Advertisement
When at-home treatment is not enough
If you live with arthritis pain, you’re probably familiar with at-home fixes such as ice and heat packs, stretching routines, pain relievers and simply putting your feet up and taking a break.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
All of these can be helpful — but sometimes they’re just not enough.
Rheumatologist Scott Burg, DO, talks about four cases that need further attention from your primary care doctor or rheumatologist.
If you have a minor flare-up of aches and pains, conservative home therapy often works well. This can include ice or heat as needed, over-the-counter pain relievers (as long as you don’t have any dangerous drug interactions — see below) and periods of rest.
The Arthritis Foundation suggests trying acupuncture, massage therapy, tai chi and yoga as a few options to help relieve your arthritis pain.
If your pain doesn’t respond after a week, it’s worth a trip to the doctor’s office for a thorough checkup and diagnosis.
“Rest often goes a long way toward relief,” says Dr. Burg “When this conservative approach fails, it may be a sign of a deeper problem.”
You probably know your baseline of pain pretty well. You know you may have 15 to 20 minutes of stiffness in the morning, for example. But if you suddenly have a red-hot, swollen knee, wrist or other isolated joint — especially if that’s not typical for you — it may be cause for concern.
“We call this a ‘joint out of phase’ because it differs from your usual aches and pains,” explains Dr. Burg. “Excessive redness and swelling raise red flags because they often are signs of infection.”
Infections can be serious business, especially if you have conditions like rheumatoid arthritis or lupus and are taking medications that weaken your immune system. If this happens to you, especially if you have symptoms such as a fever, see your doctor. It’s critical that any infection is identified and treated properly, so it doesn’t spread.
Rest pain is another sign your arthritis may need more aggressive treatment. Rest often goes a long way toward relief. But when this conservative approach fails, you may have a deeper problem.
Advertisement
“If your pain doesn’t get better with rest, see a doctor,” says Dr. Burg. “It may be time to consider medical treatment, including the possibility of surgery for severe back, hip or knee pain. In fact, most orthopedic surgeons won’t operate on a person unless they have rest pain; that’s how much of a red flag it is.”
Many people deal with some type of arthritis along with other conditions, like GERD or stomach ulcers. But if this is your case, be especially careful with self-medication.
Here’s why: Many times, drugs to treat pain and inflammation conflict with drugs to treat other conditions. For example, long-term use of non-steroidal antiinflammatories (NSAIDs) can make digestive issues like ulcers worse, especially if you’re taking a proton pump inhibitor for heartburn or GERD. Likewise, many pain medications raise your risk levels if you have heart disease or be dangerous if you have kidney disease.
If you take multiple drugs for multiple conditions, check with a doctor before treating your arthritis on your own, Dr. Burg recommends. Without proper guidance, adding more medications to the mix might do more harm than good.
Advertisement
Learn more about our editorial process.
Advertisement

Exercising can actually improve arthritis symptoms — and low-impact exercises are best

Over-the-counter pain medications, typing pads and wrist braces can help when you’re in a wrist pinch

Research shows a strong association between rheumatoid arthritis and heart issues
It’s always a good idea to let a healthcare provider know about any back pain you’re experiencing, especially if it results from trauma or persists longer than three months

From physical and biofeedback therapy to nerve ablations and blocks, there are many nonsurgical options for managing back pain
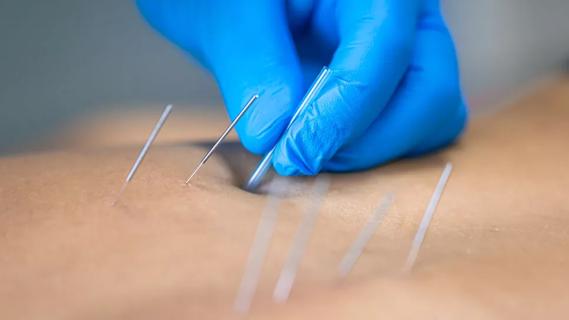
Both can help reduce pain, but they’re very different in terms of origins, philosophies and practices

Use foot warmers and hand warmers, layer your clothing and avoid sharp shifts in temperature
As part of a larger treatment strategy, it can help decrease muscle tightness and reduce pain

Focus on your body’s metabolic set point by eating healthy foods, making exercise a part of your routine and reducing stress

PFAS chemicals may make life easier — but they aren’t always so easy on the human body

While there’s little risk in trying this hair care treatment, there isn’t much science to back up the claims