Reducing inflammation is key when you’re in a flare-up, but so is having a preventive nutritional plan in place when you’re not

A diagnosis of diverticular disease might bring up a lot of questions and concerns. What are you allowed to eat? Are there foods you should avoid? Will your symptoms go away on their own, or will you feel this way forever?
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Searching for answers can be just as confusing. With a lot of misinformation and myths around the differences between diverticulosis and diverticulitis, where do you even begin?
According to registered dietitian Anna Taylor, RD, LD, you want to focus your diverticulitis diet on reducing inflammation and severity of symptoms whenever you’re caught in the middle of a flare-up. But you also want to be preventive when you’re not having a flare-up by building out an eating plan that works for you and your digestive tract.
Taylor clears up the confusion about how to manage both halves of the diverticular disease equation and provides answers about what foods you may or may not want to eat if you’re dealing with these conditions.
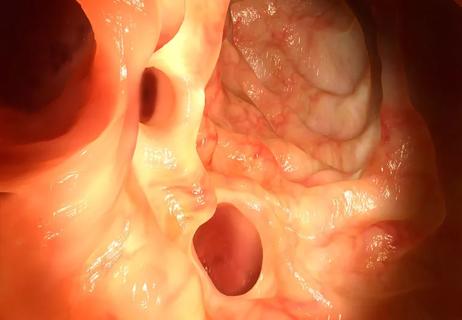
When you have diverticulosis, little pouches or pockets form on the inside lining of your intestines and your colon. These pockets, called diverticula, are relatively harmless on their own. You can think of them as freckles or skin tags. They’re usually not a problem unless they get irritated or infected — and when this happens, it’s called diverticulitis.
When these pockets become infected or injured, it can cause inflammation to build up inside those pockets that can then spread to other areas of your colon. During these flare-ups, you’ll likely experience:
Advertisement
It’s possible to have diverticulosis without ever developing diverticulitis. So, the key to preventing flare-ups is making sure your diet doesn’t cause any additional inflammation or injury when you have diverticulosis. And when you’re having a flare-up because of diverticulitis, your diet should change to decrease the severity of your symptoms and allow your intestines to recover.
“When you have diverticulitis, those pockets in your intestinal wall are upset, inflamed and maybe even infected. So, we want to reduce traffic in your gastrointestinal tract so that nothing else irritates them,” explains Taylor. “Decreasing the fiber in your diet helps with that.”
During a diverticulitis flare-up, your provider may recommend rest, antibiotics and either a clear liquid or low-fiber diet so your colon can rest and recover until the flare-up has passed.
If a diverticulitis flare-up is severe or requires surgery, your doctor may recommend a clear liquid diet. “After a day or two, you progress from clear liquids to a low-fiber diet,” says Taylor. “Even if your pain doesn’t subside, you still move toward regular food. You can’t be on a liquid diet long term because you can become malnourished.”
On a clear liquid diet, you can eat:
For milder cases of diverticulitis flares, eat a low-fiber or GI soft diet. A low-fiber diet limits fiber intake to between 8 and 12 grams of fiber, depending on the severity of the flare-up.
Good low-fiber food options include:
Advertisement
Foods to avoid with diverticulitis include high-fiber options such as:
You’ll want to follow this low-fiber diet until your diverticulitis symptoms subside. “Usually, someone starts to improve after several days of being on antibiotics,” Taylor says.
If you do, your provider will have you gradually increase your fiber intake over several days to weeks to avoid constipation and bloating.
“The goal is getting back to a high-fiber diet to decrease your risk for future bouts of diverticulitis,” she adds. “But if you’re not feeling better within a few days, talk to your provider.”
But what if you’re not having a flare-up of diverticulitis? What can you do to prevent flare-ups from happening in the future? Constipation often contributes to the development of diverticula. Hard, stuck stools may also irritate or injure those pockets lining the walls of your colon, which can cause flare-ups to reoccur over time.
“People develop diverticula due to years of excessive muscular contractions as the body attempts to move small, hard stools,” explains Taylor. A high-fiber diet helps fight constipation by softening stool, which then moves through your gastrointestinal (GI) tract more comfortably and easily. There’s also less pressure against those pockets, which helps prevent diverticulitis flare-ups.
Advertisement
A high-fiber diet typically includes 25 to 35 grams of fiber per day. You can work that into your nutritional plan by choosing minimally processed plant foods such as:
Years ago, doctors thought that if you ate corn, popcorn, nuts and seeds, those tiny components could get caught inside the pockets along your intestines, causing them to become inflamed so that you developed diverticulitis. But there’s no research to support that theory.
“It’s safe to eat these types of foods, including tomatoes and strawberries with seeds,” Taylor notes. “All that normal roughage and fiber is fine.”
To get the most out of a high-fiber diet, she also recommends:
“Diverticular disease may be common in Western societies because our diets are so low in fiber,” Taylor says. “Americans, on average, eat around 14 grams each day — about half of what’s recommended.”
Advertisement
If you’re not having a flare-up or experiencing any symptoms, you should limit low-fiber foods, red meat and other food triggers that cause you GI upset.
If you’re having a flare-up and are experiencing symptoms, you should avoid high-fiber foods until your symptoms subside or your healthcare provider gives you the all-clear.
It may sound confusing on the surface, but it’s two sides to the same coin. Once you’re more in tune with how your body reacts to certain foods, and you’re able to identify your food triggers, living with diverticular disease becomes much more manageable. Keeping a food journal might help track your symptoms and triggers. But you’ll also want to talk to your doctor about a long-term plan.
And if you’ve recently been diagnosed with diverticular disease, meet with a dietitian to learn practical and sustainable ways to get more fiber into your diet.
“Dietitians can also give you more specific recommendations to feel better during a diverticulitis flare-up,” encourages Taylor.
Learn more about our editorial process.
Advertisement

It’s not an enema or bowel prep, and this colonic hydrotherapy can harm proper colon function

Some symptoms you can treat at home, but others require a visit to the doctor

TikTok trend encourages eating papaya seeds to ‘deworm’
The short answer from a colorectal surgeon

People with PKU need to avoid high-protein foods, like meat, dairy, legumes and whole grains

The caffeine and natural acids in coffee may trigger acid reflux, but there are ways to lessen the effects

Olive oil is high in heart-friendly unsaturated fats

The tropical fruit is a good source of antioxidants and vitamin C

The tropical fruit is a good source of antioxidants and vitamin C

Most people fall asleep within 10 to 20 minutes, but if your experience is different, adjusting your sleep schedule may help

Exploring your hidden side can lead to better understanding of what makes you tick