Advertisement
SBRT is an effective option when you’re too frail for surgery
Your doctor says you have early-stage lung cancer. Although it’s always difficult to learn that you have cancer, outcomes are typically better when you catch and treat lung cancer in its early stages.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
But what if surgery is just not an option for you? What else can you do if you’re told that your other medical issues make undergoing the operation much too risky for you or isn’t safe?
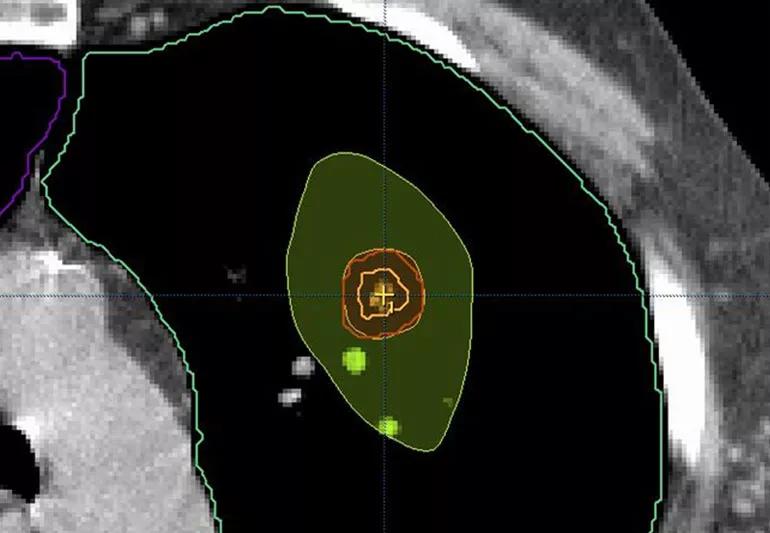
For such patients, a special form of radiation therapy ― specifically stereotactic body radiation therapy (SBRT) ― has been found to be effective at getting rid of the cancer, says radiation oncologist Gregory Videtic, MD.
In general, radiation therapy uses high energy X-rays to kill cancer cells while normal body cells touched by them can repair themselves. Treatments are usually given over many weeks to balance the benefits and the repair.
By comparison, SBRT delivers an extremely high dose of radiation that’s precisely focused to a small targeted area, such as a lung cancer that’s only in the lung and hasn’t spread anywhere else. Because treatment is pinpointed on the tumor only, this means that damage to surrounding normal tissue is also limited. Plus, treatment can be much faster than traditional radiation therapy.
SBRT is an outpatient procedure often done over three to five appointments. The number of sessions is chosen by the radiation oncologist, based on the size and location of the tumor in the chest. Some larger medical centers with a lot of experience, including Cleveland Clinic, may also offer a single-dose SBRT treatment for certain tumors.
There are several reasons why you and your doctor ― usually a surgeon and/or a lung doctor (a pulmonologist) ― may decide that a non-surgical option is best for you.
You may have multiple medical problems or a specific disease or illness that makes you unable to withstand surgery.
This might mean you have poor lung function because of COPD or a heart condition such as congestive heart failure, for instance. In other words, removing any lung or putting your heart under stress could be too much for your body to handle.
“Sometimes, especially with elderly patients, they don’t feel strong enough to go through surgery,” Dr. Videtic says.
Any surgical procedure has potential risks. There are some patients who don’t want an operation if there’s an alternative.
“In some areas of the country, and even worldwide, there are patients who have to travel really long distances to undergo surgery which makes short-course radiation therapy very handy,” Dr. Videtic says. “They get in, get out, and go about their life.”
The two main types of lung cancer are non-small cell and small cell.
Of these two types, it is generally non-small cell that may show up in the early stage, although even then only a minority of patients with lung cancer will have this early diagnosis. Early stage means that the cancer has been found to be only in the lung, not spread to the glands (or lymph nodes) in the middle of the chest that drain the lungs, and not been found in any other parts of the body outside the chest.
In other words, if your doctor says surgery is not safe for you, radiation may be offered as an alternative for you if:
Advertisement
In this case, we like to treat the patient with SBRT. A very high dose of radiation is given to just the tumor during three to five sessions. It’s very quick.
The success rate of SBRT matches that of surgery, Dr. Videtic says.
“It’s 85 percent to 95 percent, depending on what study you read,” he says. “So it’s extremely effective and doesn’t require anesthesia or recovery from a larger surgery.”
When oncologists use radiation in high doses to get rid of your lung cancer, safety is also their No. 1 concern.
“We have a radiation oncology physicist, physician and therapist all present during the entire planning and treatment process. The patient is well monitored,” Dr. Videtic says. “Also, once we create a plan, a second physician and physicist review that plan. We take our patients’ safety seriously.”
Before SBRT became available, radiation doctors would still try to help patients who were not safe for surgery with older-style radiation. But there was always a worry of damaging too much lung in already frail patients since the radiation wasn’t pinpointed.
“Radiation is a scary word,” he acknowledges. “But for years, all we could do was watch the tumor grow until we were forced to do something. Of course, the bigger the tumor, the less likely we are able to control it.
“But today, thanks to SBRT, we have this excellent treatment for otherwise inoperable patients. And the patients have been quite pleased with the results.”
Advertisement
Learn more about our editorial process.
Advertisement

Vaping exposes you to thousands of chemicals, including many that cause cancer and lung disease

Medications, tubing and stress can steal away the ZZZs you need

Your risk goes down once you quit, but you may still need a lung cancer screening
Early detection of the disease can extend your life, but there are specific testing guidelines

Practice meditation together, make a unique-to-them care package and embrace emotions
Knowing the signs (like a cough that won’t quit) may help some people detect lung cancer early

Thoughts and feelings can change over time; relaxation, self-care and support groups can help

Misconceptions can be worse than reality

Focus on your body’s metabolic set point by eating healthy foods, making exercise a part of your routine and reducing stress

PFAS chemicals may make life easier — but they aren’t always so easy on the human body

While there’s little risk in trying this hair care treatment, there isn’t much science to back up the claims