Advertisement
Understanding care for this dangerous type of aneurysm
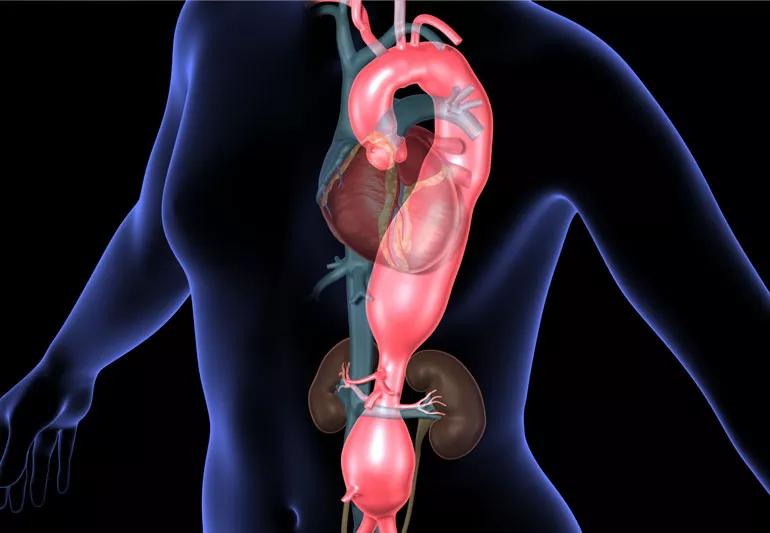
The aorta is the largest blood vessel in the body and arguably the most important: It carries oxygenated blood away from the heart to all parts of the body.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The section that runs from the heart through the chest is called the thoracic aorta.
When a section of aorta wall weakens, it may bulge as blood surges through it. A bulge, or aneurysm, increases the risk the aorta will burst (rupture) or tear apart (dissect). Both scenarios are medical emergencies that many patients do
not survive. That’s why preventing a rupture or dissection is so important.
“As soon as a thoracic aortic aneurysm is discovered, the patient should see a cardiologist with expertise in aortic disease. This provides the best chance of appropriate and timely decisions about managing the aneurysm to prevent a catastrophe,” says Aorta Center Director Eric Roselli, MD.
Until an aneurysm reaches a certain size, there are many things that can be done to lessen stress on the artery wall. Maintaining tight blood pressure control is critical. New guidelines recommend achieving a target blood pressure less than 130/80 millimeters of mercury (mmHg), which Cleveland Clinic believes is a critical goal for patients with thoracic aneurysm. “This usually requires a medication such as beta blockers. Even a low dose may be helpful,” says Dr. Roselli.
Most patients with thoracic aortic aneurysm may safely participate in moderately intense aerobic activities, such as walking, jogging or cycling.
Lifting weights or other heavy items should be discouraged, since this may cause a significant short-term increase in blood pressure.
We do not have strong evidence to support specific recommendations about exercise limitations, but in theory, lifting more than half your body weight could increase your blood pressure enough to cause a weak aorta wall to rupture or dissect.
When patients are involved in competitive sports, activity restrictions should be tailored to the risk of dissection or rupture. “We may recommend exercise stress testing to assess a patient’s heart rate and blood pressure response to exercise,” says Dr. Roselli. “We are developing research protocols to learn more about the interaction between these variables so activity recommendations can be tailored to the individual.”
The growth of a thoracic aortic aneurysm is carefully monitored, since it is unlikely to cause symptoms until the moment it ruptures or dissects.
Surgery is generally recommended when an aneurysm reaches 5.0 to 5.5 centimeters (cm, or about 2 inches) in diameter or grows more than 0.5 cm per year.
Surgery may be advised earlier in patients with a family history of aortic disease, a bicuspid aortic valve or a known connective tissue disorder, due to increased risk of rupture at a smaller diameter.
In older, sicker patients, the risks of surgery may be greater than the risk that a smaller aneurysm will dissect or rupture.
“We find it is psychologically beneficial for patients to meet with a surgeon relatively early in the course of treatment to learn what surgery involves, its risks and benefits, and to gain some reassurance that we can manage most of these problems very safely,” says Dr. Roselli.
Advertisement
If the patient has a family history of aortic dissection, surgery may be recommended when the aneurysm reaches the diameter of the family member’s aorta when the dissection occurred. In some cases, the threshold to operate may be particularly low.
“At our center, we routinely recommend patients with thoracic aortic aneurysm visit a clinical geneticist and have all first-degree relatives screened if there is a suggestion of a family history,” says Dr. Roselli.
This article originally appeared in Cleveland Clinic Heart Advisor.
Advertisement
Learn more about our editorial process.
Advertisement

Factors like temperature, energy levels and sleep quality play a role in determining whether working out in the morning or evening is best for you

Obesity, age and preexisting heart conditions can all raise your risk of cardiovascular disease during pregnancy

Xylitol in processed food can increase risk of heart attack and stroke — but there’s no danger in xylitol in oral care products

If your provider has ruled out a serious cause, you can treat chest pain at home with antacids, inhalers or anti-inflammatory medications

Walking is a great goal, but how many steps are best for you depends on factors like your fitness level and age

Research shows a strong association between rheumatoid arthritis and heart issues

Eating more natural, whole foods can lower your risk of heart and cardiovascular diseases

First things first — slowly sit or lie down

Focus on your body’s metabolic set point by eating healthy foods, making exercise a part of your routine and reducing stress

PFAS chemicals may make life easier — but they aren’t always so easy on the human body

While there’s little risk in trying this hair care treatment, there isn’t much science to back up the claims