Your genes, family history and anatomy can all influence obstructive sleep apnea — but lifestyle factors can, too
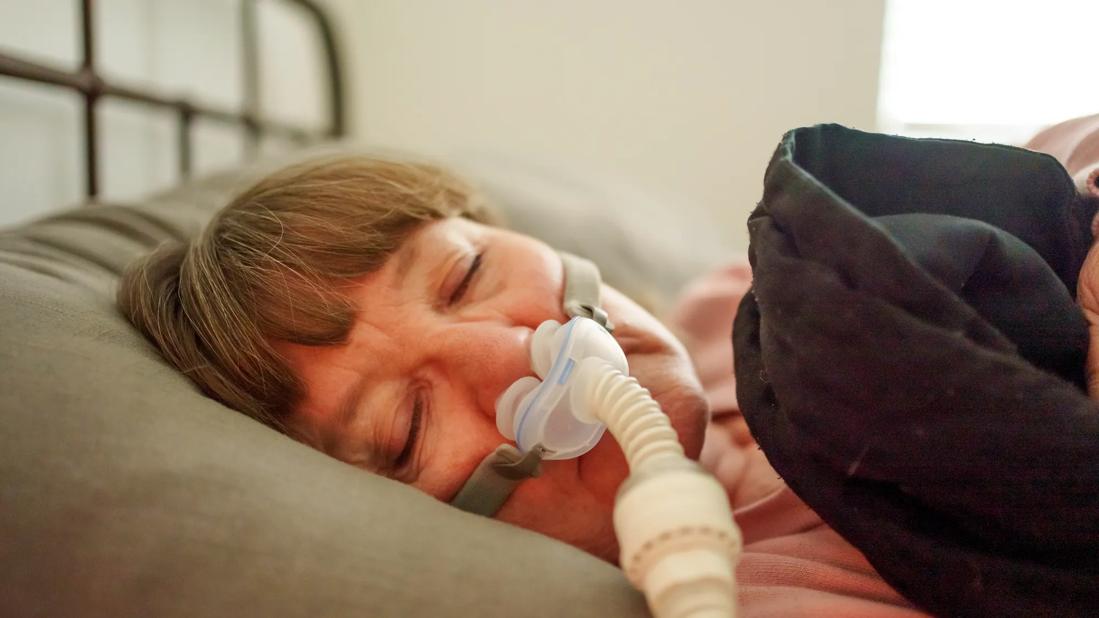
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/2d72a00f-1c17-416b-b3de-ab603d16c49e/sleep-apnea-machine-2191888530)
Older person sleeping with a continuous positive airway pressure machine, CPAP
If it seems like sleep apnea runs in your family, you’re not imagining it.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Sleep medicine specialist Cinthya Pena Orbea, MD, explains how certain genetic factors may increase your risk for this sleep disorder.
Obstructive sleep apnea (OSA) is the most common form of sleep apnea — and it has a strong genetic and hereditary component.
“Your genes can influence traits that make your airway more likely to collapse during sleep,” Dr. Pena Orbea explains. “In fact, inherited factors may account for as much as 30% to 70% of OSA risk.”
Central sleep apnea is a less common form of sleep apnea. And it’s not genetic.
“This type of sleep apnea is commonly secondary to other diseases and medications,” she says.
That means it’s usually linked to underlying medical conditions (like heart conditions or neurological disorders) or medications that affect breathing signals in the brain. It’s also more common in people living at high altitudes.
Genetics can influence several key risk factors for obstructive sleep apnea, many of which affect how your airway functions while you sleep. Dr. Pena Orbea walks us through them.
Research shows that genetics plays a big role in your likelihood of developing obesity. And when it comes to your chances of having sleep apnea, that’s important — because obesity is one of the biggest risk factors for OSA.
Advertisement
“Extra fatty tissue around the neck can narrow your airway, while abdominal fat can prevent your lungs from fully expanding,” Dr. Pena Orbea says.
Research shows that people with obesity are more than 10 times as likely to have obstructive sleep apnea. In one study, 70% of people awaiting bariatric surgery were found to have OSA, and 40% of them were considered to have severe OSA.
“Craniofacial anatomy” refers to your skull and the bone structure of your face. And it can contribute to OSA.
“The shape and size of your facial skeleton and airways can be inherited,” Dr. Pena Orbea explains. “And certain features are risk factors for OSA because they can make your airway less open during sleep.”
These may include:
Some people inherit differences in how their brains regulate breathing. These subtle changes can make the airway more prone to collapsing at night.
“Those inherited differences can raise your overall risk of obstructive sleep apnea,” Dr. Pena Orbea confirms.
If you have close biological relatives who have OSA, your risk is higher, especially if you share similar physical traits or health patterns.
“We use a scale called the Apnea-Hypopnea Index (AHI) to measure the number of times a person’s airway collapses during sleep,” Dr. Pena Orbea explains. “Data shows that nearly 40% of variance in a person’s AHI score may be explained by familial factors.”
Some health conditions run in families, and they can raise your risk of obstructive sleep apnea. These include:
There’s no single “sleep apnea gene.” But researchers have identified groups of genes that may contribute to a higher risk of OSA.
These are genes that generally affect:
“Many of these genetic influences work together,” Dr. Pena Orbea notes. “That’s why obstructive sleep apnea is considered a complex, multifactorial condition, not something that’s caused by one gene alone.”
You’re two to four times more likely to have obstructive sleep apnea if you have close biological relatives who have the condition. But that doesn’t mean you’re destined for it.
Advertisement
Dr. Pena Orbea explains that maintaining a healthy weight through regular physical activity and balanced nutrition can help lower your risk, even if sleep apnea runs in your family.
“You can’t change your genetics or your craniofacial structure,” she acknowledges. “But you may be able to make meaningful changes to your body weight that can help lower your risk of obstructive sleep apnea.”
Obesity is the most significant modifiable contributor to OSA. Data shows that a 20% decrease in body mass index (BMI) is associated with a 57% decrease in AHI score.
Of course, weight loss can be complex and nuanced, too — and often, certainly easier said than done. But you don’t have to do it alone. Your healthcare provider can help you come up with a personalized plan that may include strategies like:
Though there’s often a genetic component to obstructive sleep apnea, it’s usually a mix of inherited traits and lifestyle factors — which means there are things you can do to help lower your risk and improve your overall health.
“If you have a family history of OSA, talk to your healthcare provider,” Dr. Pena Orbea advises. “They’ll walk you through ways to manage your risk, explain potential symptoms to watch for and talk about whether you should be evaluated for sleep apnea.”
Advertisement
Advertisement

Sign up for our Health Essentials emails for expert guidance on nutrition, fitness, sleep, skin care and more.
Learn more about our editorial process.
Advertisement
Obstructive sleep apnea can lead to high blood pressure — and vice versa
People with PKU need to avoid high-protein foods, like meat, dairy, legumes and whole grains
Sleep disorders, mental health conditions and other health concerns can all affect the quality of your sleep
You’ll work with your provider to weigh the pros and cons of different medications
Stress, dental work and repetitive motions are just a few of the many HAE triggers
People with sickle cell trait have one copy of an abnormal gene — people with the disease have two
Mouth taping may seem promising, but it can actually cause more harm than good, especially if you snore or have sleep apnea
Pain, light exposure and anxiety are just a few factors that could be waking you up in the middle of the night
The virus that causes the so-called ‘stomach flu’ can cling to surfaces for days or even weeks
There isn’t clear evidence that melatonin harms your heart — but finding the cause of sleep issues is key to long-term heart health
Your dollar bills, coins and cards are covered in germs — but they’re very unlikely to make you sick