Advertisement
This autoimmune disease can affect more than your skin
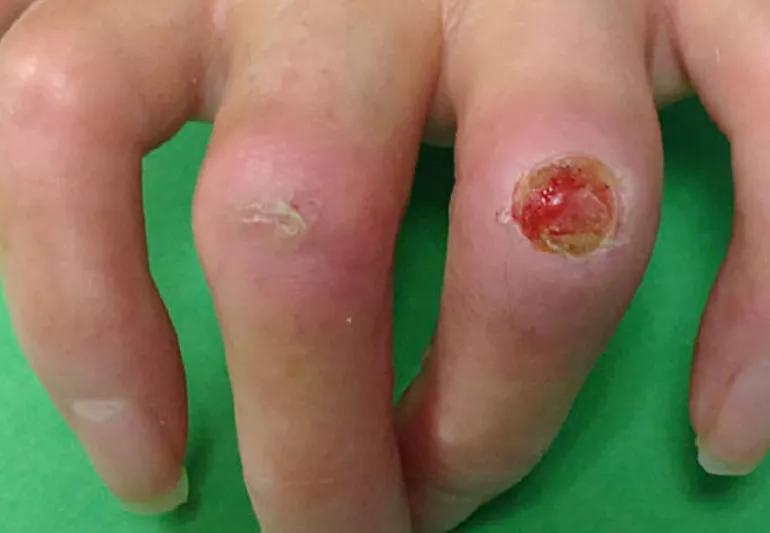
Scleroderma (also known as systemic sclerosis) is a chronic autoimmune disease. An estimated 300,000 Americans have scleroderma and of those, 100,000 have the systemic form. Most are women between the ages of 25 and 55.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
If you’ve never heard of scleroderma or are unsure of its presence, hardening of the skin is one of the most visible signs of this disease. Scleroderma most often affects the skin, but it can also affect many other parts of the body, including the digestive system, lungs, kidneys, heart, blood vessels, muscles and joints.
It’s a disease in which dense, thick fibrous tissue takes the place of normal tissue. This happens when your immune system triggers cells to overproduce collagen, a protein that provides strength and elasticity to skin, bone and other connective tissue. The extra collagen is deposited in the skin and organs, which causes hardening and thickening that is similar to scarring.
“Prompt and proper diagnosis and treatment may minimize the symptoms of scleroderma and lessen the chance of irreversible damage,” says pulmonologist Kristin Highland, MD.
“It is not uncommon for autoimmunity to run in families,” Dr. Highland says. For example, one person could have multiple sclerosis (MS), another could have scleroderma or lupus and yet another might have thyroid disease.
However, the risk is only slight. There is one exception in that the prevalence of scleroderma in the Choctaw Native Americans who originally settled in Oklahoma is quite increased. It’s important to share your family history with your physicians.
“There are multiple potential causes of shortness of breath in patients with scleroderma,” Dr. Highland says.
These include:
“Fatigue in scleroderma can be a result of multiple complications, and the management will depend on which of these complications is contributing most, such as anemia, thyroid disease, sleep apnea or Sjögren’s syndrome,” Dr. Highland says. It’s important to discuss this with your rheumatologist, who can figure out the cause of your fatigue and help address it.
Joint pain can be a result of inflammatory arthritis. If this is the case, medications are available to control it, and again this should be assessed by your healthcare provider before a decision can be made. Joint pain also can be a result of mechanical damage to the joints along with central pain from concomitant fibromyalgia. So the management of joint pain will depend on the cause of it.
“Gastrointestinal involvement can be quite different from patient to patients who have scleroderma,” Dr. Highland says. Symptoms can include:
Advertisement
Scleroderma can be tricky to diagnose, so it’s important to share any symptoms you are experiencing and any history of autoimmune disease in your family, with your doctor.
Advertisement
Learn more about our editorial process.
Advertisement

Treatments have improved outcomes for a condition once viewed as fatal

Research shows a strong association between rheumatoid arthritis and heart issues

An overactive immune system can be just as serious as one that stops working

The answer varies from person to person and vaccine to vaccine

Learn all you can, seek out support and don’t be afraid to advocate for yourself

From nausea, weight gain and eczema, stress can affect your immune system in many ways

This autoimmune disease can cause health issues ranging from mild to severe

Choose foods high in omega-3s and antioxidants; avoid red meat and dairy

Focus on your body’s metabolic set point by eating healthy foods, making exercise a part of your routine and reducing stress

PFAS chemicals may make life easier — but they aren’t always so easy on the human body

While there’s little risk in trying this hair care treatment, there isn’t much science to back up the claims