From hyperactive immune response to disordered nerve connections, the itch is real

Those of us who live with eczema — the most common form of atopic dermatitis — can attest: When it comes to itchiness, the struggle is real.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
It’s so real, in fact, that it can make it hard to go about your day-to-day life. Because it’s a common condition, not all people treat eczema as the serious problem it is. But dermatologist Anthony Fernandez, MD, PhD, sees the toll eczema takes every day.
“Eczema itch impacts patients significantly, both physically and mentally,” he says. “It really affects every aspect of quality of life.”
Dr. Fernandez routinely sees people who have eczema:
Does that sound a bit extreme? Well, eczema itch is extreme! In fact, the itch eczema generates can be more severe than what you might experience from a bug bite or poison ivy.
We talked to Dr. Fernandez about why eczema itch is so dang itchy — and what you can do to stop it.
As anyone who lives with eczema knows, the dry skin, angry red rashes and swelling can be unbearable. Even mild cases of eczema can cause severe itching. Dr. Fernandez says that’s because eczema creates a perfect storm of itchiness.
Advertisement
“The main reason it’s so severe is the fact that there are multiple pathways that are all malfunctioning at the same time, which promotes the itch,” he explains.
When you have eczema, by definition you have damaged skin barriers, which promotes bacterial overgrowth. That bacterial overgrowth triggers an immune response. People with eczema tend to have hypersensitive immune systems, which become activated and release chemicals that cause itching inappropriately.
“Over time, the nervous system and the skin become sensitized and hyperactive,” Dr. Fernandez continues.
But wait, there’s more!
There’s a growing body of research suggesting there are disordered connections between the nerves in the skin of people with eczema that change how they send itching signals to their brains.
“So, when you have all of these systems malfunctioning at the same time, it ends up creating severe itch,” he adds.
As you’re probably realizing, itchiness is a fairly complex physiological experience. And there are actually two different kinds of itch, both of which you may experience when you have eczema.
Itchiness is the product of nerves transmitting signals from your skin to your brain. Neurogenic itch happens when those pathways get inappropriately activated.
Dr. Fernandez explains: “In people who don’t have eczema, the same stimuli would not cause itch. There isn’t damage to the nerves themselves, they’re just overactive.”
Meanwhile, psychogenic itch doesn’t originate in your skin — it originates in your brain. This phenomenon explains why hearing about somebody else having head lice immediately makes your head itchy (sorry), or why some people get itchy when they’re nervous.
Of course, if you scratch a psychogenic itch, the irritation to your skin could lead to neurogenic itching — especially if you have an existing dermatological issue like eczema.
As much as we all wish we could eliminate eczema itch with a good scratching session, that’s the worst possible thing you can do. Not only does scratching make the itch worse, but it can also lead to open sores, bacterial infections and pain.
Try these itch-relief tactics instead.
If you feel like you hear that advice a lot, it’s because you do. Dr. Fernandez notes, “That’s a knee-jerk reaction for dermatologists because it’s just about the safest thing you can do to get on top of itching.”
Moisturizing your skin with a sensitive-skin lotion or cream at least twice a day manages the itching you’re experiencing in the moment and helps prevent future flares. The best part: Many over-the-counter moisturizers are affordable and you don’t need to go to a physician to get them.
Advertisement
While you may not have purchased them for your eczema, you probably have a number of products sitting in your medicine cabinet or first-aid kit that could help tame the itching. Among them:
Your medicine cabinet isn’t the only place you can turn when you’re searching for eczema itch relief. Here are some of the most popular home remedies:
Advertisement
“Most of my patients say their itching is the worst at night,” Dr. Fernandez shares.
“We’re not exactly sure why this is, but one of the leading hypotheses is that people’s minds are really busy on the tasks of the day. That distraction may lead the itching to bother them less. But then at night, when there’s no other stimuli other than the itch, it becomes severe.”
If eczema itch is cutting into your beauty sleep, Dr. Fernandez recommends you:
If all else fails, you can minimize the risk of infection by keeping your hands clean and your nails trimmed.
Advertisement
This long list of eczema-itch elimination methods wouldn’t be complete without also noting that not all the advice you see on the internet is good advice. We asked Dr. Fernandez if there were any consistent mistakes people with eczema make in their fight against itchiness.
“The one thing that we see patients do over and over again — that stops us in our tracks — is they rub alcohol on their skin,” he recounts.
“They do that because they swear it helps their itching. And it may … in the very short term. The problem with alcohol is that it’s an irritant,” he continues.
“Over time, they’re going to impair their skin barrier worse than it was impaired before and stir up more inflammation, which makes the itching worse. It just leads to more problems in the future.”
The bottom line? There are plenty of reasons to keep rubbing alcohol on hand. Eczema isn’t one of them.
Because eczema is so common, it can be hard to know when the itch justifies a trip to your healthcare provider. Dr. Fernandez says the decision can vary based on your age. After all, 30% of all children under the age of 2 experience atopic dermatitis of some kind or another.
“Babies tend to have enough well checks that their primary care physicians will address it. But if what they’re doing to address it doesn’t seem to be helping, it’s probably wise to get an opinion from a dermatologist,” he advises.
Not only can the dermatologist determine whether or not your child’s rash actually is eczema, but they can also provide a more detailed treatment regimen to get your baby’s rash under control.
For older children and adults, the answer is a bit simpler: Dr. Fernandez encourages you to see a dermatologist any time the itching is affecting your quality of life, or when what you’re doing at home isn’t working anymore.
If you have mild eczema, your provider may prescribe:
If you have moderate to severe eczema, your provider may prescribe something more systemic, like:
No matter what treatment your provider decides is best for you, they’re also going to drive home these two messages: (1) don’t forget to moisturize and (2) don’t scratch!
Eczema itch is difficult to deal with because it’s the product of different bodily systems malfunctioning at the same time: your skin, your immune system, your nerves and your brain.
For immediate itch relief, look to your medicine cabinet. If home remedies and common approaches to fighting itch aren’t solving the problem — or if the itch is severe enough that it’s impacting your quality of life — it’s time to talk to your doctor about more aggressive treatment options.
Whatever you do, just don’t scratch!
Learn more about our editorial process.
Advertisement

Colloidal oatmeal, petroleum jelly and other around-the-home products can help provide needed relief

Your body’s natural response to stress can lead to painful skin irritation

Eczema triggers are different for everyone, but there are some common ways to manage and prevent flare-ups

Hot or cold, your eczema can have flare-ups during multiple times of the year

Keep your showers short and lukewarm, and moisturize promptly after with a cream containing ceramides
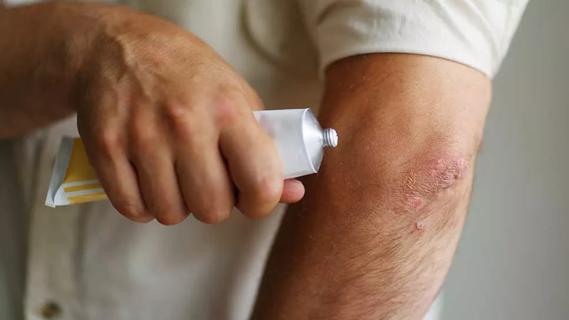
Steroids, self-injections and medications can be game changers
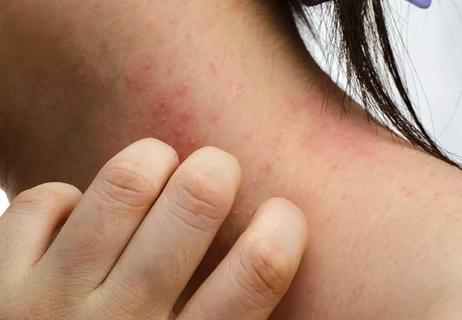
Changing your wardrobe or environment won’t eliminate eczema, but it can help reduce flares
Ingredients to look for and ones to avoid

If you’re feeling short of breath, sleep can be tough — propping yourself up or sleeping on your side may help

If you fear the unknown or find yourself needing reassurance often, you may identify with this attachment style

If you’re looking to boost your gut health, it’s better to get fiber from whole foods