Advertisement
Understand how these imaging tests differ
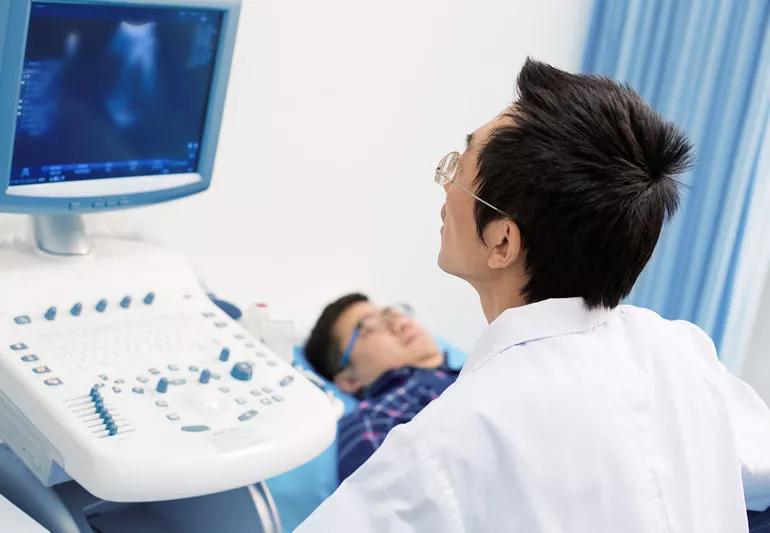
When aches, pains and other symptoms stem from a problem with the musculoskeletal system (meaning the bones, muscles, cartilage, tendons, ligaments and joints) your doctor may order an imaging test to help determine the underlying cause.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
There are several ways of looking inside the body, including X-rays, computed tomography (CT) scans and magnetic resonance imaging (MRI). Another one, high-resolution ultrasound, offers some advantages over the others for musculoskeletal problems.
“Some common reasons we do musculoskeletal ultrasound are to evaluate the rotator cuff in the shoulder, to look for Achilles tendon tears and to evaluate elbow tendon problems,” says diagnostic radiologist Michael C. Forney, MD. “But an ultrasound can be performed on most joints as long as the area evaluated is limited to just part of the joint.”
“Sometimes patients wonder why an ultrasound is ordered instead of an MRI for musculoskeletal problems.” Dr. Forney says.
MRI and ultrasound look at the body in different ways.
MRI, which uses powerful magnets to produce 3-D anatomic images, is a high-contrast resolution modality that can determine changes in the tissue quality. With a muscle injury, for example, MRI images often show a bright signal indicating that there is more water in the muscle, which is a sign of injury.
Ultrasound uses high-frequency sound waves to look at organs and structures. It is a high-spatial resolution modality that provides greater, high-level detail of a structure, especially when it’s not too deep from the skin’s surface. “Ultrasound is like a flashlight that allows us to see high detail over a small area of tissue,” Dr. Forney says.
“Ultrasound has many advantages as an imaging modality,” Dr. Forney says. “Ultrasound does not use any radiation and does require the patient to enter the bore or tube of a scanner, like with MRI or CT.”
Ultrasound can show pictures in real-time, like a movie, and therefore, can demonstrate abnormalities that are only seen with motion like impingent of the bursa in the shoulder, he explains.
“When structures are not very deep, or superficial, ultrasound can show images with higher resolution/detail than MRI,” Dr. Forney notes. The tendons in the fingers are often seen in greater detail with ultrasound compared with MRI, for example.
“Since ultrasound is like a flashlight, whereas MRI is like a flood light, there are times when ultrasound may not be able to make the diagnosis or may show findings that are indeterminate and need further testing,” he adds. “Nevertheless, ultrasound very often makes a diagnosis or provides useful information to your doctor about a musculoskeletal problem.”
Ultrasound isn’t just a diagnostic tool. When some type of injection treatment is needed, such as a corticosteroid shot into a joint, ultrasound can be used to visualize the structure to ensure that the needle is placed in the correct location.
Image-guided joint injections also are done with X-rays or CT scans. But with ultrasound, there’s no radiation and no need to inject a contrast dye.
With ultrasound, a specially trained technician or sonographer moves a handheld probe over the area to be studied. Once the sonographer feels that they have acquired diagnostic images, the radiologist will then interpret those images, typically within 24 hours.
Advertisement
“While we schedule most ultrasound patients for an hour, some examinations may take more or less time depending on what the sonographer finds,” Dr. Forney says.
Ultrasound does have some limitations, and there are situations when MRI is needed instead. “Ultrasound does not show the structures inside joints,” Dr. Forney says. “We can only see the soft tissues outside, around the joint.”
To evaluate damage to cartilage, bone or other structures inside and around a joint, MRI is the better choice. MRI is also preferred for conditions that impact deep or large areas since ultrasound can evaluate only a small area at a time.
“If a patient needs a detailed look an entire joint, an MRI is a better test,” Dr. Forney says. Many times, however, your doctor may start with an ultrasound.
This article was adapted from Cleveland Clinic Arthritis Advisor.
Advertisement
Learn more about our editorial process.
Advertisement
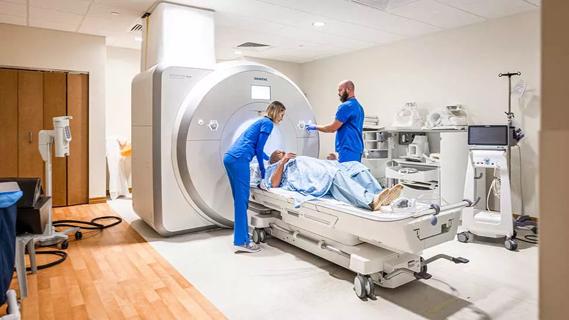
CTs and MRIs use different technologies to show different things — neither is necessarily ’better’ than the other
This noninvasive procedure can help aging skin by boosting collagen production
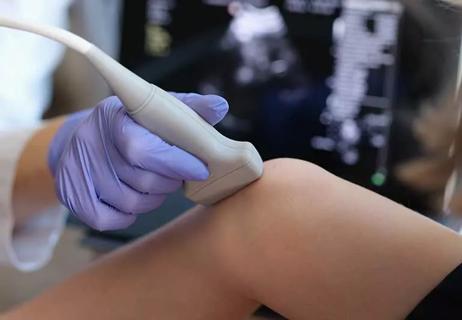
One medical test, two different parts
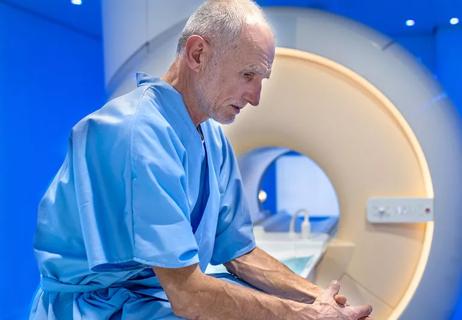
What to know about cardiac implants and imaging tests
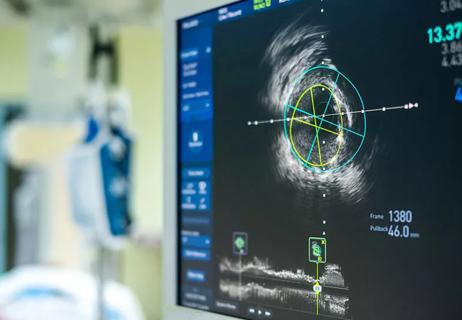
Understand who may (and may not) benefit

Footwear that offers cushioning plus heel and arch support can help you relieve and manage symptoms

Over-the-counter pain medications, typing pads and wrist braces can help when you’re in a wrist pinch
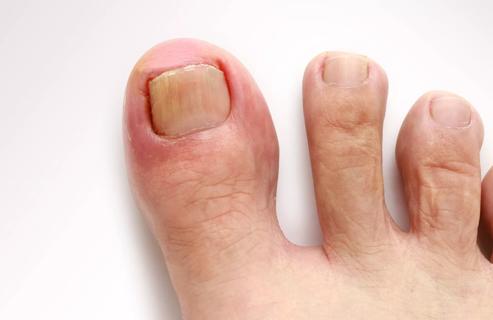
Pain meds, toenail protectors and petrolatum jelly may spare you a trip to a podiatrist

Focus on your body’s metabolic set point by eating healthy foods, making exercise a part of your routine and reducing stress

PFAS chemicals may make life easier — but they aren’t always so easy on the human body

While there’s little risk in trying this hair care treatment, there isn’t much science to back up the claims