What you need to know about prosthetic joint infection after surgery
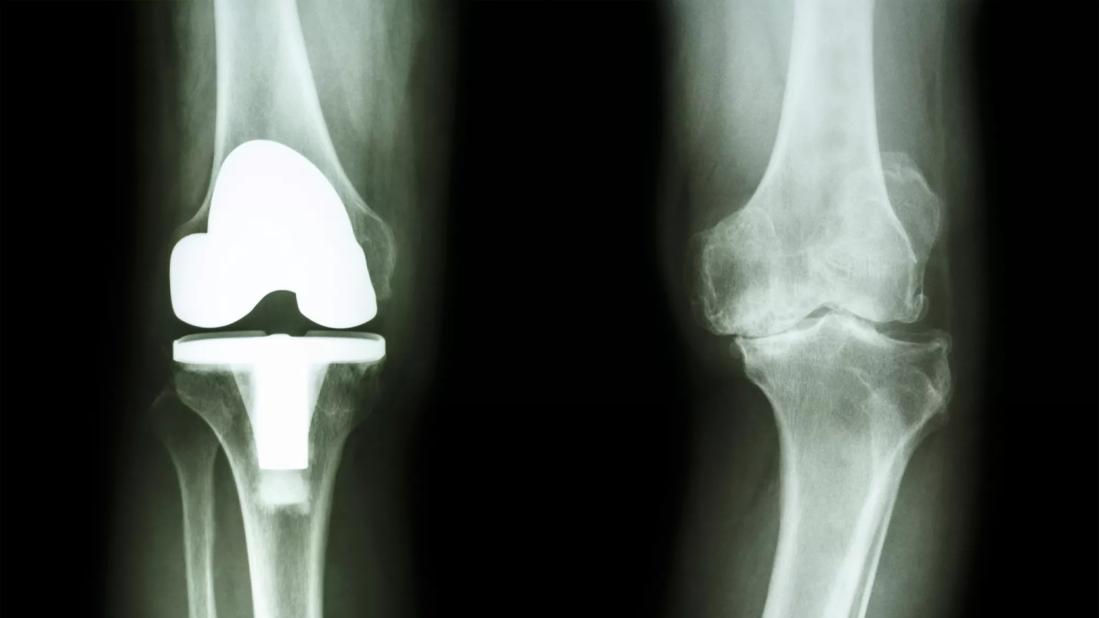
According to orthopaedic surgeon Anokha Padubidri, MD, two of the most common questions asked at her outpatient clinic is, “Should I have joint replacement surgery done?” and “How old is too old for joint replacement?”
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“There’s no age limit on who can safely undergo joint replacement surgery,” she says. But for some people, the risks that may follow surgery can outweigh the benefits.
“One of the more serious risks is a complication of total joint arthroplasty called prosthetic joint infection or periprosthetic infection,” Dr. Padubidri says. “It’s important for patients to know risks like PJI before considering surgery. There are also preventative steps they’ll need to consider to prevent this often debilitating and expensive complication if they do opt for it,” she says.
Prosthetic joint infection happens when bacteria around a replaced joint gets infected after surgery. It causes swelling, pain and other more severe problems that if not prevented may require a long-term, painful and costly treatment plan.
“This infection compromises both function and pain relief after surgery,” Dr. Padubidri says. “But it can’t be understated that patients can play a huge role in their own prevention of it.”
She points out that not only are these infections burdensome for patients, but also for hospital systems. PJI occurs in 0.5% to 2.5% of joint replacements in the United States alone. The cost to treat it in the U.S. is expected to reach more than $1.6 billion in 2021.
Advertisement
The cheapest and best way to avoid complications from prosthetic joint infection is to prevent it. Prevention is controlled both by the surgeon and patient factors.
If you’re considering joint replacement here are four ways to help reduce your risk of infection:
This is a bacteria that commonly causes joint infections. Not all hospital systems perform this simple test. Those patients who are carriers are given an antibiotic ointment to apply to their nose and special medicated wipes to use before surgery. This can decolonize the patient and lessen their risk of infection.
Patients who use nicotine in any form are at a greater risk of having wound healing problems. Wound healing issues can lead to prosthetic joint infection but people who quit using nicotine prior to surgery can decrease their infection risk.
Another important factor in minimizing infection risk is adequate control of blood sugar for those patients who have diabetes. Diabetes control is often checked with a blood test called hemoglobin A1c, or HbA1c. People whose HbA1c is above seven are at greater risk for prosthetic joint infection. Surgery should be delayed until better diabetes is under better control.
Finally and most importantly, maintaining a healthy weight can dramatically reduce the risk of prosthetic joint infection. Ideally, a body mass index less than 35 to 40 kg/m2 can be achieved prior to surgery. If a patient’s BMI is over 40 their risk of complications may be up to seven times higher.
“In today’s healthcare environment patients need to take ownership of their health,” Dr. Padubidri emphasizes.
“In order to prepare yourself for surgery and minimize your risks, it’s best to consider losing weight and aggressively managing any medical issues, especially diabetes. You’ll also want to stop smoking. Be sure to ask your surgeon what steps the hospital takes to manage the risk of infection.”
Advertisement
Learn more about our editorial process.
Advertisement
Some creakiness is typical after rest, but longer-lasting stiffness may be other issues

Barometric pressure can play a role in joint pain, but that doesn’t mean you have to live with it
Several options to help get you moving

Even one less pound helps preserve hips and knees

Getting the facts straight about osteoarthritis

These creams that you apply to your skin can actually help reduce localized pain, swelling and inflammation

While an ultrasound shows your muscles and tendons, an MRI also shows your joint cartilage, bones and heart chambers

Arthritic knees can benefit from bridging, mini squats, balancing exercises and other stretches

Wearing a scarf, adjusting your outdoor activities and following your asthma treatment plan can help limit breathing problems

Your diet in the weeks, days and hours ahead of your race can power you to the finish line

When someone guilt trips you, they’re using emotionally manipulative behavior to try to get you to act a certain way