Several conditions, like vitiligo and fungal infection, can cause a loss of pigmentation, leading to white spots or patches on your skin
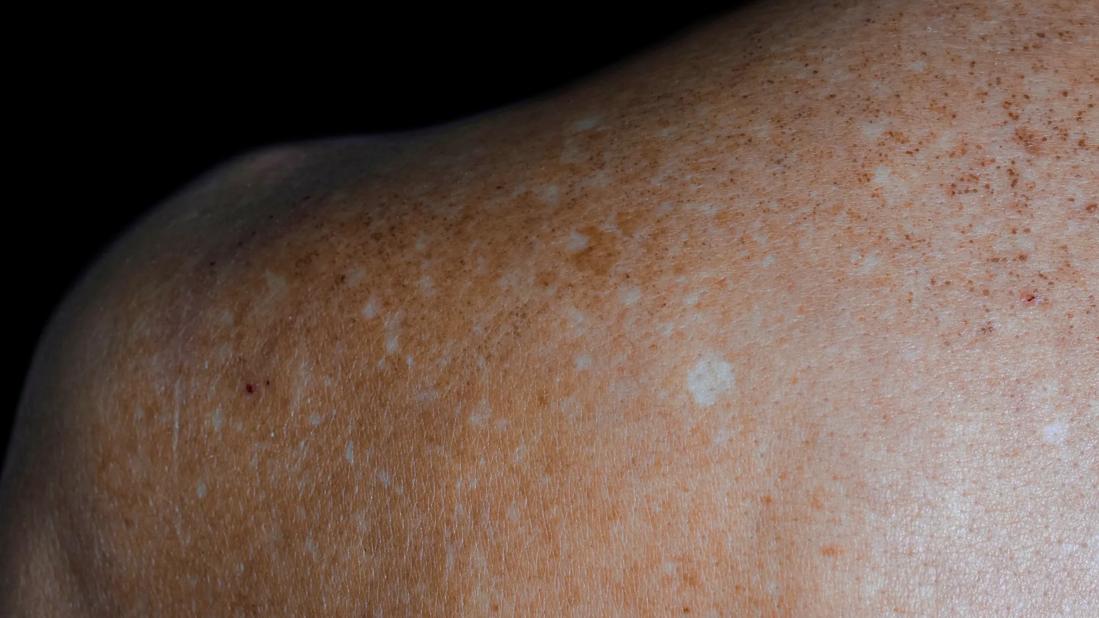
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/2296e401-b928-47cf-8b74-a9de85da1880/sun-spots-skin-1449529284)
Person's bare shoulder with white spots and freckles
White spots, white patches or discoloration on your skin can happen for a variety of reasons — but are they ever a cause for concern? Depending on their appearance and where these pigment changes pop up, they could be signs of different skin conditions that may or may not need treatment.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Dermatology resident Angela Wei, MD, shares details behind some of these white spots and when you should get them checked out.
White spots or patches are areas of your skin that, for some reason, are missing their pigment. To understand how this happens, it helps to know that one inch of your skin has about 19 million skin cells and 60,000 melanocytes. Melanocytes are the cells that make melanin, or skin pigment.
The amount of melanin you have determines the color or pigmentation of your skin. So, when there’s a lack of pigment or a loss of melanocytes, white spots or patches can show up. These affected areas are very different from acne or sunburn.
Here are some of the most common conditions associated with white spots or patches.
Idiopathic guttate hypomelanosis is a benign condition that looks like little raindrops or white dots on your skin. These spots can appear anywhere on your body that’s been exposed to the sun, but you tend to see them more on your:
“While we don’t know exactly why it happens, it’s thought to be related to sun exposure over time,” says Dr. Wei. “Since it could be a marker of sun damage, sun protection is very important.”
Advertisement
Tinea versicolor is a common fungal skin infection that often shows up in white patches. It can also appear as dark or pink spots. It’s not harmful or contagious, but it can be itchy. Caused by an overproduction of yeast, you’ll often find these white patches on your:
The yeast removes pigment from skin, and that lack of pigment is what causes the white patches. If you have darker skin, these patches may show up as a faint, light brown color.
“The yeast organisms thrive in warm and humid environments, so this condition can become more pronounced and spread if you sweat excessively,” notes Dr. Wei. “Typically, this condition can be treated with antifungal body wash, cream or oral medication. It could take months for pigmentation to return.”
Vitiligo is a chronic autoimmune condition that happens when inflammatory cells target and kill the melanocytes that create pigment in your skin. It appears as large, smooth patches of white or lighter skin and can grow over time if left untreated.
It’s not painful, but lighter areas of your skin can be more vulnerable to severe sunburn because they don’t contain pigment.
Vitiligo typically starts around your:
“Treatment usually starts with topical steroids, but as it’s a chronic condition and we can’t use topical steroids forever, there are often other treatments we use longer term,” clarifies Dr. Wei.
Most often, treatment relies on nonsteroidal topical creams like tacrolimus. In some cases, light treatments can be used to target and activate pigmented cells.
If treatment doesn’t work, you might experience vitiligo all over your body. If you prefer a more uniform skin tone, doctors may suggest removing pigment completely with the help of oral medications or skin therapy treatments.
Pityriasis alba causes raised, round or oval itchy patches of lighter skin that mostly affect children. The lightening of pigment is thought to occur because of inflammation associated with eczema. When your surrounding skin gets darker as a result of sun exposure, the areas affected by eczema can also appear whiter and more noticeable.
“This condition causes lighter, wider patches on the cheeks of kids who often have eczema,” says Dr. Wei. “People with eczema have a very active immune response. Their skin is very sensitive and very itchy.”
Often, this condition will improve on its own over time. To help manage the inflammation associated with pityriasis alba and speed up the recovery process, healthcare providers will recommend topical steroids or nonsteroidal topical creams.
Advertisement
“Just like eczema, the most important thing with this condition is to keep your skin moisturized to prevent your skin from drying up and becoming itchy,” says Dr. Wei.
Milia, or milk spots, are small, raised, white cysts that develop just under the surface of your skin. Although harmless and painless, they’re commonly confused with whiteheads or pimples. They most often pop up on your:
Dead skin cells that get trapped and then harden under the surface of your skin cause these white cysts. Because they’re not harmful, they don’t require treatment. But if their appearance concerns you, a dermatologist can recommend over-the-counter and medicated creams or surgical treatments to help remove them.
There are other reasons why you might have white patches or spots on your skin. Many of these are rare (and some potentially dangerous), including:
Advertisement
“While these conditions are typically rare, it’s important to see your doctor or dermatologist to have new or changing spots on your skin evaluated to make sure there is nothing more serious going on,” advises Dr. Wei.
While white spots on your skin aren’t typically dangerous, if you notice any changes in your skin tone, consider making an appointment with a dermatologist just to be safe. Additionally, pay close attention to any changes in moles, birthmarks, pimples or bruises on your body. Annual skin cancer screenings are also recommended for anyone with a history of:
And if you ever experience other symptoms, like painful, bleeding or itchy skin, it’s good to get that looked at, too.
“Areas without pigment cells are more vulnerable to the development of skin cancers,” states Dr. Wei, “So, I stress to everyone, particularly those with pigmentary problems, to be hyper-vigilant about any changes to their skin and to prioritize sun protection.”
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about our editorial process.
Advertisement
This cooling gel can help soothe sunburned skin, but it can’t cure the burn
You know it’s not good if you’ve been holding onto it for more than three years or if it’s changed in color, consistency or smell
Look for a UPF rating of 50+ for optimal protection against UV rays
A sunburn will leave you itchy and red, while sun poisoning can feel like an allergic reaction
A cool shower, aloe vera gel, anti-itch treatments and cool compresses can provide fast sunburn relief
SPF stands for ‘sun protection factor’ — it’s a measure of how much protection you’re getting before a sunburn is possible
This ‘poisoning’ is actually a severe sunburn that seems similar to an allergic reaction
When outside, protect your skin from damaging UV rays with a fresh layer of sunscreen at least once every two hours
Sweat less by using antiperspirant, wearing breathable fabrics and talking to a provider about medical options
Following a few simple gym rules can help you feel confident, avoid awkward moments and stay safe
If your kidneys are healthy, an uptick in protein is usually fine, but going overboard can be risky