Sneezing, coughing and clear mucus shouldn’t be ignored
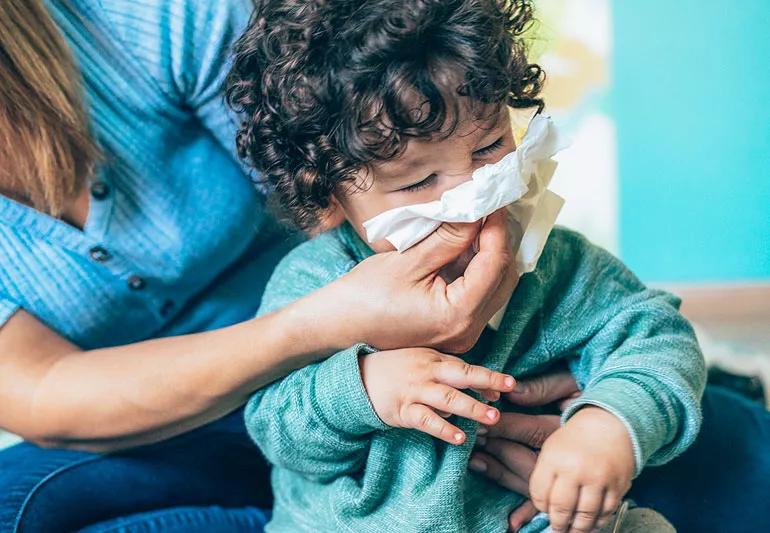
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/18812f79-6476-4c43-a03e-b91ae9869119/toddler-Mom-Wipes-Nose-1358823379-770x533-1_jpg)
While sitting on floor, parent wipes toddler's nose with tissue.
Irritants like pollen, ragweed and mold can spell misery for people with allergies — and that includes kids. It may be easy to recognize your own allergy symptoms, but it can be tough for even the most seasoned caregiver to tell the difference between allergies and a cold or other infection.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
But spotting allergy signs, and treating them appropriately, is important says allergist Sandra Hong, MD. “When allergies aren’t controlled, they can cause asthma flare-ups, with coughing, wheezing and difficulty breathing. And allergy flare-ups can make it difficult for children to concentrate in school, especially in classrooms where they may be exposed to environmental allergens, like pollen and mold.”
Dr. Hong shares how to spot allergy symptoms in kids, and what to do if you suspect your child is dealing with seasonal and environmental allergies.
Children who have allergies can feel quite miserable, and their symptoms can keep them from being able to do their best in school or while participating in extracurricular activities.
Kids with environmental allergies tend to exhibit many of the same symptoms as adults. That includes things like:
But maybe your child can’t articulate exactly what they’re feeling. That’s OK, and very common.
Some allergy symptoms are things you can spot without your child having to explain their symptoms to you. Dr. Hong says one telltale sign of allergies is a child rubbing their face. A lot.
Advertisement
“Rubbing their eyes and rubbing their nose is pretty common,” she says. “Some kids will get a little tiny line, right on their nose, and it’s because they actually push up on the fleshy part of their nose so often. So you’ll see a little crease there just from rubbing their nose so much.”
As soon as you notice that your child is having trouble with allergies, you’re best off managing them right away, before they start to exacerbate asthma symptoms, or gum up the works to the point of a sinus infection or ear infection.
If their symptoms get out of hand, contact their healthcare provider, like their pediatrician.
Dr. Hong suggests these strategies to manage your kid’s allergies:
Avoidance is the best treatment for allergies, but it’s tricky when the trigger wafts in the air. Luckily, you can lower your child’s exposure without locking them in a bubble all allergy season long.
If things like grass or weed pollen seem to be the trouble, save the outdoor activities for evenings when possible. That’s because those allergens tend to peak in the morning. And have your child wear sunglasses when they’re playing outside to prevent itchy, irritated eyes.
After outdoor fun, make sure your child showers and has their hair washed before going to bed.
Inside, you can create a pollen-free zone in your child’s bedroom. Be sure to keep the windows shut to keep the allergens out. Another thing you can do is use a HEPA filter for your central air conditioner unit or a personal air filter in your child’s room to reduce indoor pollen.
Over-the-counter treatments such as saline sprays, nasal steroid sprays and antihistamines can work for children, but Dr. Hong recommends that parents talk to their pediatrician about the different medications and proper dosing.
It’s also important to be on the lookout for how allergy medications make your child feel.
“Some liquids or pills can cause sleepiness, so you want to make sure that you either dose them at night or choose one that’s a little bit better for your child during the day so they’re not drowsy,” Dr. Hong advises.
Antihistamines and nasal sprays are best given throughout the allergy season, even if your child feels better.
Some over-the-counter medications manage allergy symptoms well for most children. Some long-acting, antihistamines come in children’s formulations — like liquids and chewables. And they typically don’t cause drowsiness. That includes medications like:
Advertisement
Dr. Hong notes that antihistamines work well for sneezing and itching but may not adequately address symptoms like stuffiness and drainage.
Some kids may benefit, too, from antihistamine eye drops for itchy eyes. It’s best to avoid eye drops that are marketed as redness reducers. Those drops may actually make dry eyes worse over time.
If your child is dealing with sneezing, itching, stuffiness and drainage from allergies, Dr. Hong says a nasal spray may work well. That includes medications like:
If you choose a nasal spray, know that proper application is important and could make all the difference in how well the medicine works. It can also decrease nosebleeds, which can be a possible side effect.
When giving your child nasal spray, try this technique: Insert the applicator in the right nostril, not too far. Aim out toward the right eye and spray. Repeat on the left side.
Nasal decongestants like Sudafed® and Zyrtec-D® are popular for adults.
But Dr. Hong advises talking with your child’s healthcare provider before giving decongestants to kids. That’s because they can cause a number of side effects and serious complications. So, you’re probably better off trying other methods for symptom relief first.
Advertisement
If avoiding allergens and trying allergy medications don’t do the trick, it may be time to ask your pediatrician or allergist about allergy immunotherapy.
Allergy immunotherapy is a way of desensitizing your child’s allergy response. Depending on certain conditions, like your child’s specific allergens, age and more, your provider may recommend injections (“allergy shots”) or dissolvable immunotherapy tablets.
Injections are given weekly over the course of months. That’s followed by maintenance injections for several years. Allergy immunotherapy can help reduce the severity of your child’s allergy symptoms.
Sublingual (under-the-tongue) tablets can be taken daily before your child’s allergy season and throughout. They’re effective like shots and can be taken at home for certain allergens.
If your child is having allergy symptoms long-term, or if allergies are affecting their school attendance or focus in class, Dr. Hong advises seeking medical treatment. Talk with a children’s healthcare provider or immunologist to get your child the relief they need.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about our editorial process.
Advertisement
The right choice for you depends on your symptoms, but options like nasal sprays and antihistamines can offer relief
When your allergies flare up depends on your location, immune health, personal triggers and more
Washing your sheets, rinsing your sinuses and running an air purifier are simple tricks for all-natural allergy relief
A variety of factors, including changes to your body as you age, may lead to new allergies later in life
Most antihistamines, like Zyrtec, are OK, but avoid decongestants for at least the first trimester
You can now get lifesaving epinephrine in a nasal spray and prefilled syringes
Drowsiness is a side effect of inflammation, disrupted sleep and, sometimes, your allergy medicine
If you’re sensitive to aspirin or other salicylates, limiting exposure is the best remedy
These tiny saltwater larvae can get trapped under your swimsuit and trigger an itchy reaction called seabather’s eruption
Searching nature for edible items requires training and knowledge to avoid poisonous plants
Yes, but you can protect yourself with hats, scarves or even hair sunblock