Advertisement
Lung cancer doesn't just affect people who smoke

If you think you’re safe from lung cancer because you’ve never smoked, think again.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
While cigarette smoking is the No. 1 cause of lung cancer, you also can get it from breathing secondhand smoke, being exposed to asbestos or radon, or having a family history of lung cancer.
Many people think lung cancer always is the result of a personal choice to smoke cigarettes and don’t see those with lung cancer in the same light as, say, those who have breast cancer. However, the vast majority of people who die from lung cancer quit smoking long before they received a lung cancer diagnosis.
“There’s a huge stigma associated with lung cancer because the majority of people who die from either smoke or used to smoke,” says oncologist Nathan Pennell, MD, PhD. “The fact is that anyone who has lungs can be exposed to carcinogens and develop lung cancer, so this is a disease that should concern everyone.”
One of the first questions people usually ask when they find out someone has lung cancer is, “Did they smoke?”
“Tobacco smoke is one of the most addictive substances known to man. Addiction is a disease,” says Dr. Pennell. “Many people who smoke become addicted as teenagers. Whether you smoke or not, nobody deserves to die from lung cancer.”
Lung cancer is the leading cause of cancer death among men and women in the United States. Unfortunately, because of the stigma associated with lung cancer, it is difficult for researchers to get funding to try to find a cure.
“Public funding has a lot to do with politics and public opinion doesn’t support lung cancer as it does the so-called ‘blameless cancers’ like breast cancer or prostate cancer,” says Dr. Pennell. “Those types of cancers also have a lot more survivors who can advocate for funding.”
A Northwestern University study found that underfunding common cancers like lung cancer could negatively impact research, drug development and the number of FDA drug approvals for those poorly funded cancers.
“There are not enough lung cancer survivors to demand change,” says Dr. Pennell. “Those who do survive often blame themselves, so there is a smaller percentage of survivors who are willing to tell their stories.”
Despite funding difficulties, medicine has made progress in lung cancer diagnosis and treatments and genetic testing is just one example.
“There are many different types of lung cancer,” says Dr. Pennell. “Genetic testing has helped researchers to develop therapies that target specific types of cancer cells.”
Immune-based therapies, in which the immune system is primed to attack tumors, are also helping patients with lung cancer live longer. These therapies have been approved for treating many other types of cancer as well.
Advertisement
Development of screening tools such as CT scans help with early identification of lung cancer, too, which could save tens of thousands of lives. Lung cancer screenings are another popular way to catch the cancer. Available for high-risk healthy people 55 to 77 years old, lung cancer screenings search for lung cancer in hopes of finding it at an early stage.
While not all lung cancers can be prevented, you can take some measures that may lower your risk. First and foremost, quit smoking, if you currently do, because the benefits go beyond external changes. For example, if you stop smoking for 10 years, your risk of lung cancer death is about half of that of someone who currently smokes.
A healthy diet is also crucial in not only maintaining your weight, but it can also reduce your risk of lung cancer. Lastly, reduce any exposure to chemicals like asbestos and radon.
Lung cancer research is still underfunded. It needs financial support and advocating for support for lung cancer research could be the key to funding the research that discovers a cure.
“I would encourage survivors, especially those who never smoked, to advocate for lung cancer research and to let people know that progress is being made,” says Dr. Pennell. “We need to get the word out about how important this is to everyone, not just to those who smoke.”
Advertisement
Learn more about our editorial process.
Advertisement

Vaping exposes you to thousands of chemicals, including many that cause cancer and lung disease

Your risk goes down once you quit, but you may still need a lung cancer screening
Early detection of the disease can extend your life, but there are specific testing guidelines
Knowing the signs (like a cough that won’t quit) may help some people detect lung cancer early

Toxic chemicals stay on surfaces long after smoke clears
Early detection and screening are important
Early detection through screening can improve survival numbers
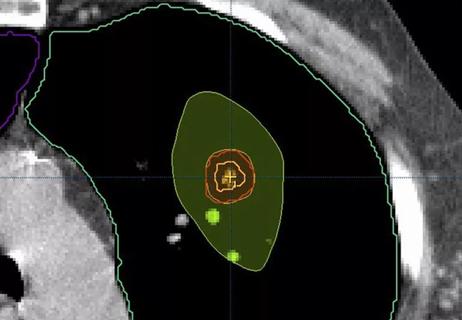
SBRT is an effective option when you’re too frail for surgery

Focus on your body’s metabolic set point by eating healthy foods, making exercise a part of your routine and reducing stress

PFAS chemicals may make life easier — but they aren’t always so easy on the human body

While there’s little risk in trying this hair care treatment, there isn’t much science to back up the claims