Unlike varicose veins, spider veins don't necessarily indicate poor circulation
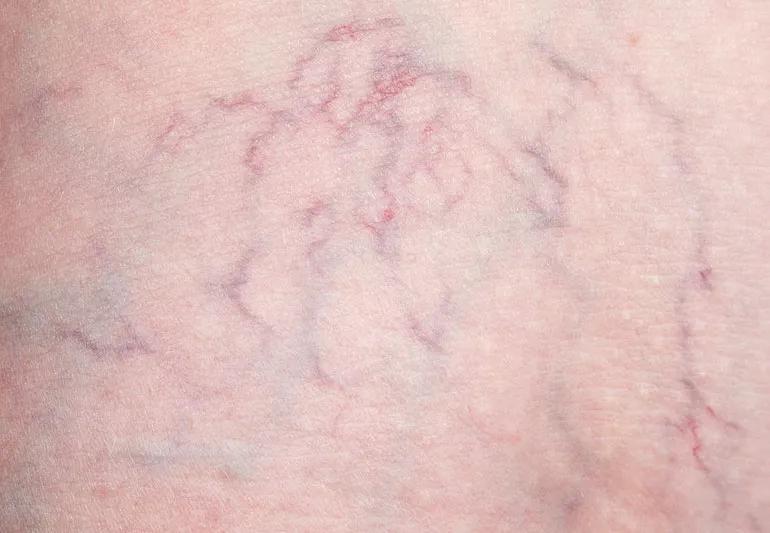
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/944857af-f3f4-4615-a280-0120a817c271/spider-Veins-on-leg-184277101-770x533-1_jpg)
Closeup of spider veins on leg.
Most of us only pay attention to our blood vessels when something isn’t quite right. But when something is wrong, they can be hard to ignore.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
That’s especially true of varicose veins and spider veins because they impact our appearance.
While they can be a source of discomfort and even annoyance, most of us don’t fully understand what varicose and spider veins are, much less how to tell them apart.
We talked to vascular medicine specialist Meghann McCarthy, DO, about the differences between varicose veins and spider veins. She explains the causes, symptoms, treatments and what the two conditions mean for your health.
Varicose veins are larger than spider veins and more readily visible to the naked eye. They usually look like lumps, bumps or ropey nodules underneath your skin. Depending on its size and where it’s located, a varicose vein can also have a blue-green appearance.
Varicose veins form on your legs, feet and ankles.
Varicose veins can also form in the scrotum. Those are referred to as varicoceles, and are handled differently from other varicose veins.
Spider veins (telangiectasias) affect smaller blood vessels than the ones you see in varicose veins. Spider veins form when smaller venous structures — like capillaries, venules and arterioles — are damaged in some way.
Like varicose veins, spider veins can be red, blue purple or green. And, as you’ve probably already guessed, they tend to show up in clusters that resemble a spider web.
Advertisement
“Spider veins are more wispy and smaller than varicose veins, almost like little blue hairs on the skin’s surface. And they tend to be much more superficial,” Dr. McCarthy explains. “You usually can’t feel them if you run your hands over them.”
While you can get spider veins anywhere, they’re most common on your legs and face.
If you’re trying to figure out if you’re dealing with a varicose or a spider vein, this table may help:
| Varicose veins | Spider veins | |
|---|---|---|
| Location | Veins in your legs, feet and ankles. | Small blood vessels anywhere, but mostly on your legs and face. |
| Appearance | Lumps or ropey nodules. Sometimes blue, green or purple. | Small, spiderweb or branch-like clusters of veins. Can be red, blue, green or purple. |
| Are the veins 3D? | Yes. | Sometimes. |
| Size | >3 millimeters wide. | <1 millimeter wide. |
| Symptoms | Itching, pain, swelling and venous leg ulcers. | Usually asymptomatic. See a healthcare provider about itching, burning or cramping. |
| Location | ||
| Varicose veins | ||
| Veins in your legs, feet and ankles. | ||
| Spider veins | ||
| Small blood vessels anywhere, but mostly on your legs and face. | ||
| Appearance | ||
| Varicose veins | ||
| Lumps or ropey nodules. Sometimes blue, green or purple. | ||
| Spider veins | ||
| Small, spiderweb or branch-like clusters of veins. Can be red, blue, green or purple. | ||
| Are the veins 3D? | ||
| Varicose veins | ||
| Yes. | ||
| Spider veins | ||
| Sometimes. | ||
| Size | ||
| Varicose veins | ||
| >3 millimeters wide. | ||
| Spider veins | ||
| <1 millimeter wide. | ||
| Symptoms | ||
| Varicose veins | ||
| Itching, pain, swelling and venous leg ulcers. | ||
| Spider veins | ||
| Usually asymptomatic. See a healthcare provider about itching, burning or cramping. |
For many people who get them, varicose veins are no big deal and don’t cause any complications. But others experience troublesome symptoms like itching, pain and swelling.
People with severe varicose veins occasionally develop venous leg ulcers, which are open sores that stubbornly refuse to heal and require medical attention.
Most spider veins are a purely cosmetic concern. In rare cases, spider veins can cause uncomfortable symptoms like burning, itching and cramping. In those cases, it’s important to check with a healthcare provider. It could be a sign of an underlying medical condition.
Varicose veins are very common. Approximately one-third of us will develop them at some point in our lives.
Our vascular system has a tough job: Circulating blood throughout our body requires that our veins to fight against gravity. According to Dr. McCarthy, there are valves in our veins that help prevent blood from flowing backward toward our feet. Varicose veins form when one or more of those valves aren’t working properly.
Varicose veins develop for many reasons. Here are some of the most common:
Spider veins are even more common than varicose veins, but we don’t know as much about what causes them. That’s at least in part because blood vessels can be damaged in many different ways.
We do know that factors can influence how early you develop spider veins, including:
Varicose veins and spider veins are both extremely common — and having one can be an indication that you’re likely to develop the other. The two conditions also have a genetic component: If members of your immediate family have vein issues, it’s pretty likely you’ll develop them at some point, too.
Generally speaking, women are more prone to both varicose veins and spider veins. Dr. McCarthy explains that’s probably because hormones like estrogen fluctuate dramatically throughout women’s lives, from puberty and possible pregnancy to menopause and post-menopause.
Advertisement
Your career choice and hobbies can also raise your risk for vein issues. Activities that have you on your feet all day put pressure on your legs, which Dr. McCarthy says can form spider veins. Oddly enough, being too sedentary can have the same effect!
Most people with varicose veins don’t have any complications. But complications are possible. And when they happen, they can be dangerous.
Advertisement
Severe varicose veins may also be a sign of a condition called chronic venous insufficiency (CVI). If you have varicose veins and your legs are swollen and discolored all the time, speak to a doctor.
Unlike varicose veins — which can have a host of complications and may be a sign of an underlying health condition — spider veins are usually harmless.
“When you look up spider veins online, you may see a lot of scary stuff,” Dr. McCarthy notes. “But they generally are a benign thing and don’t usually indicate a health problem.”
There’s only so much you can do to prevent varicose veins and spider veins. For many of us, they’re inevitable. But doing the following things can help keep your vein issues from getting worse:
Advertisement
The first step in varicose vein treatment involves making a series of lifestyle changes, including wearing compression stockings, elevating your legs throughout the day, adjusting your diet, etc.
If home remedies are unsuccessful, or if you’re bothered by your veins’ appearance, there are three different procedures available: endovenous thermal ablation (laser therapy), injection therapy (sclerotherapy) or vein surgery (ligation and stripping).
Spider veins rarely require any kind of treatment, as they don’t cause symptoms and aren’t normally a sign of a larger health problem. But a lot of people don’t like how spider veins look — especially as, unlike varicose veins, you can get them all over your body.
“If the appearance is bothersome to you, then that’s a good enough reason to talk to your doctor,” Dr. McCarthy says. “There’s always things that can be done to treat just for appearance purposes.”
The most common spider vein treatments are laser and injection therapy.
Varicose veins and spider veins are two distinct medical conditions, but they have a lot in common, including causes, risk factors and even some treatment options. In fact, it’s common for people who have spider veins to develop varicose veins — and vice versa!
At the end of the day, there’s one very important question you need to ask yourself: “Are my veins bothersome or causing me any symptoms?”
If the answer to that question is yes, Dr. McCarthy encourages you to get your veins seen by a healthcare provider. They’ll be able to tell you whether your symptoms are a sign of an underlying health condition and recommend the best treatment option for your specific situation.

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about our editorial process.
Advertisement
At-home treatments and lifestyle changes may help ease the symptoms and improve the appearance of varicose veins — but they aren’t a cure
Regular exercise, an iron-rich diet, adequate sleep and bedtime routines that include a warm bath or massage may help with your kid’s RLS
Cardio can reduce the appearance of varicose veins, but only temporarily
It could be your feet need a rest, but swollen legs may also be a sign of a serious condition
Some symptoms should be taken seriously
Pain may signal a damaged nerve or herniated disk
Strategies for getting the sleep you need
The short answer from an interventional cardiologist
These tiny saltwater larvae can get trapped under your swimsuit and trigger an itchy reaction called seabather’s eruption
Searching nature for edible items requires training and knowledge to avoid poisonous plants
Yes, but you can protect yourself with hats, scarves or even hair sunblock