Gastric bypass and sleeve gastrectomy are different procedures that offer similar benefits, including significant weight loss
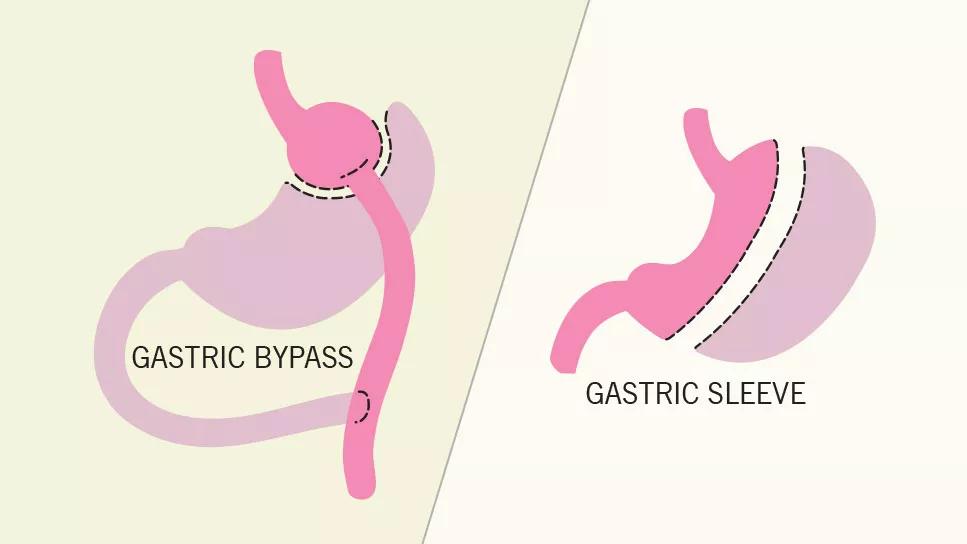
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/c5ca55b2-1b79-406d-9cda-598a102b8be7/gastric-Sleeve-Gastric-Bypass-bariatric-surgery-1348967549-967x544-1_jpg)
Two bariatric surgery options: grastric bypass and gastric sleeve
When you’re trying to live your healthiest life, trying to achieve a healthy weight is an important part of the equation. But it’s not always something you can do on your own.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Obesity is a medical condition, and not everyone can diet and exercise their way to a slimmer self. In these cases, bariatric surgery — also known as weight loss surgery or metabolic surgery — may be just what the doctor ordered.
“These procedures are the most effective treatment for obesity,” says bariatric surgeon Ali Aminian, MD. “They induce weight loss and influence your metabolism by changing your gastrointestinal (GI) physiology.”
But how can you decide which weight loss surgery is best for you? Dr. Aminian breaks down the options.
The two most common weight loss procedures are Roux-en-Y gastric bypass and sleeve gastrectomy. “Sleeve is a bit safer, while gastric bypass is a bit more effective,” Dr. Aminian says. “But both procedures help people lose large amounts of weight, and they both have profound metabolic effects.”
Gastric bypass surgery is an operation that shrinks your stomach, along with the amount of calories and fat your body absorbs. After gastric bypass surgery, any food you eat will enter your small intestine directly. It literally bypasses 90% to 95% of your stomach.
“We disconnect the top part of the stomach and make a small pouch there,” Dr. Aminian explains. “Then, we move the small intestine up and connect it to that pouch, which reroutes the GI tract.”
Advertisement
Sleeve gastrectomy surgery, on the other hand, is an operation on only your stomach. Surgeons remove around 80% to 85% of it, leaving a smaller “sleeve” in its place. “The shape of the stomach typically looks like a football,” Dr. Aminian illustrates. “After surgery, it looks more like a banana — narrow and tubular.”
For the most part, both procedures offer similar results and outcomes. Here are some of the benefits of bariatric surgery:
That said, there are some considerations that might tip the scales in favor of one over another. Dr. Aminian answers your questions about some of the differences between the two procedures.
Gastric bypass is a more powerful tool than sleeve gastrectomy and typically leads to losing more weight. On average, people who’ve had gastric bypass lose 10 to 25 pounds more than people who’ve had sleeve gastrectomy.
“For the most part, though, whichever procedure you have, most people are able to keep the weight off for a very long period of time,” Dr. Aminian says.
Sleeve gastrectomy is a bit safer than gastric bypass, Dr. Aminian says, but only by a little. “On the whole, these are extremely safe operations.”
The risk of all complications is 3% after sleeve gastrectomy versus 5% with gastric bypass. That means that for every 100 patients, three to five may develop post-surgical issues, like:
It’s a tie: Both procedures take about the same amount of time to recover from. Today’s surgeons perform almost all bariatric surgical procedures using minimally invasive techniques, which means smaller incisions and faster recovery time than ever before.
Advertisement
Both operations take about two hours to perform, and people typically stay in the hospital for one night, maybe two. “It usually takes about two or three weeks to recover,” Dr. Aminian adds, “and after that, you’re able to get back to your normal life.”
Gastric bypass is generally a slightly better option for people with diabetes because rerouting the GI tract leads to some hormonal changes that can increase your chances of diabetes improvement.
“In more than half of patients, diabetes goes into remission,” Dr. Aminian notes, “which means they don’t need any medications to control blood sugar for many, many years.”
Figuring out the right procedure for you requires an in-depth discussion between you and your bariatric surgeon. “Together, we’ll consider your medical history, conditions and expectations,” Dr. Aminian says. “Then, we come up with a plan together.”
Some medical conditions and concerns may mean that sleeve gastrectomy is the better choice for you, like if you:
Advertisement
Historically, bariatric surgery has been viewed as a last option for people with severe obesity. But within the last 20 years, the field has progressed significantly.
“These operations are much safer and more effective than ever,” Dr. Aminian clarifies, “and they’re not just for people with a severe form of disease. New guidelines mean that people with mild to moderate obesity are now also good candidates for bariatric surgery.”
Talk to a healthcare provider to learn whether bariatric surgery is a good fit for you.
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about our editorial process.
Advertisement
Body contouring can help trim excess skin
Maintaining a healthy weight, focusing on exercise and eating a well-balanced diet can improve your overall metabolic health
This diabetes medication can treat obesity, but it’s not for people who just want to drop a few pounds
Successful weight loss takes a long-term commitment — build a healthy lifestyle you can stick with
Overweight and obesity increase your CKD risk, and may speed disease progression in people who have the condition
Having a BMI in the healthy range doesn’t mean you’re safe from health conditions often associated with obesity
Having obesity can lead to pregnancy complications — be sure to eat more whole foods and try pregnancy-safe exercise
These medications can increase fertility — but the risk of taking them while pregnant isn’t well known
This ‘harm reduction’ approach to sobriety involves subbing one substance for another — a method that isn’t backed by research
Educate your child about body image, expectations and skin care first
A true chlorine allergy is extremely rare — it’s far more likely that you have a damaged skin barrier