Advertisement
From benefits to side effects
Cholesterol-lowering statin medications have been at the forefront of managing cardiovascular disease for several decades now. Why? It’s because a large body of research supports their benefits in reducing the risk of heart attack and stroke.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The drugs have become so universally used that if you haven’t been prescribed a statin already, chances are you will at some point.
Preventive cardiologist Luke Laffin, MD, says statins lower your LDL ( or “bad”) cholesterol, which is associated with a reduced risk of atherosclerotic cardiovascular disease. (That’s the buildup of cholesterol, fatty cells and inflammatory deposits on the inner walls of your arteries aka “hardening” or “clogging” of the arteries).
“Additionally, statins lower inflammation, which we know is a factor that causes atherosclerosis and cardiovascular disease,” Dr. Laffin says.
Yet, despite their many benefits, statins (like all medications) have some important side effects you need to know about. So, review the risks and benefits of these important medications with your physician, and discuss your need for statin therapy.
Statins inhibit the action of an enzyme that’s responsible for cholesterol production in your liver. In the process, they significantly reduce LDL and total cholesterol, while also having beneficial effects on HDL (“good”) cholesterol, triglycerides and inflammation. Some evidence suggests that high-intensity statin therapy may help to slow, and potentially reverse, the growth of artery-clogging atherosclerotic plaques. They may also make them less prone to rupture and cause heart attacks and strokes.
“There are good data to suggest that the more LDL lowering we can achieve, the lower the risk of adverse cardiac events such as strokes and heart attacks,” Dr. Laffin explains.
Although statins all belong to the same drug class, they differ in how potent they are and how much they can lower LDL cholesterol.
Your doctor will use a tool like the American College of Cardiology/American Heart Association risk calculator and other factors to gauge your long-term risk of atherosclerotic cardiovascular disease, determine if you need statin therapy, and if so, which one.
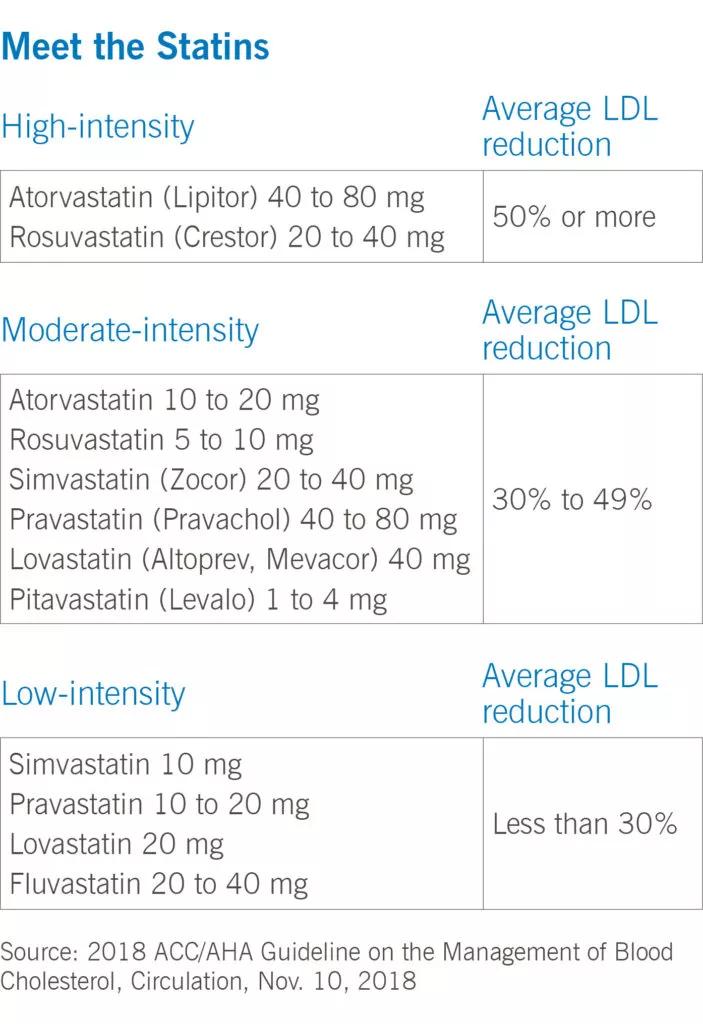
The statins are generally taken once daily and are available in generic forms. “It’s important to note that atorvastatin and rosuvastatin really are the workhorses of cardiology and statins at this point,” Dr. Laffin adds. “A lot of pharmacies typically will have one of the high-intensity statins. They’re inexpensive and easy to obtain. In my experience, 99% of insurance companies cover at least one of them, and more than 75% cover both of them.”
Guidelines from the American College of Cardiology and American Heart Association recommend statin therapy for:
Advertisement
* These factors include a family history of ASCVD, LDL levels persistently ≥160 mg/dL, triglyceride levels persistently ≥175 mg/dL, chronic kidney disease, ethnicity, inflammatory diseases, metabolic syndrome, and (in certain people, if measured) results of high-sensitivity C-reactive protein, lipoprotein(a), and apolipoprotein B. Note: The guidelines recommend considering coronary artery calcium scoring for people at intermediate risk in whom a decision about starting statin treatment remains uncertain.
Elevated liver enzymes. In addition to more common side effects such as headache and nausea, statins occasionally may cause increases in liver enzymes, suggesting liver inflammation. However, the latest ACC/AHA guidelines recommend liver-enzyme testing only for statin users who are at higher risk or have symptoms that may suggest liver toxicity. Furthermore, statins may cause small elevations in blood sugar, enough to push some people into the range of type 2 diabetes. “But, we know that the benefits of statins outweigh that small increase in blood glucose across multiple populations,” Dr. Laffin notes.
Mental fogginess. While some studies have identified positive effects of statins on cognitive function, some users have reported problems like mental fogginess and forgetfulness, which go away after stopping the drug. Overall, though, large-scale clinical trials don’t suggest an increase in cognitive problems associated with statin use, Dr. Laffin says.
Muscle pain. One of the most noteworthy side effects associated with statin therapy is muscle aching and stiffness, which can be more severe as the statin dose and potency increase and may make some people intolerant to the drugs. Certain statins — in particular, atorvastatin and simvastatin — are more likely to cause these side effects, while others, like rosuvastatin and pravastatin, have less of an effect.
Advertisement
Some treatable conditions (like thyroid dysfunction and severe vitamin D deficiency) may contribute to statin intolerance. So may consuming large quantities of grapefruit (or juice) and taking certain medications. Addressing these factors may ease or prevent statin-related muscle effects. Also, some people have found that taking coenzyme Q10 supplements may help, although the ACC/AHA guidelines don’t recommend their use.
It’s important not to stop taking your statin and to report any muscle side effects to your physician. Your doctor may switch you to a less-potent statin, change the dose, or explore alternative dosing strategies. This may include taking the drugs every other day or less frequently. With some perseverance, you and your physician can develop a statin regimen that works for you.
“Usually, you can find at least some dose of statin that people can tolerate, even if it is just a couple times a week,” Dr. Laffin says. “If you absolutely cannot tolerate a statin at any dose, then we have other medications we can use,” such as ezetimibe (Zetia®) or newer drugs known as PCSK9 inhibitors: alirocumab (Praluent®) and evolocumab (Repatha®).
Age is the most significant risk factor for atherosclerotic cardiovascular disease. However, the risks and benefits of statins must be carefully considered in older populations, especially those with health problems.
Older adults, as a whole, may be more likely than their younger counterparts to experience serious side effects from statins. Many seniors take multiple medications, making them more likely to experience adverse medication interactions with a statin. Importantly, seniors with other medical conditions that shorten their life expectancy may not reap the benefits of statin therapy.
So, if you’re over age 75 — and especially if you have other health problems — discuss the pros and cons of statin therapy with your physician, Dr. Laffin advises.
“The effects of statins are usually over the long term—we’re talking five to 10 years in terms of cardiovascular risk reduction,” he explains. “So, you have to balance the risk of taking another medicine versus whether you are going to die from something else in those five to 10 years. I think it’s very reasonable for someone who has other competing comorbidities to talk about deprescribing statins.”
This article first appeared in Cleveland Clinic Men’s Health Advisor.
Advertisement
Learn more about our editorial process.
Advertisement

Factors like temperature, energy levels and sleep quality play a role in determining whether working out in the morning or evening is best for you

Lifestyle adjustments can help you raise your HDL, the ‘good’ cholesterol

Obesity, age and preexisting heart conditions can all raise your risk of cardiovascular disease during pregnancy

Xylitol in processed food can increase risk of heart attack and stroke — but there’s no danger in xylitol in oral care products

If your provider has ruled out a serious cause, you can treat chest pain at home with antacids, inhalers or anti-inflammatory medications

Walking is a great goal, but how many steps are best for you depends on factors like your fitness level and age

Research shows a strong association between rheumatoid arthritis and heart issues

The scenarios vary based on how many pills you’ve missed and whether you take a combination pill or progestin-only pill

Focus on your body’s metabolic set point by eating healthy foods, making exercise a part of your routine and reducing stress

PFAS chemicals may make life easier — but they aren’t always so easy on the human body

While there’s little risk in trying this hair care treatment, there isn’t much science to back up the claims