include:
Most people spend one-third of their day sleeping. Don’t underestimate how vital that time is for your overall well-being.
“Sleep is as important to good health as diet and exercise,” says Dr. Foldvary-Schaefer. “We need sleep to restore every cell in our bodies. If we neglect it, some aspect of our health will suffer.”
Advertisement
Learn more about our editorial process.
Advertisement

Sleep apnea is associated with sudden cardiac death and other complications that increase your risk of mortality

Here’s what to know from a sleep medicine specialist
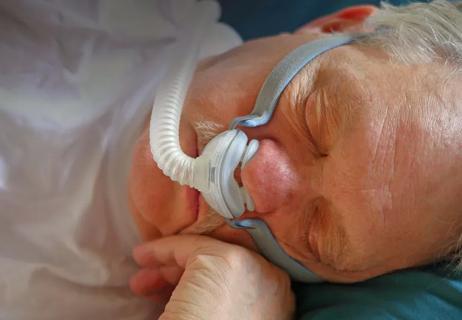
Sleeping disorder may increase danger of cardiac event

Manage your sleep apnea and keep your diabetes in check

If you’re putting off going to bed to have some time for yourself, you’re not doing your well-being any favors

Pain, light exposure and anxiety are just a few factors that could be waking you up in the middle of the night
Try setting a regular sleep schedule, creating a comfortable sleep environment and reducing stress

If allergies have you coughing and sniffling all night, try showering before bed, keeping the windows closed and propping your head up

If you’re feeling short of breath, sleep can be tough — propping yourself up or sleeping on your side may help

If you fear the unknown or find yourself needing reassurance often, you may identify with this attachment style

If you’re looking to boost your gut health, it’s better to get fiber from whole foods