Advertisement
Three alternatives to open-heart surgery
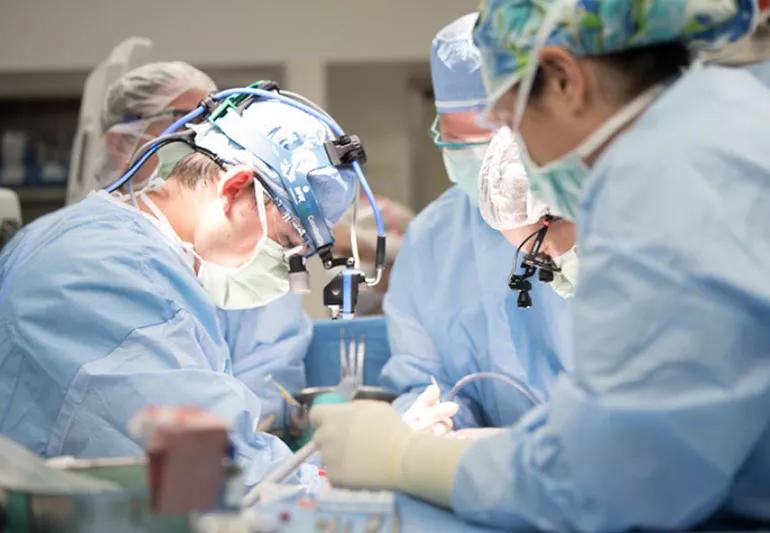
When you hear that you need heart surgery, you may see a picture in your head of a surgeon performing open-heart surgery. If that picture makes you nervous, you can take a sigh of relief because surgeons perform many heart surgeries with a minimally invasive or small-incision approach.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The benefits of these less invasive surgeries are less bleeding, less trauma, fewer infections and a quicker recovery, says cardiac surgeon Daniel Burns, MD.
In minimally invasive surgery, the surgeon makes smaller incisions (sometimes as small as a keyhole) with or without the use of robotics. Dr. Burns explains how this approach works best for three types of heart surgeries:
A valve operation, with either a valve repair or a valve replacement, is the most common minimally invasive procedure for heart surgery.
“We perform these through the side of the chest, a small incision over the breastbone or sometimes even with robotic assistance,” says Dr. Burns.
Traditional heart surgery requires a large incision (typically 6 to 8 inches in length) over the middle of the breastbone (sternum), but these heart valve operations reduce incisions to 2 to 4 inches in length. Not only does this reduce pain and blood loss, but it leaves less scarring and you likely will have a shorter hospital stay.
Through robotically-assisted valve surgery, surgeons use a specially designed computer console to control surgical tools on thin robotic arms. The robotic arms gently ease into separate 8 mm incisions in the right side of your chest, combined with a 4 cm main incision between the ribs. The surgeon’s hands then control the endoscopic tools to open the pericardium (the thin sac around the heart) to perform the surgery.
Coronary artery bypass grafting (CABG) is performed with a small- incision approach, either through the center of the chest or through the side.
“We tend to reserve this procedure for patients who need one or two bypass grafts,” says Dr. Burns. “Through a CABG, we bypass one or more blocked coronary arteries with a blood vessel graft to restore normal blood flow to the heart.”
These grafts usually come from the patient’s own arteries and veins located in the chest, leg or arm.
CABG is performed by putting the graft around the blocked arteries to create new pathways for oxygen-rich blood to flow to your heart. The goals of the surgery are to relieve symptoms of coronary artery disease, allow you to return to a normal lifestyle and lower your risk of a heart attack or other heart problems.
The other good news is that while you will have a scar on your chest from the incision, and where the grafted blood vessels were taken from, the scars will gradually fade over time.
“It’ll take about two months to recover from CABG,” he says. “Your overall health and the outcome of the operation plays a big role in how you’ll feel after you get out of surgery.”
Some surgeons perform aortic procedures, such as aneurysm repair, through small incisions. Occasionally, aortic aneurysm, or Type B dissection repair, can be achieved through a small groin incision used to place a stent graft from the inside of the artery.
If you have high blood pressure or a disease that affects the connective tissues of your body, the aortic artery sometimes develops a dissection (or a tear) in its arterial lining. Your blood normally flows through the aortic artery like water inside a garden hose. When a tear occurs, your blood flows through the torn segment as well, creating two passages
Advertisement
“With a Type B dissection, a tear occurs in the part of the aortic artery that runs through your chest and abdomen into the organs and lower extremities,” says Dr. Burns. “In the past, we could only repair it through open surgery.”
Type B dissection is now fixed via a minimally invasive approach by using a stent. The surgeon inserts a tiny tube through the groin into the aortic artery and expands it to seal off the tear — and keeps the torn part of the artery open.
In choosing the best surgery option, it’s important for you to find a heart surgeon with experience in all approaches. The two of you then can work together as a team to decide how best to fix your problem.
“Be sure your surgeon knows that you want to explore a minimally invasive option,” says Dr. Burns. “Don’t be afraid to ask questions. Ask how frequently they do the surgery so you can get an idea of how comfortable and experienced the surgeon is.”
Advertisement
Learn more about our editorial process.
Advertisement

Factors like temperature, energy levels and sleep quality play a role in determining whether working out in the morning or evening is best for you

Advances in technology and medications have made the process safer than ever

Keep the area clean and monitor your incision site for discharge, odor or a change in appearance

Obesity, age and preexisting heart conditions can all raise your risk of cardiovascular disease during pregnancy

Xylitol in processed food can increase risk of heart attack and stroke — but there’s no danger in xylitol in oral care products

If your provider has ruled out a serious cause, you can treat chest pain at home with antacids, inhalers or anti-inflammatory medications

Walking is a great goal, but how many steps are best for you depends on factors like your fitness level and age

Research shows a strong association between rheumatoid arthritis and heart issues

Focus on your body’s metabolic set point by eating healthy foods, making exercise a part of your routine and reducing stress

PFAS chemicals may make life easier — but they aren’t always so easy on the human body

While there’s little risk in trying this hair care treatment, there isn’t much science to back up the claims